Auricular Hematoma - Ear's Blood Blister
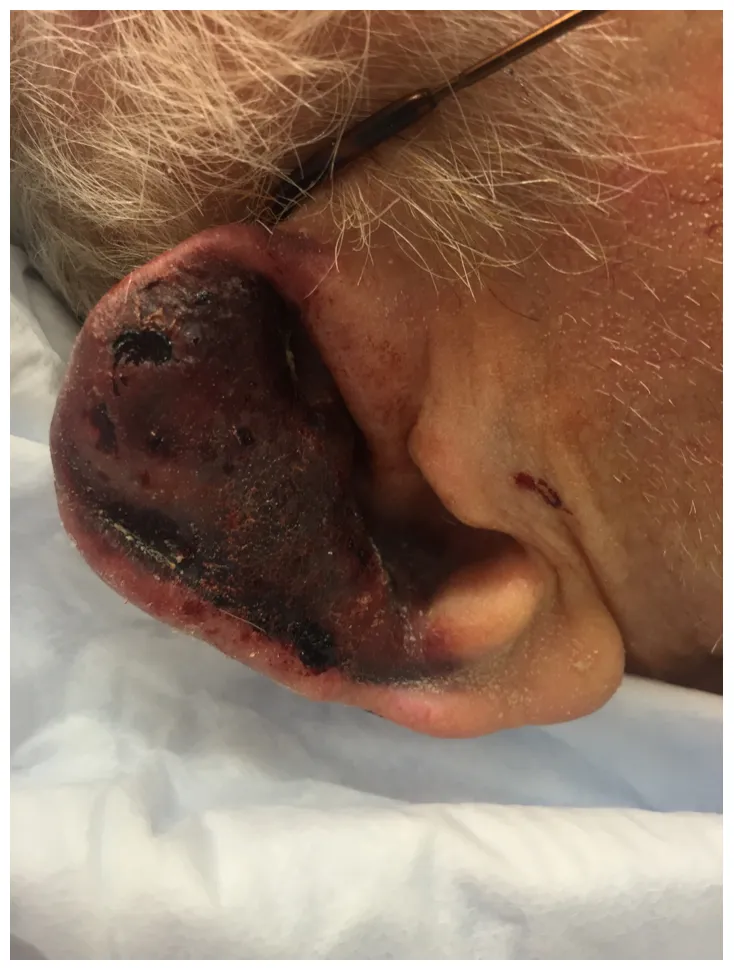
⭐ Auricular hematoma is a collection of blood between the auricular cartilage and its overlying perichondrium.
- Etiology: Commonly due to blunt trauma (e.g., wrestling, boxing, rugby).
- Pathophysiology: Shearing forces separate cartilage from perichondrium, causing blood to pool. This compromises cartilage nutrition.
- Clinical Features: Tender, fluctuant, bluish swelling on the auricle, obscuring normal contours.
- Complications: Untreated hematomas can lead to
Mechanism & Mayhem - How It Happens
Direct trauma or shearing forces to the auricle initiate the cascade:
⭐ Shearing forces are the primary culprits, leading to separation of the perichondrium from the underlying avascular cartilage.
This cartilage relies on the overlying perichondrium for its viability.
Spotting the Swelling - Signs & Symptoms
- Onset: Develops within hours (typically 2-24 hours) post-trauma to the ear.
- Appearance:
- Smooth, tense, fluctuant swelling on the auricle.
- Bluish or erythematous discoloration.
- Loss of normal auricular contours.
- Location: Most common on the anterior surface, between cartilage and perichondrium (e.g., scaphoid fossa, concha).
- Symptoms:
- Pain, often significant and throbbing.
- Tenderness on palpation.
- Sensation of pressure or fullness.

⭐ A key diagnostic feature is a fluctuant, tender swelling on the auricle, typically appearing hours after trauma.
Drain & Defend - Treatment Tactics
- Goal: Evacuate hematoma, prevent re-accumulation & infection, preserve cartilage.
- Intervention Timing:
- Ideal: Within 24-72 hours.
- Acceptable: Up to 7 days post-injury.
- Procedures:
- Needle Aspiration: For small, acute hematomas (<2 cm, <24-48 hours old).
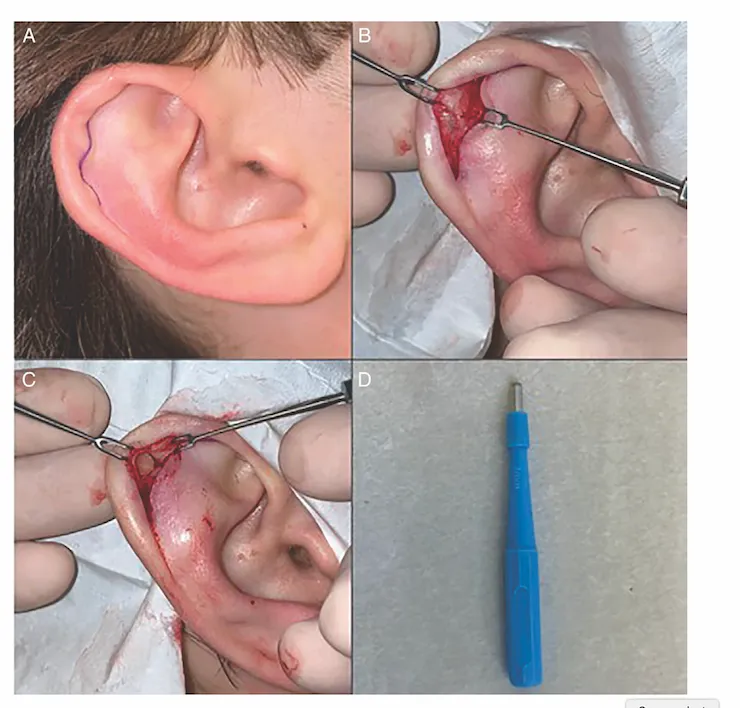
- Incision & Drainage (I&D): For larger, older, or recurrent hematomas.
- Curvilinear incision along skin crease.
- Evacuate clot, irrigate.
- Pressure Dressing (Crucial):
- Conforming dressing to prevent dead space & re-accumulation.
- Methods: Dental rolls (bolsters), buttons, silicone splints, mattress sutures.
- Maintain for 5-7 days.
- Antibiotics:
- Prophylactic anti-staphylococcal (e.g., Flucloxacillin, Clindamycin) for 7-10 days.
- Follow-up:
- Regular checks for re-accumulation or infection.
⭐ Prompt drainage (ideally within 24-72 hours, but acceptable up to 7 days) and application of a conforming pressure dressing are crucial to prevent cauliflower ear.
Cauliflower Calamity - Risks & Safeguards
- Risks of Neglect:
- Cartilage necrosis, perichondritis/abscess.
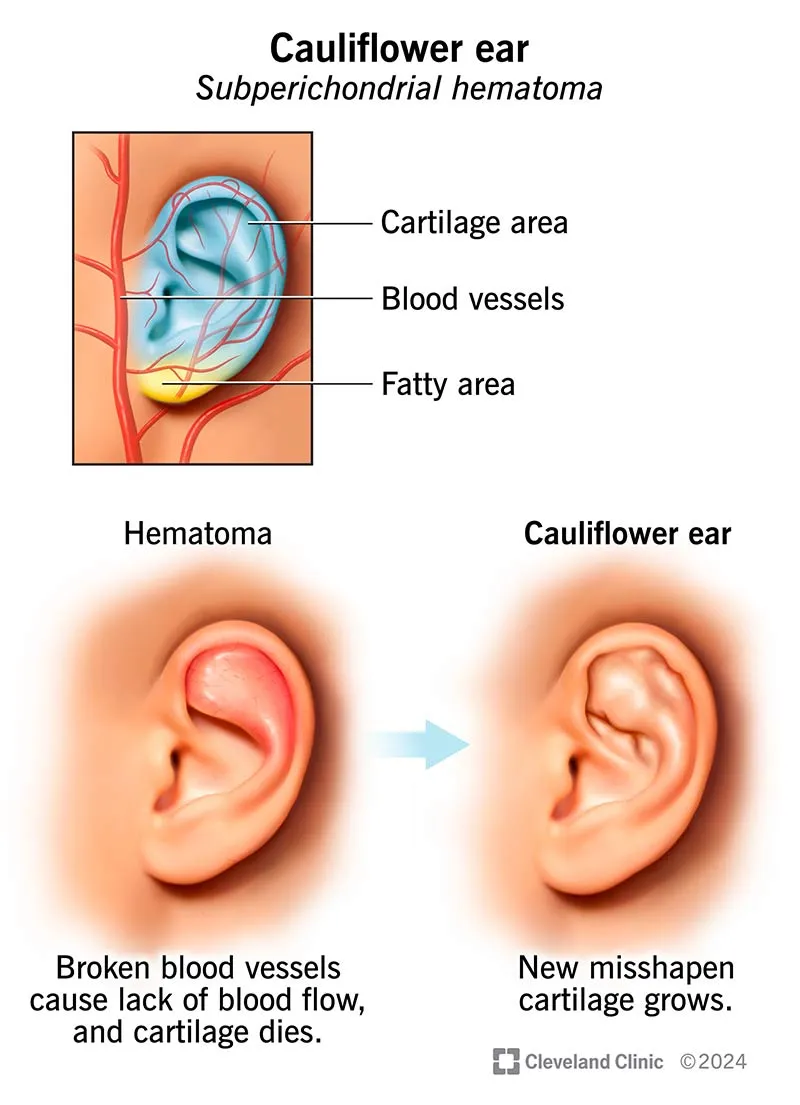
- Permanent "Cauliflower Ear" deformity.
- Cosmetic & functional impairment.
- Hematoma recurrence.
- Key Safeguards:
- Urgent drainage (ideally <48h, max 7 days).
- Strict asepsis.
- Effective pressure dressing (bolsters/buttons).
- Consider antibiotics (e.g., anti-staphylococcal).
- Vigilant follow-up.
⭐ Cauliflower ear (perichondrial chondroneogenesis) results from cartilage ischemia, inflammation, and subsequent disorganized fibrocartilage formation if the hematoma is not evacuated.
High-Yield Points - ⚡ Biggest Takeaways
- Auricular hematoma: Blood collection between auricular cartilage and its perichondrium.
- Typically results from blunt trauma (e.g., contact sports).
- Risk of cauliflower ear (fibrocartilaginous deformity) if untreated due to cartilage necrosis.
- Urgent drainage (ideally < 48 hours, max 7 days) prevents deformity.
- Management: Incision & Drainage followed by a compressive pressure dressing.
- Maintain strict asepsis to avoid perichondritis, a serious complication.
- Reaccumulation is common without adequate, sustained pressure post-drainage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

