Definition & Pathophysiology - Headache Horror
- Definition: Postural headache, typically bilateral, fronto-occipital. Onset usually 24-72h post-dural puncture.
- Incidence: Higher in obstetric patients. ↑ with larger needle size & cutting needles (vs. pencil-point).
- Pathophysiology: CSF leakage → ↓ CSF volume & pressure.
- Brain sag → traction on pain-sensitive structures (meninges, vessels, nerves).
- Compensatory cerebral vasodilation.
- Monro-Kellie doctrine: ↓CSF volume → intracranial hypotension.
⭐ Classic PDPH is postural, worsening on sitting/standing and relieved by lying flat. oka
Risk Factors - Who Gets Hit?
- Patient Factors:
- Younger age, female sex, pregnancy (all ↑ risk)
- Prior PDPH, low BMI (both ↑ risk)
- Connective tissue disorders (e.g., Marfan) (↑ risk)
- Procedural Factors:
- Needle: ↑ gauge (e.g., 22G), cutting tip (Quincke) vs. ↓ gauge, pencil-point (Sprotte, Whitacre)
- 📌 Mnemonic: "SPiN" - Sprotte Pencil-point is Non-cutting (↓ PDPH)
- Bevel (cutting needles): Perpendicular to dural fibers (↑ risk) vs. parallel (↓ risk)
- Multiple attempts, operator inexperience (both ↑ risk)
- Loss of resistance: Air vs. saline (air ↑ risk? - controversial)
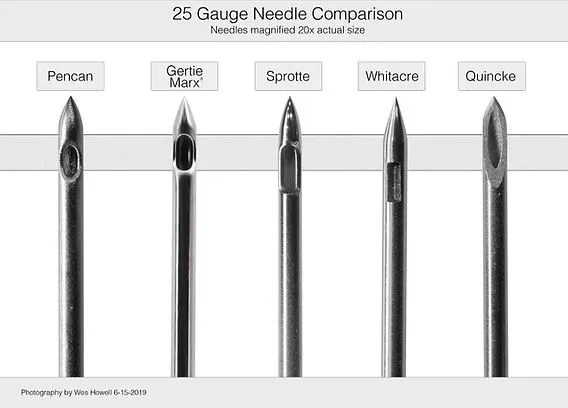
- Needle: ↑ gauge (e.g., 22G), cutting tip (Quincke) vs. ↓ gauge, pencil-point (Sprotte, Whitacre)
⭐ Use of smaller gauge, non-cutting (pencil-point) needles (e.g., Sprotte, Whitacre) significantly reduces PDPH incidence.
Clinical Features & Diagnosis - Spotting the Villain
⭐ Hallmark: Postural nature (worsens upright within 15-30 min, relieved supine within 15-30 min).
- Key Symptoms: 📌 POSTURAl H:
- Postural, Occipital/frontal
- Stiff neck, Tinnitus
- Upright worsening, Recumbent relief
- Associated (Nausea/Vomiting, photophobia, phonophobia)
- Lightheadedness, Headache (often bilateral, throbbing/dull).
- Onset: Typically 24-72h post-puncture. Duration: Self-limiting (days to 2 weeks).
- Diagnosis: IHS criteria (history of dural puncture, characteristic postural headache, specific timing).
- Key Differentials: Migraine, tension headache, meningitis, sinusitis, pre-eclampsia headache, Cerebral Venous Thrombosis (CVT).
- Red Flags: Fever, focal neurological deficits, non-postural nature, sudden severe onset, altered sensorium.
Prevention Strategies - Dodging the Doom
- Procedural (📌 PREVENT):
-
Pencil-point/atraumatic needles (e.g., Sprotte, Whitacre).
-
Re-insert stylet before withdrawal.
-
Experienced operator; limit attempts.
-
Vigilant bevel: For cutting needles, orient parallel to dural fibres.
-
Effective (smallest) gauge (e.g., 25-27G Sprotte).
-
No multiple attempts.
-
Technique: Median/paramedian approach.
⭐ Orienting the bevel of a cutting needle parallel to the longitudinal dural fibres is a key preventive measure if such a needle is used.
-
- Patient Positioning: Post-puncture position lacks strong evidence for prevention.
- Prophylaxis:
- Routine Epidural Blood Patch (EBP): Not generally recommended.
- Fluids: Maintain hydration; limited prevention evidence.
- Drugs (caffeine, cosyntropin, sumatriptan): Evidence lacking/controversial for prevention.
Management Options - Taming the Pain
- Conservative (First-line): 📌 Mnemonic: "B-HAC"
- Bed rest (supine position).
- Hydration (oral/IV).
- Analgesics (simple): Paracetamol, NSAIDs.
- Caffeine: Oral 300-500mg; IV 500mg (caffeine sodium benzoate).
- Pharmacological (Limited/Equivocal Evidence; Not First-Line):
- Gabapentin, hydrocortisone, theophylline, sumatriptan.
- Invasive Procedures:
- Epidural Blood Patch (EBP):
⭐ Epidural Blood Patch (EBP) using 15-20 mL of autologous blood is the gold standard treatment for severe or persistent PDPH.
- Technique: Aseptic injection into epidural space (at/below puncture level).
- Success rate: >90%.
- Complications: Backache (common), repeat PDPH.
- Sphenopalatine Ganglion Block (SPGB): Emerging option.
- Epidural Blood Patch (EBP):

High‑Yield Points - ⚡ Biggest Takeaways
- PDPH is a postural headache (worse upright, relieved supine) after neuraxial block, due to CSF leakage.
- Onset typically 24-48 hours post-dural puncture, often fronto-occipital.
- Key risk factors: large-bore cutting needles, young age, female sex, pregnancy, multiple attempts.
- Prevention: Use small-gauge, pencil-point needles (e.g., Sprotte, Whitacre).
- Conservative management: Bed rest, hydration, analgesics, caffeine.
- Epidural Blood Patch (EBP) is the gold standard treatment for severe or refractory PDPH.
- Associated symptoms: Nausea, neck stiffness, photophobia, tinnitus may occur.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

