Intro & Epidemiology - Patchy Hair Havoc
- Autoimmune, T-cell mediated, non-scarring hair loss targeting anagen hair follicles.
- Presents as well-demarcated, smooth patches of alopecia, often round or oval.
- Types:
- Alopecia Areata (patchy): Most common; one or more coin-sized patches.
- Alopecia Totalis (AT): Complete loss of scalp hair.
- Alopecia Universalis (AU): Complete loss of all body and scalp hair.
- Epidemiology:
- Lifetime risk: ~1.7-2%.
- Peak incidence: Ages 20-40 years; can occur at any age.
- Associations: Autoimmune diseases (thyroiditis, vitiligo), atopy, Down syndrome.
⭐ "Exclamation mark hairs" (short, <3-4 mm, broken hairs, tapered proximally) are pathognomonic, found at active lesion peripheries.
Pathophysiology - Immune System Mischief
- Autoimmune disease: T-lymphocyte mediated attack targeting anagen (growing) hair follicles.
- Key immune cells: Cytotoxic CD8+ T cells and Natural Killer Group 2D (NKG2D+) expressing cells.
- Pro-inflammatory cytokines: Interferon-gamma (IFN-γ) and Interleukin-15 (IL-15) are pivotal.
- Mechanism: Collapse of the hair follicle's immune privilege, leading to recognition of self-antigens.
- Genetic susceptibility: Strong associations with specific Human Leukocyte Antigen (HLA) alleles (e.g., HLA-DRB1, HLA-DQB1).
- Potential triggers: Viral infections, severe emotional or physiological stress; exact role varies.

⭐ Histologically, a perifollicular lymphocytic infiltrate around the anagen hair bulb, often described as a "swarm of bees," is characteristic (though not pathognomonic).
Clinical Presentation - Spotting the Spots

- Well-demarcated, round or oval patches of non-scarring hair loss.
- Affected skin is smooth, skin-colored, or slightly erythematous; no scaling.
Diagnosis & Differentials - Sleuthing the Scalp
- Clinical Diagnosis:
- Well-demarcated, smooth, round/oval patches of non-scarring hair loss.
- Exclamation mark hairs (short, broken hairs, narrower at base) at periphery - pathognomonic.
- Nail changes: pitting (most common), Beau's lines, trachyonychia.
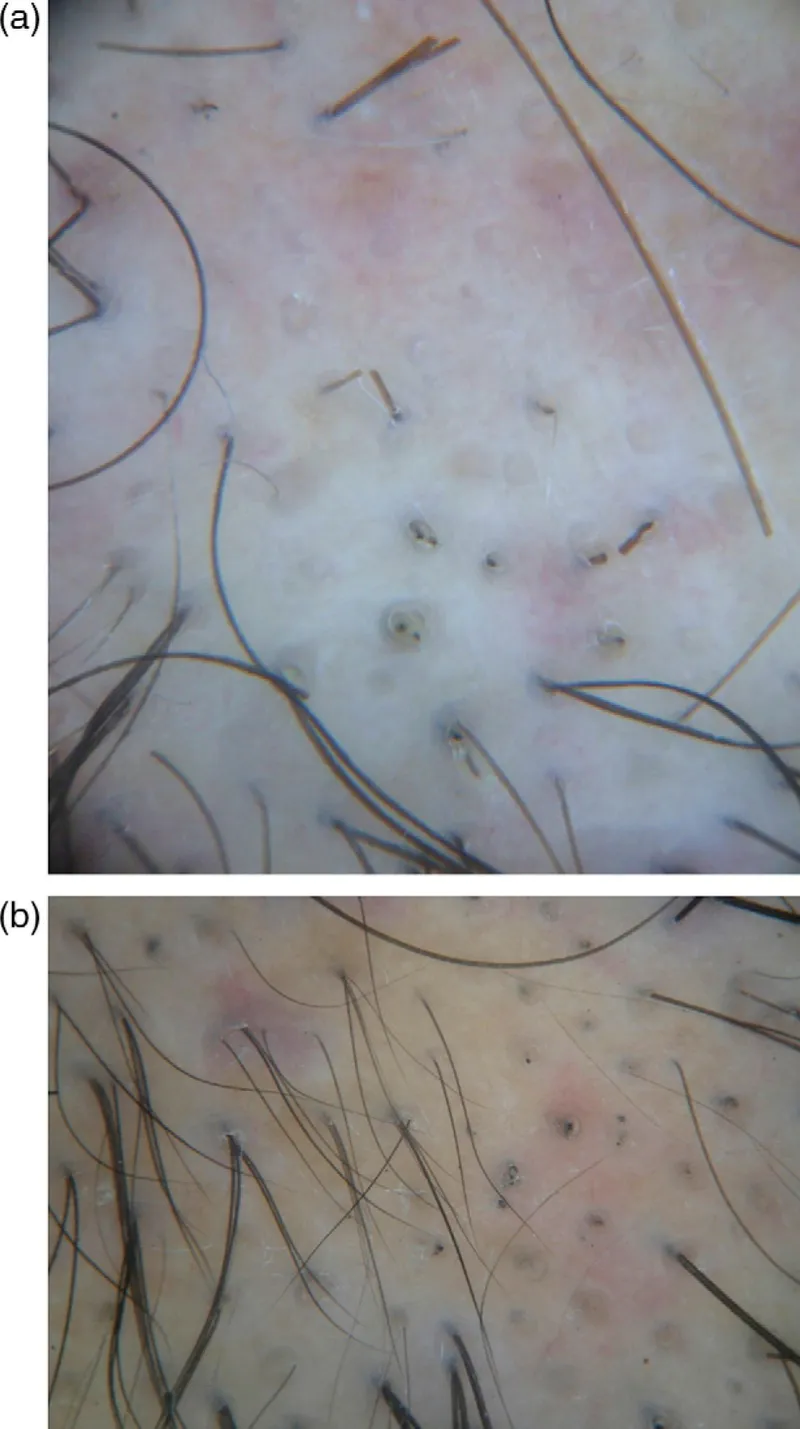
- Dermoscopy (Trichoscopy):
- Yellow dots (sebaceous gland openings).
- Black dots (cadaverized hairs).
- Broken hairs, exclamation mark hairs.
- Biopsy (Rarely needed):
- Peribulbar lymphocytic infiltrate ("swarm of bees").
- Differential Diagnosis:
- Tinea capitis (scaling, broken hairs, +KOH).
- Trichotillomania (irregular patches, varying hair lengths, bizarre shapes).
- Androgenetic alopecia (patterned loss).
- Telogen effluvium (diffuse shedding).
- Secondary syphilis ("moth-eaten" alopecia).
⭐ Alopecia Areata is an autoimmune condition often associated with other autoimmune diseases like thyroid disorders (Hashimoto's thyroiditis) and vitiligo.
Management Strategies - Taming the Tresses
- Goal: Arrest progression, induce regrowth. Choice based on age, extent, activity, duration.
- Limited Patchy AA (<50% scalp):
- Intralesional corticosteroids (triamcinolone acetonide 2.5-10 mg/mL) q 4-6 wks. First-line.
- Potent topical corticosteroids.
- Topical minoxidil 5% solution/foam.
- Topical immunotherapy (DPCP, SADBE) for refractory cases.
- Extensive AA (>50% scalp) / Rapid / Alopecia Totalis/Universalis (AT/AU):
- Systemic corticosteroids (oral prednisone 0.5-1 mg/kg/day).
- Systemic immunosuppressants (methotrexate, azathioprine).
- JAK inhibitors (e.g., tofacitinib, baricitinib) - emerging.
- Counselling & camouflage (wigs).
⭐ Ophiasis pattern, nail involvement, early onset, and atopy are poor prognostic indicators.
High‑Yield Points - ⚡ Biggest Takeaways
- Alopecia Areata: An autoimmune T-cell attack on hair follicles, causing non-scarring hair loss.
- Key features: Patchy alopecia, pathognomonic exclamation mark hairs at patch edges.
- Associated with other autoimmune diseases like thyroiditis, vitiligo, and Down syndrome.
- Nail changes are common: Pitting (most frequent), trachyonychia (sandpaper nails), Beau's lines.
- Treatment: Intralesional corticosteroids for limited patches; topical immunotherapy (e.g., DPCP) for extensive disease.
- May progress to alopecia totalis (scalp) or universalis (body); spontaneous remission can occur.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

