Fructose Path & Benign Spill - Sweet & Simple
- Normal Fructose Path:
- Fructose + ATP $\xrightarrow{\text{Fructokinase (KHK)}}$ Fructose-1-Phosphate (F1P) + ADP
- F1P $\xrightarrow{\text{Aldolase B}}$ Dihydroxyacetone Phosphate (DHAP) + Glyceraldehyde
- Essential Fructosuria (Benign Fructosuria):
- Deficiency: Fructokinase (hepatic KHK).
- Inheritance: Autosomal Recessive.
- Pathophysiology: Fructose accumulates in blood & urine (fructosuria).
- Clinical: Asymptomatic, benign condition. Fructose spills into urine.
- Diagnosis: Urine positive for reducing sugars (e.g., Benedict's test); negative for glucose (glucose oxidase test).
- 📌 Mnemonic: Kind Herbert's Kids (KHK) spill sugar, but are fine!
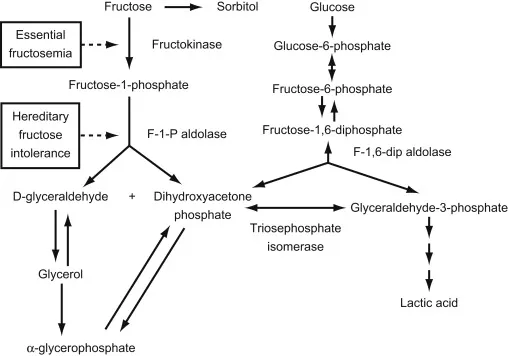
⭐ Essential fructosuria is a benign, asymptomatic condition often detected incidentally by a positive urine test for reducing substances, while the glucose-specific urine test is negative.
HFI Havoc - Fructose's Fury
- Defect: Autosomal recessive, Aldolase B deficiency.
- Accumulation: Fructose-1-Phosphate (F-1-P) in liver, kidney, intestine.
- Pathophysiology:
- F-1-P traps $PO_4^{3-}$ $\rightarrow$ ↓ ATP, ↓ $P_i$.
- Inhibits gluconeogenesis & glycogenolysis $\rightarrow$ severe hypoglycemia.
- Onset: Symptoms post fructose/sucrose/sorbitol ingestion (weaning, juices).
- Clinical Features:
- Severe hypoglycemia, vomiting, jaundice, hepatomegaly.
- Lactic acidosis, hyperuricemia.
- Chronic: Failure to thrive, liver/kidney failure, sweet aversion.
- Diagnosis:
- Clinical; urine reducing substances (+ve Clinitest, -ve GOD).
- Genetic test (ALDOB) or liver biopsy (enzyme assay).
- ⚠️ Fructose tolerance test: DANGEROUS.
- Management: Lifelong dietary elimination of fructose, sucrose, sorbitol.
- 📌 Mnemonic: HFI = Hypoglycemia, F-1-P ↑, Inhibition of pathways.
⭐ Fructose-1-phosphate accumulation is key in HFI: traps phosphate, depletes ATP, inhibits gluconeogenesis & glycogenolysis.

Galactose Path & Lens Alert - Milky Way Minors
- Galactose (from milk) metabolism: GALK → GALT → GALE.
- Galactokinase (GALK) Deficiency:
- $GALK1$ defect. ↑ Galactose leads to ↑ Galactitol.
- Key: Infantile cataracts, galactosuria.
- Spares liver/brain. Rx: Galactose-free diet.
- UDP-Galactose-4-Epimerase (GALE) Deficiency:
- $GALE$ defect.
- Peripheral (benign): Asymptomatic; RBC/WBC enzyme defect.
- Generalized (rare): Severe; mimics classic galactosemia.
- 📌 Lens Alert: Galactitol accumulation causes osmotic damage, leading to cataracts.

⭐ GALK deficiency: cataracts are primary; liver & brain typically spared (unlike GALT deficiency).
GALT's Grave Gala - Toxic Milk Mayhem
Classic Galactosemia: Severe autosomal recessive disorder from Galactose-1-Phosphate Uridyltransferase (GALT) enzyme deficiency. Results in toxic accumulation of Galactose-1-Phosphate and Galactitol.
-
Pathophysiology:
-
Clinical Features (Neonatal onset after milk ingestion):
- Jaundice, hepatosplenomegaly, liver failure
- Vomiting, diarrhea, failure to thrive (FTT)
- Cataracts (oil-droplet, develop rapidly)
- Aminoaciduria, renal tubular dysfunction
- Lethargy, hypotonia; intellectual disability if untreated
⭐ High risk of neonatal E. coli sepsis.
-
Diagnosis:
- ↑ Blood galactose, ↑ Galactose-1-P in RBCs
- ↓ GALT enzyme activity in RBCs (confirmatory)
- Urine: +ve reducing substances (non-glucose)
- Newborn screening (NBS) crucial.
-
Management:
- Prompt initiation of galactose-restricted (lactose-free) diet.
- Soy-based formula.
- Monitor for long-term complications (e.g., premature ovarian insufficiency in females, developmental delay). 📌 GALT: Grave Ailments from Lactose Toxicity.
High‑Yield Points - ⚡ Biggest Takeaways
- Essential Fructosuria: Fructokinase defect; benign, asymptomatic, urinary fructose (reducing substance).
- Hereditary Fructose Intolerance (HFI): Aldolase B defect; severe hypoglycemia, jaundice post-fructose. Fructose-1-P toxic.
- Classic Galactosemia: GALT defect; cataracts, hepatomegaly, E. coli sepsis. Galactose-1-P toxic.
- Galactokinase Deficiency: GALK defect; infantile cataracts from galactitol. Otherwise milder.
- Aldolase B & GALT defects: toxic phosphorylated intermediates accumulate.
- Key treatment: Strict dietary restriction of offending sugars.
- Cataracts in galactosemia (GALT/GALK) from galactitol accumulation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

