Intro & Pathogenesis - Schwann's Surprise
- Benign tumor from Schwann cells (PNS myelin) of vestibulocochlear nerve (CN VIII).
- Aka Vestibular Schwannoma.
- Most common Cerebellopontine Angle (CPA) tumor (~80-90% of CPA masses).
- Origin: Usually vestibular portion (inferior > superior).
- Pathogenesis:
- Sporadic (95%): Somatic mutation of NF2 gene (chromosome 22q12.2).
- NF2-associated (5%): Germline NF2 mutation.
- Leads to loss of merlin (schwannomin), a tumor suppressor.
⭐ Bilateral acoustic neuromas are pathognomonic for Neurofibromatosis Type 2 (NF2).
Clinical Presentation - Hearing's Slow Fade
- Progressive Unilateral Sensorineural Hearing Loss (SNHL):
- Most common (>90%) & earliest symptom.
- Insidious onset; patient may not notice initially.
- Difficulty understanding speech, esp. on phone or in noisy settings (cocktail party deafness).
- Speech discrimination disproportionately worse than pure tone thresholds (rollover phenomenon).
⭐ The most common and earliest symptom of acoustic neuroma is progressive, unilateral sensorineural hearing loss.
- Unilateral Tinnitus:
- High-pitched, continuous, or intermittent.
- Often precedes or accompanies hearing loss.
- Balance Issues (Disequilibrium):
- Vague unsteadiness, not typically true rotatory vertigo.
- Vertigo may occur if tumor compresses labyrinthine artery or causes hydrocephalus.
- Aural Fullness: Sensation of pressure in the ear.

Diagnostic Workup - Pinpointing the Problem
- Audiometry:
- Pure Tone Audiometry (PTA): Asymmetric high-frequency Sensorineural Hearing Loss (SNHL).
- Speech Discrimination Score (SDS): Disproportionately poor; rollover phenomenon.
- Tone Decay Test: Positive (often >30 dB).
- Auditory Brainstem Response (ABR):
- Screens for retrocochlear pathology.
- Finding: Prolonged Wave V latency or interpeak latency I-V (interaural difference >0.2 ms).
- Imaging (Definitive):
- MRI with Gadolinium: Gold Standard.
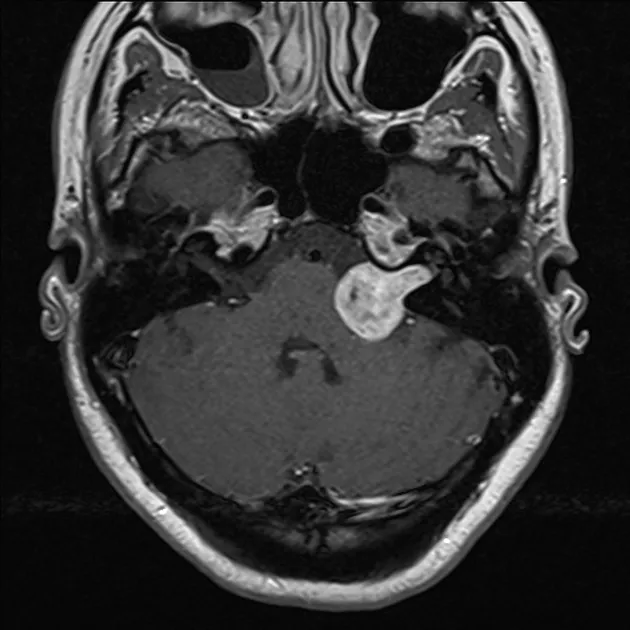
⭐ MRI with gadolinium contrast is the gold standard for diagnosing acoustic neuroma, often showing an "ice cream cone" appearance.
- CT Scan: Assesses bony erosion of Internal Auditory Canal (IAC); less sensitive for small tumors.
- MRI with Gadolinium: Gold Standard.
Management Strategies - Tumor Taming Tactics
- Observation (Wait & Scan):
- Small, asymptomatic tumors.
- Elderly/comorbid patients.
- Serial MRI monitoring.
- Microsurgery:
- Preferred for larger tumors (>3 cm), symptomatic, or younger patients.
- Aims: Tumor resection, facial nerve (FN) & hearing preservation.
- Approaches: Translabyrinthine, Retrosigmoid, Middle Fossa.
- Stereotactic Radiosurgery (SRS)/Radiotherapy (SRT):
- For smaller tumors (<3 cm), medically unfit for surgery, or recurrent tumors.
- Aims: Arrest tumor growth, preserve FN & hearing. (e.g., Gamma Knife)
⭐ For large acoustic neuromas (>3cm) causing brainstem compression or for younger patients, microsurgery is generally preferred over radiosurgery.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common CPA tumor; arises from Schwann cells of CN VIII (vestibular division).
- Bilateral acoustic neuromas are pathognomonic for Neurofibromatosis Type 2 (NF2).
- Earliest features: Progressive unilateral SNHL, tinnitus, and vestibular symptoms (disequilibrium).
- Speech discrimination is characteristically poorer than expected for the degree of hearing loss.
- Gold standard diagnosis: Gadolinium-enhanced MRI of the brain and IAC.
- CN V involvement (e.g., decreased corneal reflex) often precedes CN VII weakness.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


