Definition & Etiopathogenesis - Dizzying Dilemma
- Definition: Acute, severe, prolonged vertigo from unilateral vestibular hypofunction. Crucially, no auditory or neurological symptoms.
- Etiology:
- Predominantly viral (Herpes Simplex Virus type 1 (HSV-1) reactivation in vestibular ganglion is a leading theory).
- Post-viral inflammation.
- Less common: Ischemic (e.g., anterior vestibular artery).
- Pathogenesis: Inflammation of vestibular nerve (CN VIII), often selectively affecting the superior division.
⭐ Vestibular neuritis is distinguished from labyrinthitis by the absence of hearing loss or tinnitus.
Clinical Presentation - The World Spins
- Sudden, severe, persistent vertigo (rotational); lasts days to weeks.
- Associated with:
- Intense nausea & vomiting.
- Imbalance & gait ataxia (veers towards affected side).
- Symptoms worsen with head movements.
- Crucial negatives:
- NO hearing loss.
- NO tinnitus.
- NO focal neurological signs.
- Nystagmus: Spontaneous, unidirectional (horizontal/horizontal-torsional); suppressed by visual fixation. Follows Alexander's Law.
- Positive Head Impulse Test (HIT) towards affected side.
- Often preceded by viral illness (URI) in ~50% cases.
⭐ Absence of auditory symptoms (hearing loss, tinnitus) is key to differentiate vestibular neuritis from labyrinthitis.
Diagnosis & Investigations - Pinpointing Vertigo
- Clinical: Acute, persistent vertigo, N/V, gait instability. NO hearing loss/tinnitus.
- Nystagmus: Spontaneous, unidirectional, horizontal-torsional; fast phase beats away from affected side; suppressed by fixation.
- Head Impulse Test (HIT): Positive - corrective saccade towards affected side.
- Test of Skew: Negative.
- 📌 HINTS exam (Head Impulse, Nystagmus, Test of Skew): Differentiates peripheral (VN) vs. central (stroke).
- Audiometry: Normal.
- MRI: If atypical or HINTS worrisome for central lesion.
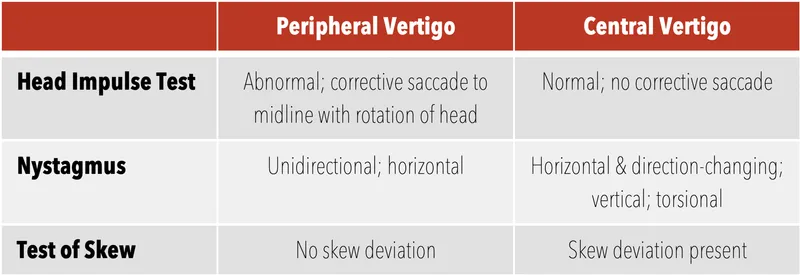
⭐ The HINTS exam is highly sensitive for stroke when a patient presents with acute vestibular syndrome and at least one stroke risk factor; a reassuring (peripheral) HINTS makes stroke very unlikely.
Differential Diagnosis - Ruling Rivals Out
- Labyrinthitis:
- Sudden vertigo WITH auditory symptoms (hearing loss, tinnitus). Full labyrinth inflammation.
⭐ Unlike vestibular neuritis (nerve only), labyrinthitis involves cochlear symptoms due to labyrinthine inflammation.
- Meniere's Disease:
- Episodic vertigo (min-hrs), fluctuating low-frequency SNHL, tinnitus, aural fullness.
- BPPV (Benign Paroxysmal Positional Vertigo):
- Brief, positional vertigo (sec-min); head movement trigger. Dix-Hallpike positive.
- Central Causes (Stroke/TIA - posterior circulation):
- Sudden, severe, persistent vertigo; neurological signs (ataxia, dysarthria). HINTS exam vital.
- Vestibular Migraine:
- Episodic vertigo with migraine history/symptoms (headache, aura).
Management & Prognosis - Steadying Steps
- Acute Phase:
- Symptomatic relief: Antiemetics (ondansetron), vestibular suppressants (meclizine, diazepam; use <3 days to avoid delaying compensation).
- Corticosteroids: E.g., Prednisolone 1mg/kg/day (max 60mg) tapered over 10-14 days, if within 72 hours of onset; may hasten recovery.
- Rehabilitation Phase:
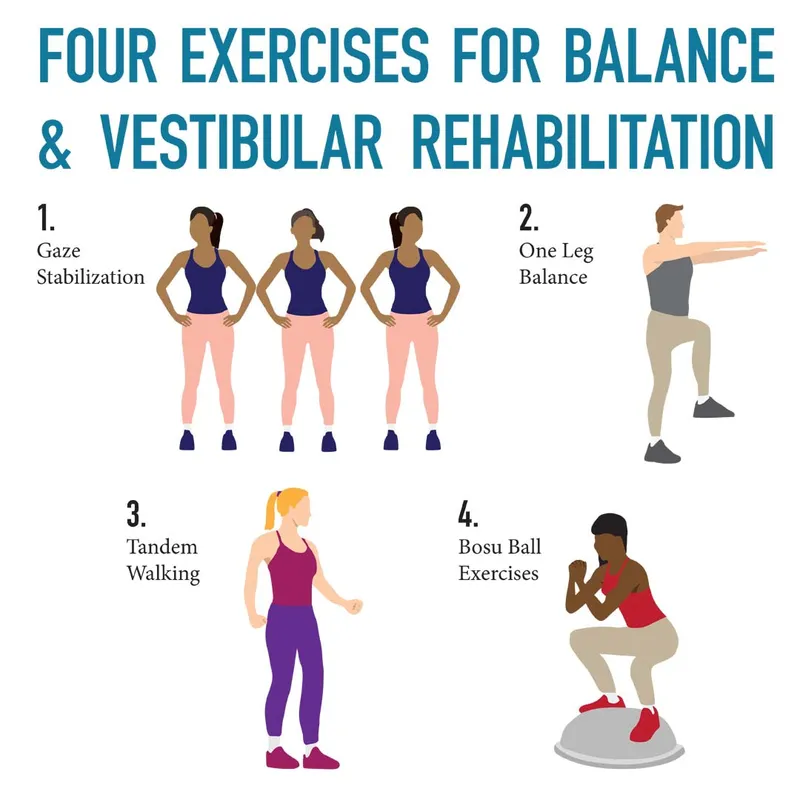
- Vestibular Rehabilitation Therapy (VRT): Crucial. Start as soon as tolerated.
- Gaze stabilization, habituation, balance training (e.g., Cawthorne-Cooksey exercises).
- Vestibular Rehabilitation Therapy (VRT): Crucial. Start as soon as tolerated.
- Prognosis:
- Acute symptoms resolve in days; full recovery in weeks to months for most.
- ~30% may have residual dizziness. Recurrence: ~2-10%.
- Potential for post-neuritis BPPV.
⭐ Early initiation of VRT is paramount for optimal functional recovery and reducing chronic symptoms.
High-Yield Points - ⚡ Biggest Takeaways
- Viral infection (often URI) precedes vestibular nerve inflammation.
- Sudden, severe, persistent vertigo, nausea, vomiting; lasts days.
- No auditory symptoms (hearing preserved) - key differentiator from labyrinthitis.
- Unidirectional horizontal nystagmus (fast phase away from affected side).
- Positive Head Impulse Test (HIT) towards affected side is diagnostic.
- Treatment: Corticosteroids (early), vestibular suppressants, antiemetics, vestibular rehabilitation.
- Prognosis generally good; most recover fully with rehabilitation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

