Recon Goals & Basics - Setting the Stage
- Primary Aims:
- Restore function: speech, swallowing, airway patency.
- Achieve aesthetic form and symmetry.
- Ensure durable coverage; prevent complications (fistula, infection).
- Fundamental Principles:
- Replace "like with like" tissue.
- Prioritize robust vascular supply for flaps.
- Tension-free wound closure is critical.
- Minimize donor site morbidity.

⭐ The reconstructive ladder (from direct closure to free tissue transfer) dictates the simplest effective solution.
Recon Ladder - Climbing Choices
- Principle: Simplest effective method first.
- 1. Secondary Intention: Small, superficial defects.
- 2. Primary Closure: Minimal tension.
- 3. Skin Grafts:
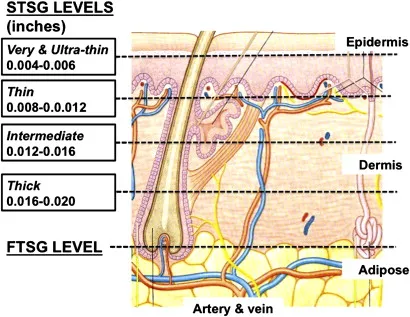
- STSG: Large areas.
- FTSG: Better cosmesis, smaller areas.
- 4. Local Flaps: Adjacent tissue (random/axial).
- 5. Regional Flaps: Pedicled (e.g., PMMC, Deltopectoral).
- 6. Free Flaps: Microvascular; for complex defects (e.g., RFFF, Fibula).
⭐ Free flaps offer superior vascularized tissue for complex 3D defects, vital for function and aesthetics. 📌 Mnemonic: "See Primary Grafts Locally, Regionally, Freely."
Skin Grafts - Patchwork Perfection
- Autologous transfer of epidermis & a variable amount of dermis, completely detached from donor site blood supply before transfer.
- Types:
- Split-Thickness Skin Graft (STSG):
- Epidermis + portion of dermis.
- Donor sites: Thigh, buttock, scalp. Harvested with dermatome (e.g., 0.010-0.018 inches).
- Pros: Better take, can cover large areas. Cons: ↑contraction, ↓cosmesis, fragile.
- Full-Thickness Skin Graft (FTSG):
- Epidermis + entire dermis.
- Donor sites: Postauricular, supraclavicular, preauricular, upper eyelid.
- Pros: ↓contraction, better cosmesis & durability. Cons: Limited size, needs well-vascularized bed.
- Split-Thickness Skin Graft (STSG):
- Graft take phases: 1. Plasmatic imbibition (0-48 hrs) 2. Inosculation (2-5 days) 3. Revascularization (>5 days).
- 📌 Causes of graft failure (HIS BED): Hematoma, Infection, Seroma, Bad recipient Bed (poor vascularity), Excessive tension, Dependent position (shear).
⭐ Meshing an STSG (e.g., ratios 1:1.5 up to 1:9) significantly increases its surface area coverage and allows for drainage of fluid from beneath the graft, improving take on contaminated or exudative wounds.
Flap Fundamentals - Vascular Victories
Flap: Tissue unit transferred with its intrinsic blood supply; maintains viability.
- Vascular Patterns:
- Random: Dermal-subdermal plexus.
- Axial: Specific arterio-venous system (e.g., Pectoralis Major Myocutaneous - PMMC).
- Classification by Movement:
- Local: Advancement, rotation, transposition.
- Regional: Pedicled from nearby territory.
- Distant (Free Flaps): Require microvascular anastomosis.
- Key Principle: Tension-free closure, adequate perfusion.
- 📌 Adequate Blood Supply Crucial (ABSC).
⭐ Most common free flap failure: Venous thrombosis (early post-op, <72 hrs).
 oka
oka
Workhorse Flaps - H&N Hit Parade
Key flaps for H&N reconstruction:
- PMMC (Pectoralis Major Myocutaneous):
- Pedicled; thoracoacromial a.
- Bulky, reliable. Oral cavity, pharynx.
- DP (Deltopectoral) Flap:
- Pedicled; internal mammary a. perforators.
- Thinner. Skin defects, fistula repair.
- LD (Latissimus Dorsi) Flap:
- Pedicled/free; thoracodorsal a.
- Large, versatile. Scalp, major defects.
- RFFF (Radial Forearm Free Flap):
- Free; radial a.
- Thin, pliable, sensate option. Oral lining.
- ALT (Anterolateral Thigh) Flap:
- Free; lateral circumflex femoral a. (descending br.)
- Versatile (skin/fascia/muscle). Large defects.
- FFF (Fibula Free Flap):
- Free; peroneal a.
- Osseocutaneous. Mandible reconstruction.
⭐ The Fibula Free Flap is preferred for mandible reconstruction due to its long bone stock (up to 25 cm), consistent anatomy, and ability to support dental implants.
 oka
oka
- The Reconstructive Ladder (or Elevator) guides choices from direct closure to free flaps.
- "Like with like" principle is key for optimal tissue replacement and function.
- Vascular pedicle integrity is paramount for flap survival.
- Key flaps: PMMC (workhorse), RFFF (oral lining), ALT (versatile), Fibula (mandible).
- Aim for three-layer closure: internal lining, structural support, and external cover.
- Prioritize functional outcomes (speech, deglutition) and aesthetics.
- Immediate reconstruction is generally preferred for most major H&N defects.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

