Anatomy - Neck's Hidden Hubs
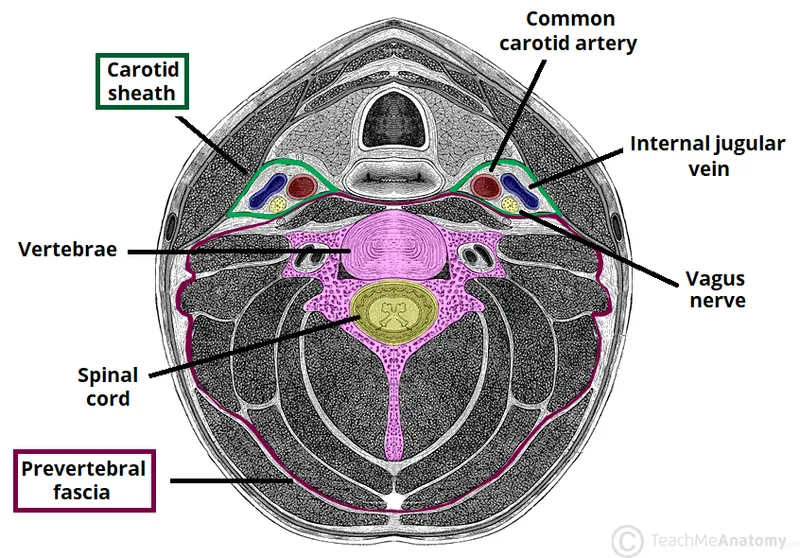
- Cervical Fascia:
- Superficial: Encloses platysma.
- Deep:
- Investing: Surrounds SCM, trapezius.
- Pretracheal: Forms visceral compartment.
- Prevertebral: Covers vertebral column/muscles.
- Key Deep Neck Spaces:
- Parapharyngeal (Lateral Pharyngeal): Lateral to pharynx.
- Retropharyngeal: Post. to pharynx; btw buccopharyngeal & alar fascia.
- Danger Space: Between alar & prevertebral fascia.
⭐ Extends skull base to diaphragm; "Highway for infection".
- Prevertebral: Ant. to vertebrae, deep to prevertebral fascia.
- Submandibular: Sublingual & submaxillary areas.
- Carotid Sheath: Common/internal carotid a., IJV, CN X.
- Pretracheal (Visceral): Surrounds trachea, esophagus, thyroid.
 oka
oka
Etiology & Bugs - Infection Invasion
- Etiology (Sources):
- Odontogenic (most common; mandibular molars)
- Tonsillopharyngeal (e.g., peritonsillar abscess)
- Salivary gland (sialadenitis)
- Trauma, IV drug use
- Common Pathogens (Often Polymicrobial):
- Aerobes: Streptococcus spp. (viridans, pyogenes), Staphylococcus aureus
- Anaerobes: Peptostreptococcus, Bacteroides, Prevotella, Fusobacterium
- Invasion: Direct spread, lymphatic.
⭐ Fusobacterium necrophorum is classically associated with Lemierre's syndrome (postanginal sepsis, IJV thrombophlebitis).
Clinical Clues & Dx - Spotting the Sepsis
- General: Fever, neck pain/swelling, dysphagia, odynophagia, trismus.
- Airway: Stridor, dyspnea - ⚠️ EMERGENCY!
- Specific Signs: Vary by space (e.g., Ludwig's: woody submandibular swelling).
- Investigation:
- CT with contrast: GOLD STANDARD. Defines extent, abscess.
- Labs: ↑WBC, ↑CRP.
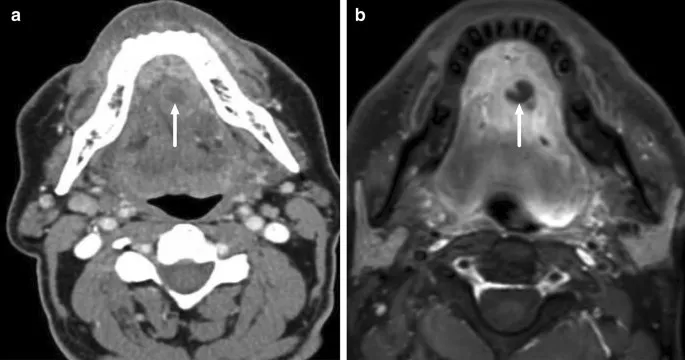
⭐ Ludwig's angina (bilateral submandibular, sublingual, submental space infection) can cause rapid airway obstruction.
Key Infections - Danger Deep Dive
- Ludwig's Angina:
- Bilateral cellulitis: submandibular, sublingual, submental spaces.
- Source: Odontogenic (mandibular molars).
- Symptoms: "Woody" floor of mouth, tongue elevation, drooling, airway risk.
- Retropharyngeal Abscess (RPA):
- Children (<5 yrs): Often after URI; midline swelling, fever, torticollis, dysphagia.
- Adults: Trauma, foreign body; can be lateral.
- Risk: Danger space spread → mediastinitis.
- Parapharyngeal Abscess (PPA):
- Source: Tonsillar, pharyngeal, dental.
- Symptoms: Trismus, medial pharyngeal wall bulge, fever, neck pain/swelling.
- Compartments: Prestyloid (trismus prominent) vs. Poststyloid (cranial nerve palsies, vascular risk).
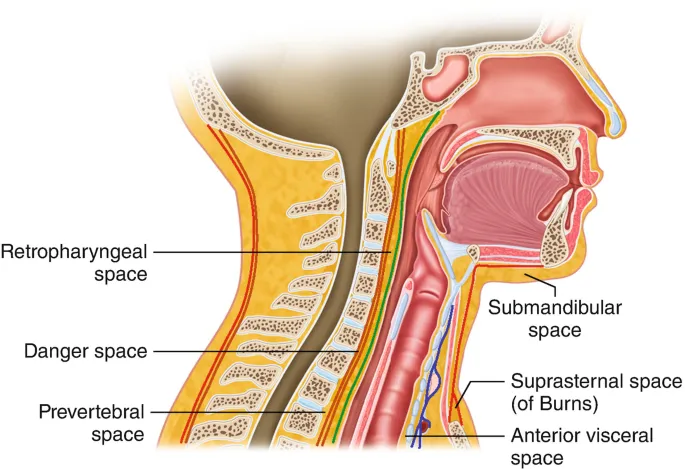
⭐ In children, retropharyngeal abscesses are typically midline due to infection of retropharyngeal lymph nodes (nodes of Rouviere), which atrophy by age 4-5 years old.
Management & Mayhem - Treatment & Threats
-
Airway First! Secure immediately if compromised (stridor, dyspnea). Options: intubation, tracheostomy.
-
IV Antibiotics: Empiric broad-spectrum (e.g., Ampicillin-Sulbactam, Clindamycin +/- Metronidazole). Tailor to culture results.
-
Surgical Drainage Indications:
- Airway compromise despite medical Rx
- Definitive collection > 2-3 cm on CT scan
- No clinical improvement in 24-48 hrs of IV antibiotics
- Presence of complications (e.g., mediastinitis)
- Specific spaces (e.g., Ludwig's angina often needs early drainage)
-
Dreaded Complications (Mayhem):
- Airway Obstruction (esp. Ludwig's Angina)
- Descending Necrotizing Mediastinitis (DNM) - high mortality
- Sepsis / Septic Shock
- Lemierre’s Syndrome (IJV thrombophlebitis, often F. necrophorum)
- Carotid artery rupture, cranial nerve (CN) palsies
⭐ Ludwig's angina involves bilateral submandibular, sublingual, and submental spaces, rapidly progressing to airway obstruction if not managed promptly; it's a surgical emergency if airway is threatened or significant cellulitis/collection exists despite antibiotics.
- Ludwig's angina: bilateral infection of submandibular, sublingual, submental spaces; odontogenic origin; high airway risk.
- Parapharyngeal space infection: presents with trismus, medial bulge of lateral pharyngeal wall.
- Retropharyngeal abscess: common in children <5 yrs; risk of mediastinitis, airway obstruction.
- Danger space (Space 4): infection rapidly spreads to posterior mediastinum.
- CT scan with contrast is key for diagnosis and extent.
- Core management: Secure airway, IV antibiotics, prompt surgical drainage.
- Predominant organisms: Aerobic Streptococci and anaerobes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

