NMDs Overview - Nerve-Muscle Maze
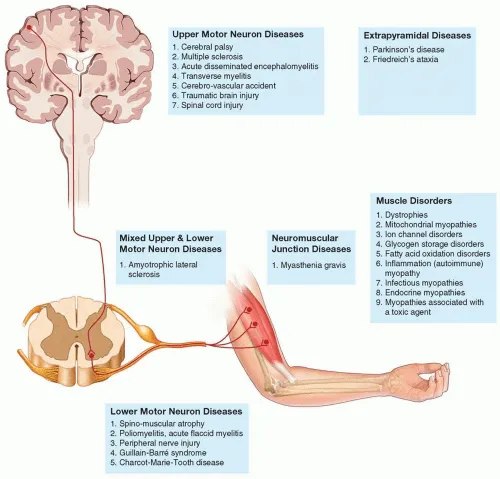
Neuromuscular disorders (NMDs) impair function of motor units: anterior horn cells, peripheral nerves, neuromuscular junction (NMJ), or muscles.
- Key Types:
- Motor Neuron Diseases (e.g., ALS)
- Peripheral Neuropathies (e.g., GBS)
- NMJ Disorders (e.g., Myasthenia Gravis, LEMS)
- Myopathies (e.g., Dystrophies, Myotonias)
- Anesthetic Focus:
- Pre-op assessment of system involvement.
- Careful airway & respiratory management.
⭐ General increased sensitivity to non-depolarizing NMBs and risk with succinylcholine in many NMDs.
Myasthenia Gravis & LEMS - Junction Function Fracas
- Myasthenia Gravis (MG):
- Patho: Postsynaptic ACh receptor antibodies.
- Clinical: Fluctuating, fatigable weakness (ocular, bulbar, limb). Improves with rest. Thymoma association.
- Anesthesia:
- NDMRs: Extreme sensitivity (use 1/10th - 1/20th dose). Titrate carefully.
- Succinylcholine: Relative resistance (may need 1.5-2 mg/kg).
- Avoid: Aminoglycosides, quinolones, $Mg^{2+}$, β-blockers.
- Post-op: High risk of respiratory failure. Continue pyridostigmine.
- Lambert-Eaton Myasthenic Syndrome (LEMS):
- Patho: Presynaptic P/Q-type $Ca^{2+}$ channel antibodies → ↓ACh release.
- Clinical: Proximal weakness, improves with brief exercise. Autonomic features. Strong SCLC link.
- Anesthesia:
- NDMRs & Succinylcholine: Increased sensitivity to both (↓ doses).
- Volatile-sparing techniques preferred.
⭐ Myasthenia Gravis patients show marked sensitivity to non-depolarizing muscle relaxants, requiring dose reduction to 1/10th to 1/20th of the usual dose.

Muscular Dystrophies - Muscle Under Siege
- Hereditary, progressive muscle weakness, degeneration.
- Duchenne Muscular Dystrophy (DMD):
- X-linked; absent dystrophin. Onset 2-5 yrs. Gower's sign.
- Systemic: Cardiomyopathy (dilated), respiratory failure (restrictive), scoliosis.
- Anesthesia:
- ⚠️ NO Succinylcholine (hyperkalemia, rhabdomyolysis).
- ↑ Sensitivity to NDMRs; titrate carefully.
- MH risk: Be prepared (controversial).
- Aspiration risk. Regional preferred.
⭐ Succinylcholine is absolutely contraindicated in Duchenne Muscular Dystrophy due to risk of hyperkalemic cardiac arrest and rhabdomyolysis.
- Becker Muscular Dystrophy (BMD):
- Milder, later onset. Dystrophin abnormal/reduced. Similar concerns to DMD, less severe.
- General Anesthetic Points:
- Pre-op: Cardiac/Respiratory evaluation crucial.
- Careful positioning. Post-op respiratory care.

Other NMDs & Peri-op Pearls - Navigating Neuro-Weakness
- General NMD Peri-op Goals: Maintain muscle strength, ensure adequate ventilation, prevent complications (e.g., aspiration, rhabdomyolysis).
- Lambert-Eaton (LEMS): ↑ Sensitivity to both NDMRs & SCh. Pre-synaptic VGCC Ab. Improvement with activity.
- Periodic Paralysis:
- HypoKPP: Triggered by CHO, rest post-exercise. Avoid glucose loads, K⁺-wasting drugs. Acetazolamide.
- HyperKPP: Triggered by K⁺, fasting, cold. Avoid K⁺, SCh. Glucose + insulin for acute attacks.
- Congenital Myopathies: Variable SCh response; potential MH risk (e.g., Central Core Disease). Biopsy key.
⭐ In Guillain-Barré Syndrome, autonomic dysfunction is common, requiring careful hemodynamic management and avoidance of succinylcholine due to upregulation of ACh receptors.
High‑Yield Points - ⚡ Biggest Takeaways
- Myasthenia Gravis: ↑ sensitivity to NDMRs, resistance to succinylcholine; risk of postoperative respiratory failure.
- LEMS: ↑ sensitivity to both succinylcholine and NDMRs; strength improves with activity.
- Muscular Dystrophies (e.g., Duchenne): Avoid succinylcholine (risk of hyperkalemia, rhabdomyolysis); ↑ MH susceptibility.
- Myotonic Dystrophy: Myotonic crisis with succinylcholine or neostigmine; avoid succinylcholine.
- Guillain-Barré Syndrome: Risk of autonomic instability and hyperkalemia with succinylcholine.
- Regional anesthesia is often preferred when possible in these patients.
- Vigilant postoperative respiratory monitoring is critical for all neuromuscular disorders.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

