Postoperative Respiratory Care: Risks & Realities - Breathing After Bliss
Surgery & anesthesia significantly impact lung function, increasing postoperative pulmonary complication (PPC) risk.
- Physiological Insults:
- ↓ Functional Residual Capacity (FRC) by 20-30% (most critical)
- ↓ Tidal Volume (TV) & Vital Capacity (VC)
- Impaired cough & mucociliary clearance
- Diaphragmatic dysfunction
- Key Risk Factors (Illustrative, e.g., ARISCAT components):
- Age >60 yrs
- Pre-existing respiratory disease (COPD, asthma)
- Smoking, Obesity (BMI >30 kg/m²)
- Surgical site (thoracic/upper abdominal)
- Surgery duration >2-3 hrs
- Emergency surgery
- Low preoperative SpO₂ <96%

⭐ The most common cause of early postoperative hypoxemia (first 24-48 hours) is atelectasis.
Postoperative Respiratory Care: PORCs Parade - When Breaths Go Bad
⭐ Atelectasis is the most common postoperative respiratory complication, typically occurring within 48 hours after surgery.
Common PORCs and their features:
| Complication | Onset | Key Symptoms | CXR Findings |
|---|---|---|---|
| Atelectasis | 24-48h | Fever, ↓breath sounds, tachypnea | Lobar collapse, opacification, mediastinal shift to affected side |
| Pneumonia | >48h | Productive cough, fever, dyspnea, crackles | Consolidation, infiltrates |
| Bronchospasm | Intra/Early Postop | Wheezing, dyspnea, ↑peak airway pressures | Often normal; hyperinflation |
| Pulmonary Embolism (PE) | Variable (3-7d) | Sudden dyspnea, pleuritic pain, tachypnea | Often normal; Westermark sign, Hampton's hump (rare) |
- Risk Factors: Smoking, obesity, COPD, prolonged/thoracic/upper abdominal surgery.
- Prevention: 📌 I COUGH: Incentive spirometry, Coughing/deep breathing, Oral care, Understanding (patient education), Getting up (mobilization), Head elevation.
- Management: Treat cause; O2, physio; specific Rx (antibiotics, bronchodilators, anticoagulants).
Postoperative Respiratory Care: Preventive Playbook - Stop Trouble Starting
📌 LUNG SAFE approach: Lung expansion, Upright position, Non-invasive ventilation (if indicated), Good analgesia, Stop smoking/Secretions clear, Ambulation/Activity, Fluid balance, Early recognition.
- Pre-operative:
- Smoking cessation: 4-8 weeks prior.
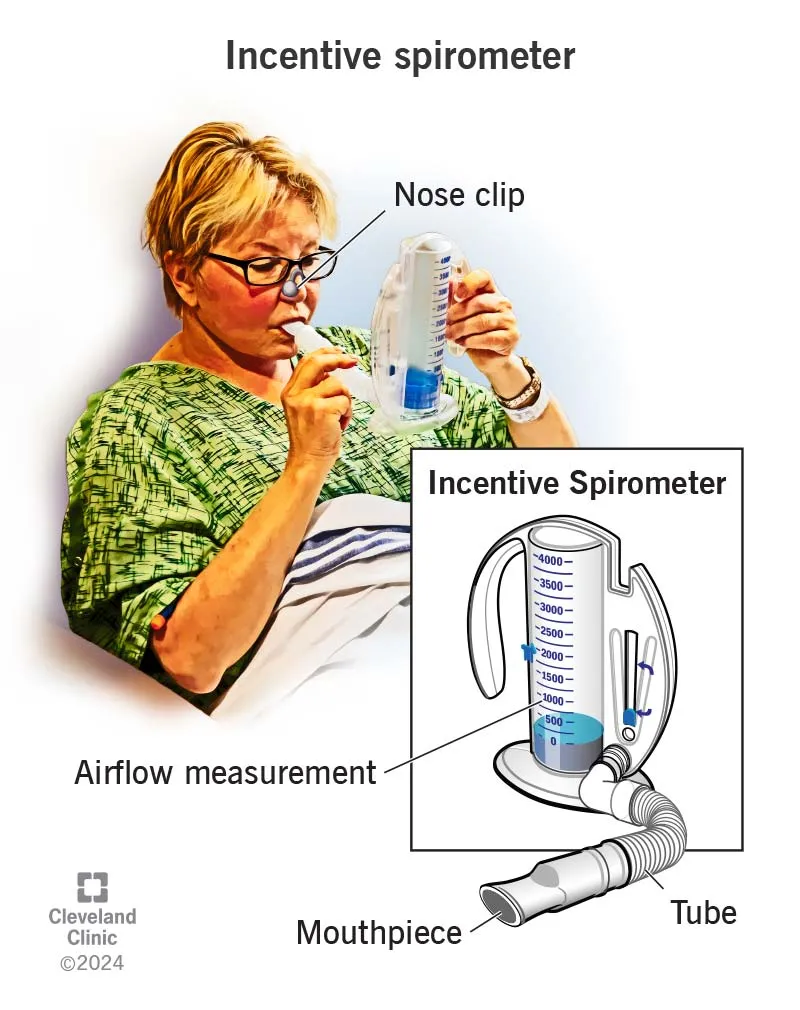
- Patient education on Deep Breathing Exercises (DBE) & Incentive Spirometry (IS).
- Intra-operative:
- Lung protective ventilation strategies.
- Post-operative:
- Effective analgesia (e.g., epidural, nerve blocks).
- Early mobilization & upright positioning.
- Lung expansion maneuvers:
- DBE, directed cough.
- Incentive Spirometry: 5-10 breaths/hour while awake.
- Chest Physiotherapy (CPT) for high-risk patients.
- Humidified oxygen if $SpO_2 < \textbf{92}%$.
- Consider CPAP/BiPAP for high-risk (e.g., OSA, COPD).
⭐ Adequate postoperative pain control, particularly with regional anesthesia or multimodal analgesia, is paramount for effective respiratory physiotherapy and prevention of Postoperative Respiratory Complications (PORCs).
Postoperative Respiratory Care: Response & Rescue - Fixing Faulty Flows
- Airway Patency: Head-tilt/chin-lift, jaw thrust. OPA/NPA. Suction. Consider LMA/ETT if refractory.
- Optimize Oxygenation: Titrate FiO₂ (Nasal cannula, Venturi, NRBM) to SpO₂ >92% (88-92% COPD). Consider CPAP/BiPAP for atelectasis/Type I failure.
- Support Ventilation: Address hypoventilation (reverse opioids/NMB). Mechanical ventilation if respiratory muscle fatigue/Type II failure.
- Specific Causes & Fixes:
- Atelectasis: Chest physiotherapy, incentive spirometry.
- Bronchospasm: Inhaled β₂-agonists.
- Pulmonary edema: Diuretics, PEEP.
- PE: Anticoagulation.
- Pneumonia: Antibiotics.
⭐ For suspected postoperative pulmonary embolism, a Wells score followed by D-dimer or CT pulmonary angiography (CTPA) is the standard diagnostic pathway.
High‑Yield Points - ⚡ Biggest Takeaways
- Atelectasis: Most common postoperative pulmonary complication, typically within 24-48 hours.
- Prevention: Incentive spirometry, deep breathing exercises, and early mobilization are key.
- Hypoxemia (PaO2 < 60 mmHg or SpO2 < 90%) requires prompt oxygen and evaluation.
- Risk factors: Obesity, smoking, COPD, thoracic/upper abdominal surgery.
- Pulmonary embolism (PE): Suspect with sudden dyspnea, chest pain, and unexplained hypoxemia.
- Aspiration pneumonitis: High risk with impaired consciousness or delayed gastric emptying.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

