CI Basics - Bionic Ear 101
- Definition: A cochlear implant (CI) is a surgically implanted electronic device. It provides a sense of sound to individuals with severe-to-profound sensorineural hearing loss (SNHL).
- Mechanism: CIs bypass damaged cochlear hair cells. They directly stimulate auditory nerve fibers (spiral ganglion cells) using electrical impulses.
- Key Components:
- External: Microphone, speech processor, transmitting coil.
- Internal: Receiver-stimulator (implanted subcutaneously), electrode array (inserted into scala tympani of cochlea).
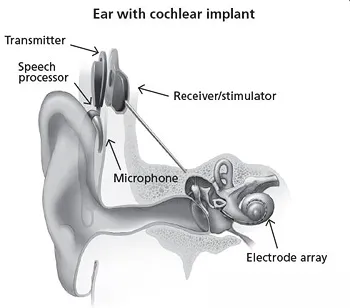
- Signal Path: Sound → Microphone → Speech Processor → Transmitter (external) → Receiver (internal) → Electrode Array → Auditory Nerve → Brain.
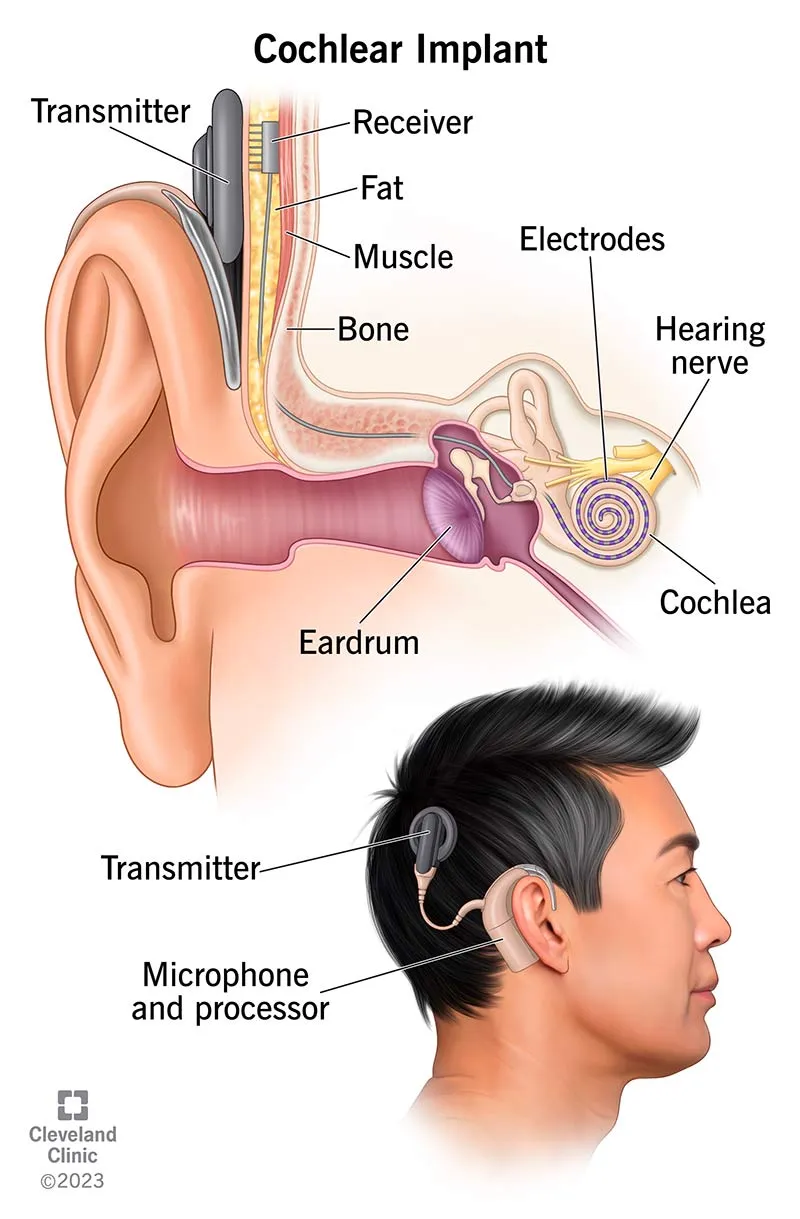
⭐ Cochlear implants directly stimulate spiral ganglion cells (auditory nerve fibers) within the cochlea.
CI Candidacy - Green Light Ears
CI is for those with significant hearing loss not adequately helped by hearing aids. "Green light" indicates strong candidacy.
- Key Audiological Thresholds:
- Adults: Bilateral severe-profound SNHL (PTA >70 dB HL). Speech recognition ≤50% (implanted ear) or ≤60% (best-aided).
- Children (12-24m): Bilateral profound SNHL (PTA ≥90 dB HL). Limited auditory progress with HAs.
- Children (>24m): Bilateral severe-profound SNHL. Speech scores (e.g., MLNT/LNT) ≤30%.
- Essential Anatomy: Patent cochlear duct, identifiable auditory nerve (CN VIII).
- Overall Status: No active middle ear disease, fit for surgery, strong motivation, and realistic expectations.
⭐ For pre-lingually deafened children, implantation before 2 years of age (ideally <18 months) yields best speech/language outcomes.
CI Workup & Surgery - Journey to Sound
Comprehensive Workup:
- Audiological: PTA, Speech Discrimination Score (SDS) < 50% (aided), OAE, ABR, EABR. Promontory stimulation test (PST) for nerve viability.
- Radiological: HRCT Temporal Bone (cochlear patency, ossification, anomalies), MRI (CN VIII integrity, labyrinthine fluid).
⭐ HRCT is crucial to assess cochlear duct patency (e.g., for cochlear aplasia/hypoplasia) & identify anomalies like Mondini dysplasia.
- Medical fitness, psychological assessment, realistic expectations.
- Vaccinations: Pneumococcal, H. influenzae type b, Meningococcal.
Surgical Pathway:
- Facial Recess: Bounded by Chorda tympani (lat), Facial N. (med), Fossa incudis (sup). 📌 "CN VII sandwich"
- Post-op: Auditory rehabilitation, regular mapping.
Post-CI & Outcomes - Switched On Life
- Switch-on: Typically 2-4 weeks post-operatively.
- Mapping (Programming): Regular audiologist sessions to program T-levels (threshold) & C/M-levels (comfortable/maximum) for each electrode.
- Auditory Rehabilitation: Intensive therapy (audiologist, Speech Language Pathologist - SLP) is KEY. Focus on:
- Listening skills development.
- Speech discrimination & production.
- Outcomes:
- Significant ↑ in speech perception (open-set & closed-set scores).
- Improved hearing in noise & sound localization (especially with bilateral CIs).
- Enhanced Quality of Life (QoL).
- Favorable Prognostic Factors:
- Younger age at implantation (esp. pre-lingual <2 years).
- Shorter duration of profound deafness.
- Consistent device use & commitment to rehabilitation.
- Good cochlear nerve status & cognitive abilities.
- Long-term Considerations: Monitor for device malfunction/failure, electrode migration; potential for reimplantation.

- ⭐ > For prelingually deaf children, implantation before 18 months of age is associated with the best prognosis for developing age-appropriate speech and language skills.
High‑Yield Points - ⚡ Biggest Takeaways
- Indicated for bilateral severe-to-profound SNHL with poor hearing aid benefit.
- Requires patent cochlea (especially scala tympani) and functional auditory nerve.
- Electrode array inserted into scala tympani, commonly via round window or cochleostomy.
- Post-operative mapping (NRT, ART) and intensive auditory-verbal therapy are crucial.
- Minimum age typically 12 months; earlier if post-meningitic ossification risk.
- Key contraindications: Michel aplasia, auditory nerve aplasia, active otitis media.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

