Rosacea - Ruddy Beginnings
- Definition: Chronic inflammatory disorder primarily affecting central facial skin (cheeks, nose, chin, forehead).
- Age of Onset: Typically 30-50 years.
- Gender Predilection: Females > Males; however, males often develop more severe manifestations like rhinophyma.
- Key Risk Factors:
- Fair skin types (e.g., Celtic ancestry)
- Positive family history
- Chronic UV radiation exposure
- Demodex folliculorum mite infestation
- H. pylori infection (role remains debated)

⭐ Rhinophyma, characterized by a thickened, bulbous, and erythematous nose, is a subtype of rosacea predominantly seen in older men.
Rosacea - The Why Behind
- Neurovascular Dysregulation:
- TRP channels (TRPV1, TRPA1) on nerves/endothelium.
- Causes flushing, persistent erythema, telangiectasias.
- Innate Immune Activation:
- ↑ Cathelicidin LL-37 (abnormally processed).
- TLR2 activation by various triggers.
- Microbial Factors:
- Demodex folliculorum mites (↑ density).
- Bacillus oleronius (Demodex-associated).
- Mast Cell Activation:
- Releases key inflammatory mediators (histamine, proteases).
- Chronic Inflammation:
- Common pathway driving persistent skin changes.
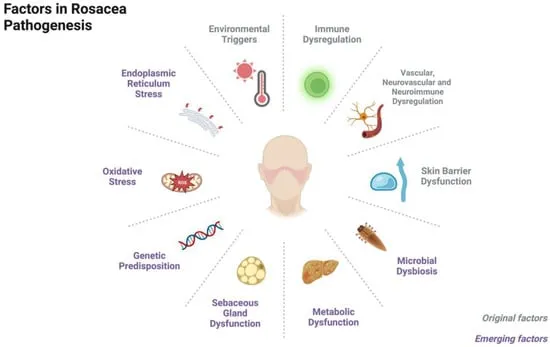
- Common pathway driving persistent skin changes.
⭐ Aberrant cathelicidin LL-37 (↑ levels, altered peptides) is a pivotal driver of inflammation and vascular effects in rosacea.
Rosacea - Faces of Redness
Rosacea: A chronic inflammatory disorder affecting the centrofacial skin, characterized by remissions and exacerbations. Common triggers include heat, sunlight, spicy foods, and alcohol.
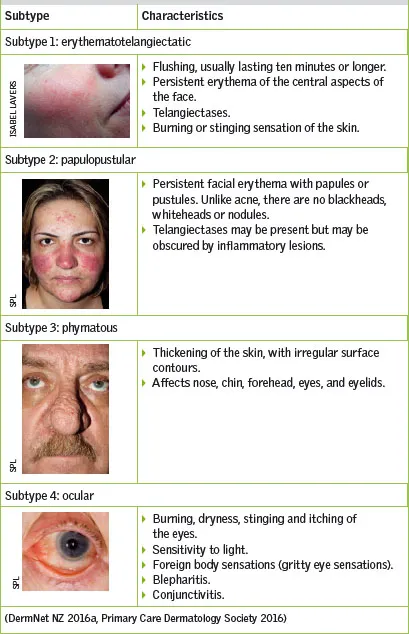
Four Main Subtypes:
| Subtype | Key Features |
|---|---|
| Erythematotelangiectatic (ETR) | Flushing, persistent central facial erythema, and telangiectasias are hallmark features. |
| Papulopustular (PPR) | Presents with transient papules and pustules on a background of central facial erythema. |
| Phymatous | Leads to skin thickening and irregular surface nodularities, most notably rhinophyma (nose). |
| Ocular | Manifests with symptoms like foreign body sensation, burning, stinging, dryness, blepharitis, and conjunctivitis. |
- Granulomatous rosacea: Characterized by monomorphic yellow-brown or reddish papules/nodules, often periorificial.
⭐ Ocular involvement occurs in up to 50-75% of rosacea patients and can sometimes precede skin changes.
Rosacea - Nailing the Diagnosis
Diagnosis is clinical, based on characteristic findings.
- Key Diagnostic Features (≥1 needed):
- Persistent centrofacial erythema
- Phymatous changes (e.g., rhinophyma)
- Major Features (≥2 needed if key features absent):
- Papules/pustules
- Flushing
- Telangiectasias
- Ocular manifestations
- Secondary Features: Burning/stinging, edema, dry appearance.
- Differential Diagnosis:
- Acne vulgaris (comedones present)
- Seborrheic dermatitis (greasy scales)
- Lupus (malar rash, spares nasolabial folds, ANA+)
- Perioral dermatitis
⭐ Rosacea is distinguished from acne vulgaris by the absence of comedones.
Rosacea - Calming the Crimson
- General Measures: Avoid triggers (sun, heat, alcohol, spicy food); gentle skincare; broad-spectrum sunscreen (SPF ≥30).
- Topical: Metronidazole, Azelaic acid, Ivermectin, Brimonidine (erythema), Sulfacetamide-sulfur.
- Systemic:
- Oral antibiotics: Doxycycline (40mg MR or 100mg), Minocycline.
- Severe/refractory: Oral Isotretinoin.
- Physical: Laser/IPL (telangiectasias, persistent erythema); Surgical debulking (rhinophyma).
- Ocular: Lid hygiene, artificial tears, topical/oral antibiotics.
⭐ Doxycycline at a 40mg modified-release dose provides anti-inflammatory action for rosacea, below antimicrobial thresholds.
High‑Yield Points - ⚡ Biggest Takeaways
- Characterized by chronic facial erythema, telangiectasias, papules/pustules; crucially, no comedones.
- Main subtypes: Erythematotelangiectatic (ETR), Papulopustular (PPR), Phymatous (e.g., rhinophyma), and Ocular.
- Rhinophyma, a phymatous change of the nose, is more common in men.
- Ocular rosacea presents with conjunctivitis, blepharitis, potentially keratitis.
- Common triggers: sunlight, heat, alcohol, spicy food, stress.
- First-line treatments: Topical metronidazole, azelaic acid, ivermectin; oral tetracyclines (e.g., doxycycline).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

