Introduction to Outcomes Assessment - Gauging Surgical Gains
- Primary Goal: Systematically measure the success of surgical interventions for snoring and Obstructive Sleep Apnea (OSA).
- Critical For:
- Guiding appropriate patient selection.
- Refining surgical techniques for better results.
- Comparing the effectiveness of various procedures.
- Foundation Of: Evidence-based practice in sleep surgery, ensuring quality care and justifying treatments.
- Utilizes both subjective (e.g., Epworth Sleepiness Scale) and objective (e.g., Polysomnography - PSG) data.
⭐ Polysomnography (PSG) is the gold standard for objectively quantifying OSA severity and treatment efficacy, primarily via the Apnea-Hypopnea Index (AHI).
Subjective Assessment Tools - Hearing Patient Stories
- Patient-Reported Outcome Measures (PROMs) capture symptomatic relief and Quality of Life (QoL) changes.
- Key Instruments:
- Epworth Sleepiness Scale (ESS): Quantifies average daytime sleepiness. Score >10 suggests excessive sleepiness.
- Functional Outcomes of Sleep Questionnaire (FOSQ-10): Assesses impact of sleepiness on daily activities; 10-item version.
- Snoring Scales: e.g., Visual Analog Scale (VAS) for snoring loudness/frequency.
- Sleep Apnea Quality of Life Index (SAQLI): OSA-specific QoL measure.
- Patient diaries: Subjective record of sleep patterns, symptoms.
⭐ A reduction of 2-4 points in ESS score is often considered a clinically significant improvement after sleep surgery.
 oka
oka
Objective Assessment Tools - Data-Driven Verdicts
- Polysomnography (PSG): Gold standard pre- & post-op.
- Key Metrics for Outcome Assessment:
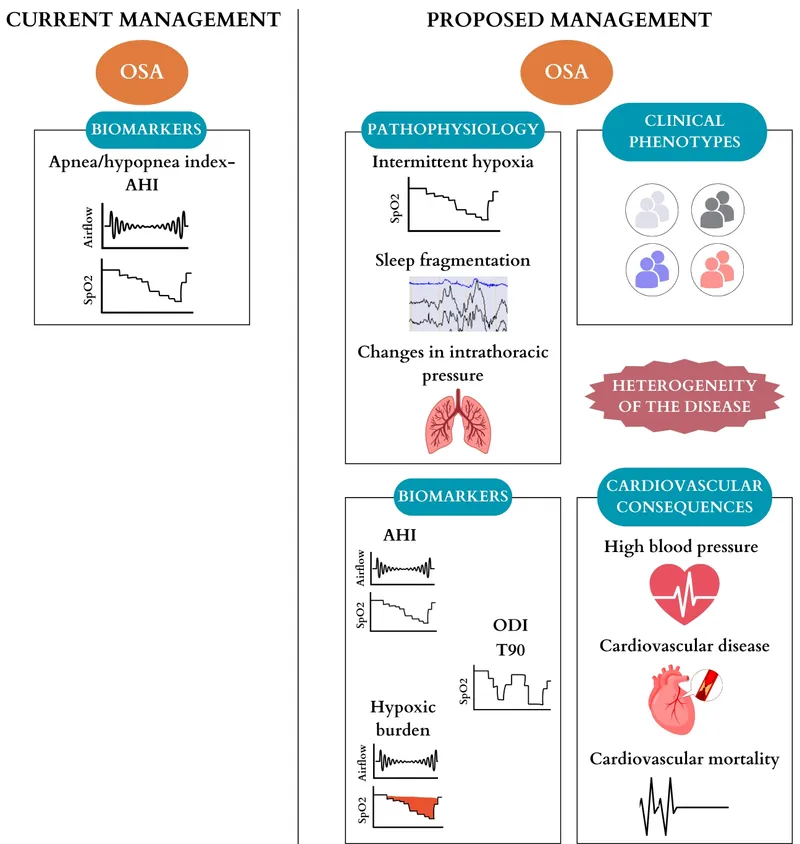
- Apnea-Hypopnea Index (AHI): Target ↓. (Severity: Mild 5-14/hr, Mod 15-29/hr, Sev ≥30/hr).
- Oxygen Desaturation Index (ODI): Target ↓ (for ≥3-4% drops).
- Nadir SaO2 (Lowest O2 saturation): Target ↑.
- Sleep Architecture: Improved efficiency, ↑REM, ↑Slow-Wave Sleep.
- Key Metrics for Outcome Assessment:
- Home Sleep Apnea Testing (HSAT): Portable option for post-op evaluation in selected patients.
- Monitors AHI/RDI, O2 desaturations.
⭐ Surgical success often defined by AHI reduction ≥50% AND post-op AHI <20/hr (Sher's criteria).
Surgical Success Criteria - Defining Surgical Triumph
- Primary Goal: ↓AHI, improve symptoms (snoring, Epworth Sleepiness Scale [ESS]).
- Sher Criteria (Classic Success):
- Post-op Apnea-Hypopnea Index (AHI) < 20/hour.
- AHI reduction ≥ 50% from baseline.
- Subjective improvement (ESS, snoring).
- Surgical Cure: Post-op AHI < 5/hour.
- Flowchart: Sher Criteria Application
⭐ Achieving a post-operative AHI < 5 is often considered a surgical "cure" for OSA.
Long-Term Follow-up & Challenges - The Enduring Picture
- Crucial: Periodic clinical assessment & objective sleep studies (e.g., PSG at 1, 3, 5 years).
- Surgical outcomes may diminish over time; vigilance for symptom return is key.
- Major Hurdles:
- Patient adherence to follow-up schedules.
- Standardizing definitions of long-term success (AHI, Patient-Reported Outcomes (PROs)).
- Addressing impact of aging and weight fluctuations.
- OSA management is a marathon, not a sprint.
⭐ Significant weight gain (>10% body weight) is a primary predictor of OSA recurrence after surgery.
High‑Yield Points - ⚡ Biggest Takeaways
- Polysomnography (PSG): Gold standard for OSA diagnosis and post-operative outcome assessment.
- Apnea-Hypopnea Index (AHI): Key objective metric for OSA severity and evaluating treatment success.
- Epworth Sleepiness Scale (ESS): Quantifies subjective daytime sleepiness, a crucial patient symptom.
- PROMs (e.g., FOSQ): Vital for assessing quality of life changes after surgical intervention.
- DISE: Aids in surgical planning by identifying specific upper airway obstruction sites.
- Surgical Success: Typically ≥50% AHI reduction plus post-operative AHI <20/hr and symptom relief.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

