Scabies: Overview - Itchy Tiny Terrors
- Definition: Intensely pruritic skin infestation by Sarcoptes scabiei var. hominis (human itch mite).
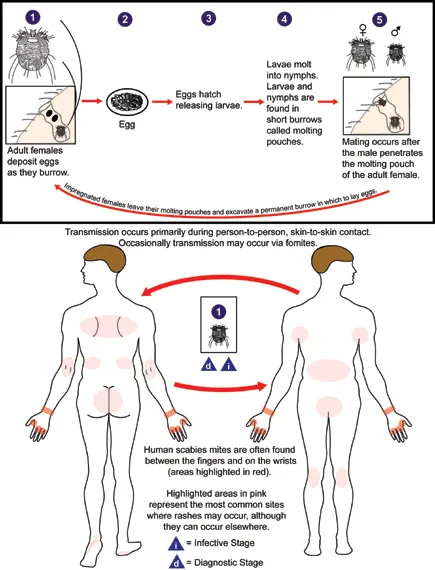
- Lifecycle: Female mite burrows in epidermis, lays eggs. Larvae hatch (3-4 days), mature to adults (10-14 days).
- Transmission: Primarily prolonged skin-to-skin contact. Fomites: less common (classic), significant (crusted).
- Incubation Period:
- Non-sensitized (1st infection): 2-6 weeks.
- Sensitized (re-infestation): 1-4 days.
⭐ Crusted scabies is highly contagious due to a massive mite burden (up to millions of mites), often in immunocompromised individuals anergic to the mite antigens, leading to minimal itching despite high parasite load.
Scabies: Clinical Features - Burrowing Blues
- Cardinal Symptom: Intense pruritus, classically worse at night.
⭐ Intense nocturnal pruritus ("wake-up sign") is a hallmark of scabies, often disrupting sleep.
- Characteristic Lesions:
- Burrows (pathognomonic): Greyish/skin-colored, serpiginous lines.
- Papules, vesicles, pustules, nodules, excoriations.
- Distribution:
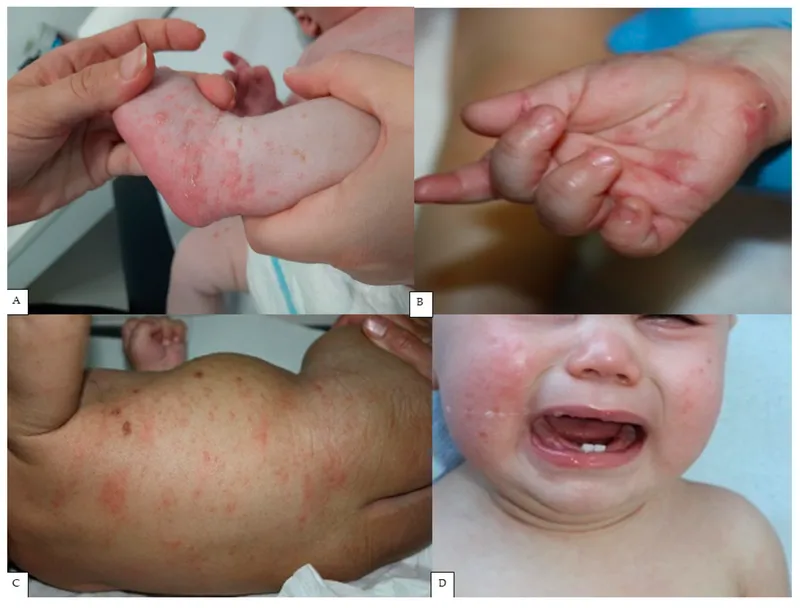
- Common sites: Finger webs, wrists (flexor), axillae, elbows, beltline, buttocks, genitalia (males), areolae (females).
- Head/neck/palms/soles usually spared in adults; may be involved in infants, elderly, or immunocompromised.
- 📌 ITCHING SITES: Interdigital, Trunk (beltline), Creases (axillae, elbow), Hands/wrists, Insteps, Navel, Genitalia, Scapula/Shoulder.
- Special Types:
- Crusted (Norwegian) Scabies: Hyperkeratotic plaques, ↑↑ mite load (millions), highly contagious. Often in immunocompromised/elderly; pruritus may be minimal initially.
- Nodular Scabies: Persistent, itchy, reddish-brown nodules (e.g., groin, axillae, buttocks); a hypersensitivity reaction.
- Bullous Scabies: Resembles bullous pemphigoid; blisters present.
- Scabies Incognito: Altered appearance due to topical steroid use, masking typical signs.
| Feature | Classic Scabies | Crusted (Norwegian) Scabies |
|---|---|---|
| Mite Load | Low (typically <15 mites) | Very High (millions) |
| Pruritus | Intense | Variable, often mild or absent |
| Appearance | Papules, vesicles, burrows | Widespread, crusted, scaly plaques |
| Contagiousness | High | Extremely High |
| Host Status | Usually Immunocompetent | Often Immunocompromised, elderly |
Scabies: Diagnosis - Mite Spotting Mission
- Clinical dx: History (pruritus, contacts), lesion pattern.
- Skin scraping: #15 blade, mineral oil; find mites, eggs, scybala. Variable sensitivity.
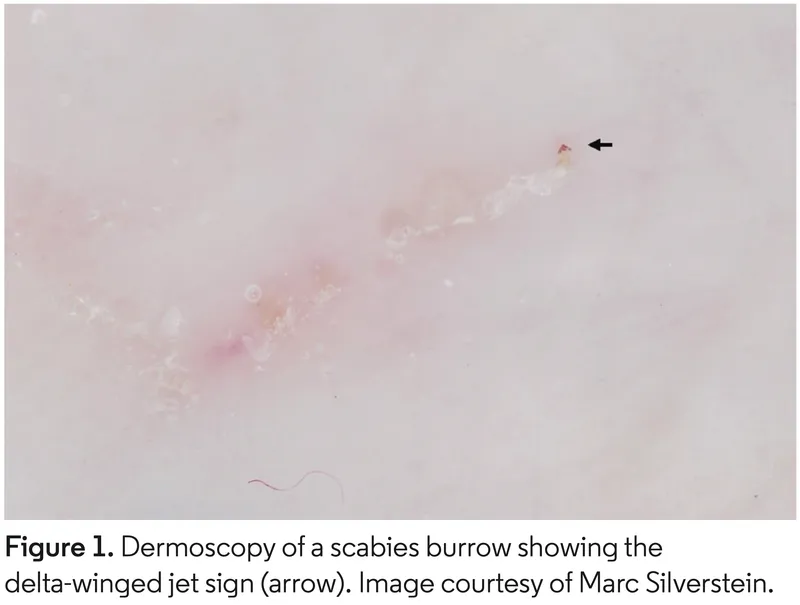
- Dermoscopy: "Delta wing" sign (mite's pigmented anterior), "jetliner with contrail" (mite & burrow).
- Adhesive tape test: Alternative, esp. children.
- Biopsy (rare): Mites in stratum corneum, eosinophils.
⭐ Negative scraping doesn't rule out scabies; mite count can be low (avg 10-15).
- DDx: Eczema, insect bites, papular urticaria, dermatitis herpetiformis.
Scabies: Treatment - Eviction Notice
- Goals: Eradicate mites, manage pruritus, prevent transmission.
- Topical (1st line): Permethrin 5% cream (DOC). Neck down, 8-14 hrs, repeat 1 wk. 📌 Permethrin is Perfect.
- Oral: Ivermectin (200 mcg/kg single dose, repeat 1-2 wks). For crusted, outbreaks, non-compliant. 📌 Ivermectin is Internal.
- Crusted Scabies: Combo topical + oral Ivermectin (multiple doses), keratolytics.
- Special Pop: Infants >2m, pregnant/lactating: Permethrin 5%.
- Adjuncts:
- Antihistamines (pruritus), mild topical corticosteroids (post-scabetic dermatitis).
- Treat contacts (simultaneously, even asymptomatic).
- Environment: Wash items >50°C or seal ≥72 hrs.
⭐ Post-scabetic pruritus (2-4 wks) common after mite eradication due to hypersensitivity; not treatment failure.
Scabies: Complications & Prevention - Staying Clear & Calm
- Complications:
- Bacterial superinfection (impetigo, cellulitis; risk PSGN, ARF)
- Post-scabetic pruritus, nodular scabies
- Scabies incognito (steroid misuse)
- Prevention:
- Prompt treatment: index case & all contacts
- Hot wash/dry linens, clothing
- Patient education
⭐ Secondary bacterial infections are common, serious, and can lead to systemic illness.
High‑Yield Points - ⚡ Biggest Takeaways
- Caused by mite Sarcoptes scabiei var. hominis.
- Intense nocturnal pruritus is the hallmark symptom.
- Burrows are pathognomonic; common in interdigital webs, wrists, axillae, genitals.
- Diagnosis: Microscopy of skin scrapings for mites, eggs, or scybala.
- Treatment: Permethrin 5% cream (topical); oral Ivermectin for severe/crusted scabies.
- Crusted (Norwegian) scabies: Seen in immunocompromised patients; highly contagious with numerous mites.
- Treat all household members and close contacts simultaneously to prevent re-infestation_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

