Cardiac Conditions - Heartfelt Hurdles
- Pregnancy: ↑CO, ↑HR, ↑BV; ↓SVR. Goals: Hemodynamic stability, avoid pain/stress.
- Key Lesions & Goals:
- MS: Slow HR, maintain preload/SVR. Avoid ↑PVR. Epidural preferred.
- AS (Critical): Maintain NSR, preload, SVR. Avoid ↓SVR (spinal dangerous!). Slow epidural/CSE.
- PHTN: Maintain SVR, RV function. Avoid ↑PVR (hypoxia, acidosis, pain).
- PPCM: LV dysfunction (EF <45%) late pregnancy/postpartum. Avoid myocardial depressants.
- Anesthesia: Regional (epidural) often preferred for slow, controlled onset.
⭐ Eisenmenger syndrome carries the highest maternal mortality risk (30-50%) among cardiac conditions.
Respiratory & Hypertensive - Breathless & Pressured
- Respiratory (Pregnancy):
- ↑MV (50%), ↑O₂ use; ↓FRC (20%) → rapid desat.
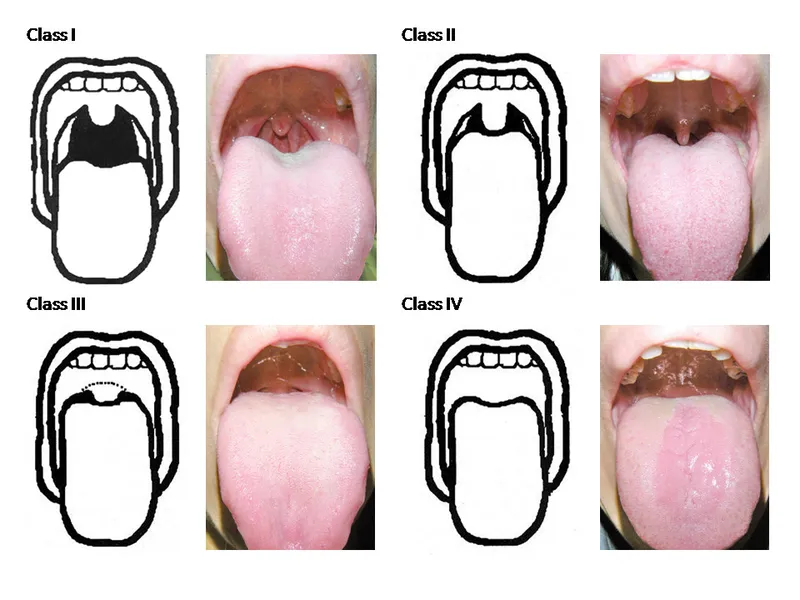
- Airway: Edema, friable, ↑Mallampati. 📌 Difficult intubation risk.
- Resp. alkalosis ($P_{aCO_2}$ 28-32 mmHg).
- Hypertension (Preeclampsia/Eclampsia):
- Preeclampsia: BP ≥140/90 mmHg (post 20wks) + proteinuria/end-organ damage.
- Severe: BP ≥160/110 mmHg, HELLP, pulm. edema, CNS.
- MgSO₄ for seizures (Load: 4-6g IV; Maint: 1-2g/hr).
- ⚠️ Toxicity: ↓DTRs, resp. depression. Antidote: Ca gluconate.
- Definitive: Delivery.
- Anesthesia: Neuraxial preferred (platelets >75,000/μL). GA: RSI, small ETT.
⭐ MgSO₄ is key for eclampsia seizure prophylaxis/treatment. Therapeutic range 4-7 mEq/L. Monitor DTRs, RR. Antidote: Ca gluconate.
Endocrine & Hematological - Metabolic Mayhem
-
Diabetes Mellitus (DM)
- Pre-gestational / Gestational (GDM).
- Target: Euglycemia (<140/80-110mg/dL intrapartum).
- Neonate: Hypoglycemia risk.
- Anes: Neuraxial pref. GA: DKA/asp. risk. Insulin.
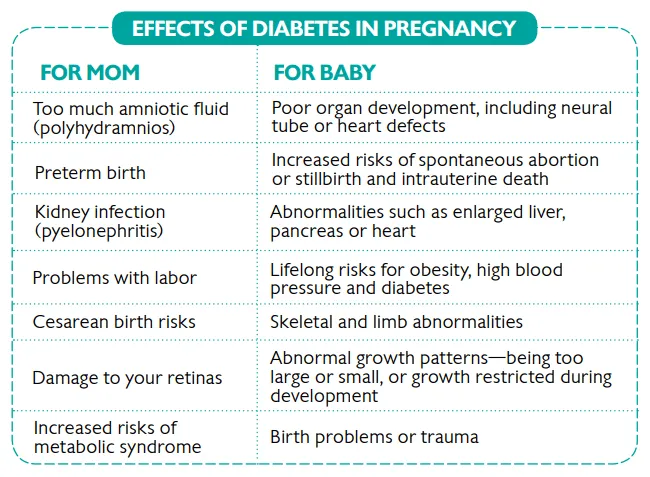
⭐ Hyperglycemia teratogenic; tight glycemic control vital preconception/early pregnancy.
-
Thyroid Disorders
- Hyperthyroidism:
- Risk: Thyroid storm (surgery/infection trigger).
- Rx: PTU, methimazole, β-blockers. Avoid ketamine.
- Neuraxial preferred.
- Hypothyroidism:
- Risk: Myxedema coma (rare).
- Rx: Levo. ↑Sedative/opioid sensitivity.
- Hyperthyroidism:
-
Hematological Issues
- Anemia:
- Common: Iron deficiency.
- Thresholds: Hb <11(T1/3), <10.5(T2) g/dL.
- Optimize. Transfuse Hb <7-8/symptomatic.
- Thrombocytopenia:
- Gestational: Mild, PLT >70k/µL.
- Others: ITP, HELLP.
- Neuraxial: PLT >80k (trend/cause). ⚠️ No NSAIDs.
- Coagulopathy & Anticoagulation:
- VWD: DDAVP/Factor VIII.
- Anticoagulants: Neuraxial timing critical (LMWH: 12h off proph, 24h off therap).
- Anemia:
Obesity & Neurological - Weighty Nerves
- Obesity (BMI ≥30 kg/m²):
- Challenges: Difficult airway (OSA), ↓FRC, positioning, co-morbidities (HTN, GDM).
- Anesthesia: RSI for GA. Regional (epidural/CSE) preferred; USG for placement. Adjust LA dose.
- Risks: ↑Aspiration, VTE, infection. 📌 RAMP positioning for intubation.
- Neurological Disorders:
- Epilepsy: Continue AEDs. Regional preferred. Avoid pro-convulsants (e.g., meperidine).
- Multiple Sclerosis: Avoid hyperthermia. Epidural preferred over spinal.
- Myasthenia Gravis: ↑Sensitivity to NDMRs. Regional ideal.
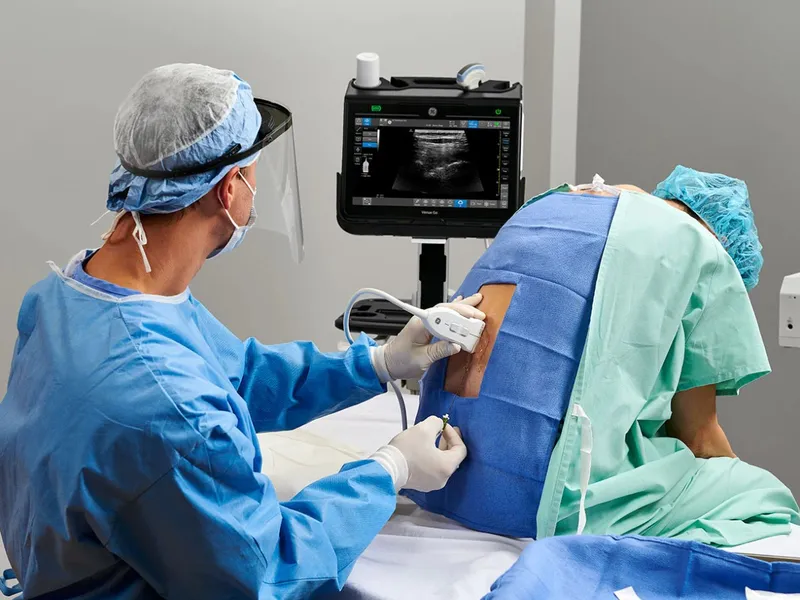
⭐ For obese parturients, reduce epidural local anesthetic dose by 20-25% due to decreased epidural space volume from engorged veins.
High‑Yield Points - ⚡ Biggest Takeaways
- Cardiac Disease: Epidural preferred for minimal hemodynamic change; avoid aortocaval compression.
- Preeclampsia: Magnesium sulfate for seizures. Neuraxial for C-section if no coagulopathy/severe thrombocytopenia.
- Obesity: High risk: difficult airway, aspiration. Early epidural placement is key.
- Asthma: Continue therapy. Regional anesthesia preferred; avoid histamine-releasing drugs.
- Thrombocytopenia: Neuraxial safe if platelets >80,000/µL; <50,000/µL relative contraindication.
- Gestational Diabetes: Maintain euglycemia to prevent macrosomia, neonatal hypoglycemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

