HAIs Intro - Hospital's Sneaky Germs
- Definition: Infections acquired during hospital stay; not present/incubating at admission. Also called Nosocomial Infections.
- Onset Criteria:
- Develops ≥ 48 hours after hospital admission.
- Within 3 days of discharge.
- Within 30 days after an operation (or up to 1 year if implant present).
- Sources:
- Endogenous: Patient's own flora (e.g., skin, gut).
- Exogenous: External sources (e.g., healthcare staff, contaminated equipment, environment).
- Major Types & Common Pathogens:
- CAUTI (Catheter-Associated UTI): E. coli, Klebsiella, Pseudomonas, Enterococcus, Candida.
- SSI (Surgical Site Infection): S. aureus, Coagulase-negative Staphylococci, Enterococcus.
- VAP (Ventilator-Associated Pneumonia): Pseudomonas, Acinetobacter, S. aureus (MRSA), Enterobacteriaceae.
- CLABSI (Central Line-Associated Bloodstream Infection): Coagulase-negative Staphylococci, S. aureus, Candida.
- Impact: ↑ Morbidity, mortality, hospital stay, & healthcare costs.
⭐ The most common healthcare-associated infection worldwide is Catheter-Associated Urinary Tract Infection (CAUTI).

📌 Mnemonic (Common HAIs - "SCUM Vets"): SSI, CAUTI, Upper respiratory (like VAP), Meningitis (rare), Vascular access (CLABSI), ets (others like GIT infections).
CAUTI & CLABSI - Pipe Problems
Catheter-Associated Urinary Tract Infection (CAUTI)
- UTI with indwelling urinary catheter (IUC) >2 days.
- Pathogens: E. coli (most common), Klebsiella, Pseudomonas, Enterococcus, Candida.
- Prevention (📌 HANDS):
- Hand hygiene.
- Aseptic insertion, proper maintenance.
- Necessity review daily.
- Drainage bag below bladder, off floor.
- Secure catheter.
- Diagnosis: Urine culture ≥$10^3$ CFU/mL.
Central Line-Associated Bloodstream Infection (CLABSI)
- Lab-confirmed BSI with central line >2 days.
- Pathogens: CoNS, S. aureus, Enterococcus, Gram-negatives, Candida.
- Prevention (📌 CLABSI BUNDLE):
- Hand hygiene.
- Maximal barrier precautions (insertion).
- Chlorhexidine skin antisepsis.
- Optimal site selection (subclavian > jugular > femoral).
- Daily review of line necessity & prompt removal.
- Hub disinfection ("Scrub the Hub").
⭐ Differential Time to Positivity (DTP): Blood culture from CVC positive ≥2 hours before peripheral culture strongly suggests CLABSI.

VAP & SSI - Breath & Breach Bugs
Ventilator-Associated Pneumonia (VAP):
- Pneumonia developing >48 hours after endotracheal intubation.
- Early-onset (<5 days): S. pneumoniae, H. influenzae, MSSA.
- Late-onset (>5 days): Pseudomonas aeruginosa, Acinetobacter spp., MRSA.
- Prevention: Head elevation (30-45°), oral chlorhexidine, daily sedation interruption, early weaning, subglottic suctioning.
Surgical Site Infection (SSI):
- Infection at/near surgical incision within 30 days (or 1 year if implant present).
- Types: Superficial incisional, Deep incisional, Organ/space.
- Common bugs: Staphylococcus aureus (most common), CoNS, Enterococcus spp., E. coli.
- Prevention: Prophylactic antibiotics (~60 min pre-incision), clippers (not razor), aseptic technique, post-op wound care.
⭐ Most SSIs are caused by the patient's endogenous flora, particularly skin flora like Staphylococcus aureus.
AMR & Surveillance - Resistance Watch
- Antimicrobial Resistance (AMR): Major threat in HAIs, increasing morbidity, mortality, and costs.
- Driven by antibiotic overuse and misuse.
- Key pathogens (📌 ESKAPE): E. faecium (VRE), MRSA, CRE (K. pneumo), A. baumannii, P. aeruginosa, Enterobacter.
- Surveillance Systems: Essential for tracking AMR patterns and informing interventions.
- National: NCDC (National Programme on AMR Containment), ICMR AMR Network.
- Global: WHO GLASS, WHONET software.
- Antimicrobial Stewardship (AMS): Programs to promote appropriate antibiotic prescribing.
- Aims: Improve patient outcomes, reduce toxicity, and ↓selective pressure for AMR.
- Core strategies: Prospective audit & feedback, formulary restriction, education.
⭐ Carbapenem-Resistant Enterobacteriaceae (CRE) are a critical priority in HAIs due to extensive drug resistance and associated high mortality rates.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common HAI: Catheter-Associated UTI (CAUTI).
- Common ICU pathogens: S. aureus (MRSA), P. aeruginosa.
- Ventilator-Associated Pneumonia (VAP): Develops >48 hrs post-intubation. Prevention: head elevation.
- CLABSI prevention: Strict aseptic technique for central line insertion and care.
- Surgical Site Infection (SSI): Within 30 days (or 1 year with implant). Prophylaxis: antibiotics ~60 mins pre-op.
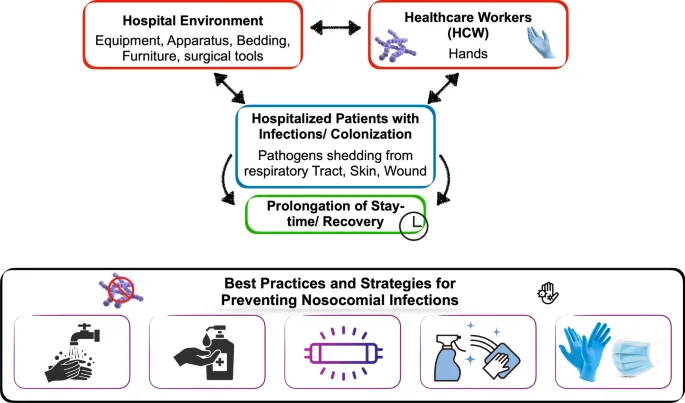
- Hand hygiene: Most crucial HAI prevention; alcohol-based rubs preferred.
- Standard precautions: Apply to all patients to prevent transmission.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

