SDB Basics - Night Noises 101
- Sleep Disordered Breathing (SDB): Spectrum of breathing abnormalities during sleep.
- Obstructive Sleep Apnea (OSA): Airway obstruction despite respiratory effort.
- Central Sleep Apnea (CSA): Absent respiratory effort.
- Mixed Apnea: Central onset, then obstructive component.
| Feature | OSA | CSA |
|---|---|---|
| Airway | Obstructed | Patent |
| Respiratory Effort | Present/↑ | Absent/↓ |
- Mild: **5-15/hr**
- Moderate: **15-30/hr**
- Severe: **>30/hr**
⭐ AHI is the number of apneas and hypopneas per hour of sleep.

OSA Mechanics - Airway Antics
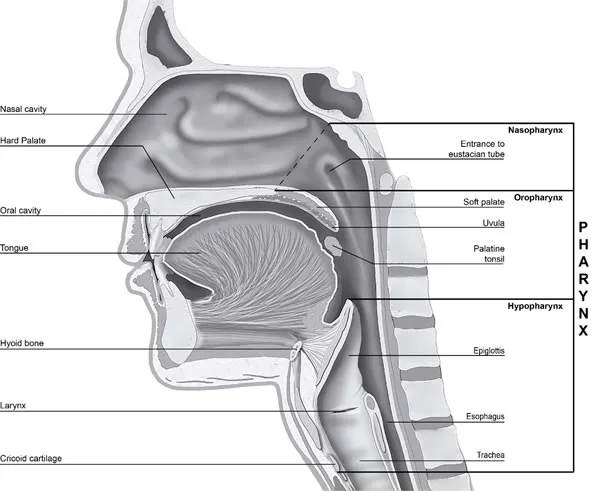
- Anatomical Factors (Narrowing the Stage):
- Bony: Retrognathia.
- Soft Tissue: Macroglossia, tonsillar/adenoidal hypertrophy, elongated/floppy soft palate/uvula, lateral pharyngeal wall thickening (fat deposition).
- Neuromuscular Dysfunction (Guard Duty Failure):
- ↓ Activity of upper airway dilator muscles (e.g., genioglossus, tensor palatini) crucial for patency, especially during REM sleep.
- Airway Collapse Dynamics:
- Inspiratory Suction: Negative intrathoracic pressure during inspiration exacerbates collapse.
- Venturi Effect: Airflow accelerates at narrow points, ↓ lateral pressure, promoting closure.
- Starling Resistor: Airway behaves like a collapsible tube; upstream/downstream pressures and wall compliance dictate patency.
⭐ The oropharynx, particularly the velopharynx, is the most common site of collapse in OSA.
CSA Central - Control Chaos
- Definition: Airflow cessation from absent/reduced respiratory effort.
- Primary CSA:
- Idiopathic.
- Cheyne-Stokes Respiration (CSR): cyclic crescendo-decrescendo breathing, central apneas.
- Secondary CSA:
- Medical conditions: heart failure, stroke, renal failure.
- High altitude.
- Drugs: opioids, sedatives.
- CSR Pathophysiology: Ventilatory instability from:
- ↑ Circulatory delay (e.g., heart failure).
- ↑ Chemosensitivity (high loop gain).
- Unstable chemoreceptor-respiratory center feedback.
⭐ Cheyne-Stokes respiration is commonly associated with advanced congestive heart failure.
SDB Fallout - System Shockers
Recurrent apneas/hypopneas unleash widespread systemic damage:
- Immediate Insults:
- Intermittent hypoxemia & hypercapnia.
- Marked intrathoracic pressure swings.
- Recurrent arousals disrupting sleep architecture.
- Hypoxemia/Reoxygenation Damage:
- Leads to oxidative stress.
- Promotes systemic inflammation (evidenced by ↑CRP, TNF-α, IL-6).
- Sleep Fragmentation Effects:
- Excessive Daytime Sleepiness (EDS).
- Cognitive impairments (e.g., attention, executive function).
- Mood disturbances (e.g., depression, anxiety).
- Cardiovascular Storm:
- Chronic sympathetic activation & endothelial dysfunction.
- Results in: systemic hypertension, arrhythmias (notably Atrial Fibrillation), Ischemic Heart Disease (IHD), stroke, and pulmonary hypertension.
- Metabolic Meltdown:
- Insulin resistance, predisposing to Type 2 Diabetes Mellitus.
- Dyslipidemia.
- Key contributor to Metabolic Syndrome.

⭐ Obstructive Sleep Apnea (OSA) is an independent risk factor for systemic hypertension.
High‑Yield Points - ⚡ Biggest Takeaways
- Upper airway collapse during sleep is central to OSA pathophysiology.
- Key consequences include intermittent hypoxia, hypercapnia, and sleep fragmentation.
- Increased negative intrathoracic pressure during obstructed breathing efforts.
- Obesity is a major risk factor, causing ↑ pharyngeal soft tissue.
- Craniofacial abnormalities (e.g., retrognathia) can predispose to collapse.
- Impaired neuromuscular control of upper airway dilator muscles is crucial.
- Leads to sympathetic activation, oxidative stress, and systemic inflammation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


