Pre-Op Neuro Check - Brainy Blueprint
- Objective: Baseline neuro status, risk identification, surgical optimization.
- BRAINY Assessment (📌):
- Baseline: GCS (e.g., < 8), focal deficits, pupils.
- Review Imaging: CT/MRI/Angio for lesion, edema, shift.
- Airway & C-spine: Assess difficulty, instability.
- ICP Signs: Headache, N/V, papilledema. Note Cushing's Triad (HTN, bradycardia, irregular respirations).
- Necessary Labs: Coags (PT/INR, aPTT), electrolytes, glucose.
- Your Meds: Antiplatelets (Aspirin hold 5-7 days), anticoagulants, anticonvulsants.
⭐ Cushing's triad (hypertension, bradycardia, irregular respirations) is a late, critical sign of markedly ↑ICP_._
Intra-Op Watchtower - Neuro-Guardians
Core Goals: Maintain CPP, ↓CMRO2, neuroprotection, surgical access, rapid emergence.
Key Monitoring:
- Standard ASA + IBP (A-line).
- Neuro-Specific:
- EEG: Ischemia/seizures. Burst suppression: 1-5 bursts/min.
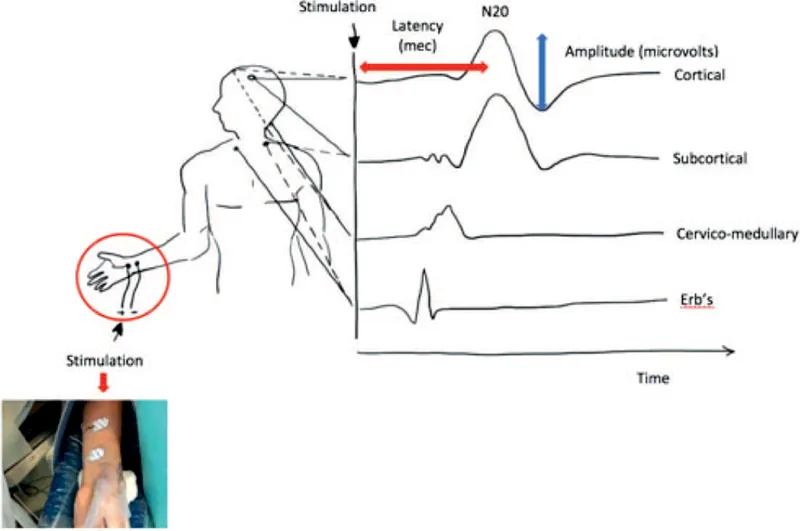
- Evoked Potentials (EPs):
- SSEP: Dorsal column. Alarm: ↓50% amplitude, ↑10% latency.
- MEP: Corticospinal tract. Alarm: ↓>50-80% amplitude. (NMB caution)
- BAEP: Brainstem.
- NIRS (Cerebral Oximetry): rSO2. Alarm: ↓20-25% baseline or <50-55%.
- TCD: Blood flow velocities.
Management Pearls:
- MAP targets: Procedure-specific (e.g., controlled hypotension).
- Ventilation: Normocapnia (PaCO2 35-40 mmHg).
- Brain relaxation: Mannitol ($0.25-1 \text{ g/kg}$), HTS.
- Temperature: Avoid hyperthermia.
⭐ During temporary aneurysm clipping, a >50% drop in SSEP/MEP amplitude warns of ischemia, may need clip adjustment.
Anesthesia Arsenal - Brain's Best Friends
- Goal: ↓ICP, ↓CMRO₂, maintain CPP, optimize surgical field.
- Induction:
- Propofol: ↓CMRO₂/ICP/MAP. ICP dose: 1-2 mg/kg.
- Etomidate: Stable hemodynamics, ↓CMRO₂/ICP. Risk: adrenal suppression.
- Thiopental: Potent ↓CMRO₂/ICP.
- Maintenance - Inhalational:
- Isoflurane, Sevoflurane: ↓CMRO₂. Keep <1 MAC (risk ↑CBF/ICP).
- N₂O: Generally avoid (↑CBF, pneumocephalus).
- Opioids:
- Remifentanil, Fentanyl: ↓CMRO₂. Minimal direct CBF/ICP effects.
- Muscle Relaxants:
- Non-depolarizing (e.g., Vecuronium): Preferred.
- Succinylcholine: Transient ↑ICP; consider defasciculation.
- ICP Management Adjuncts:
- Lidocaine IV: 1.5 mg/kg (pre-intubation).
- Mannitol: 0.25-1 g/kg. Hypertonic Saline (HTS).
⭐ Propofol is favored in neuroanesthesia: it reduces CMRO₂, CBF, and ICP, while preserving cerebrovascular CO₂ reactivity.
Vascular Hotspots - Procedure Playbook
- Universal: Maintain CPP (60-70 mmHg), brain relaxation, smooth emergence. IABP, neuromonitoring.
- Pharmacology: TIVA (Propofol/Remifentanil). Avoid N₂O, Ketamine (if ↑ICP).
| Procedure | Focus | BP Targets (Pre/Intra) | Notes |
|---|---|---|---|
| Aneurysm Clipping | Controlled hypotension, brain protection. | MAP 50-60 / ↓30% (pre-clip) | Vasospasm. Post-clip: normo/mild ↑BP. |
| Coiling/Embolization | Immobility, anticoagulation (ACT 250-300s). | Normotension / slight ↓ | Rupture, thromboembolism. Protamine. |
| AVM Resection | Controlled hypotension, prevent NPPB. | ↓MAP; Post-op: strict normotension | NPPB, hemorrhage. |
| CEA | Maintain CBF (clamp), tight BP control. | Baseline/Slight ↑ (clamp) | Stroke, MI. Neuromonitoring. |
⭐ During temporary aneurysm clipping, induced hypotension or brief adenosine-induced asystole can facilitate clip placement.
High‑Yield Points - ⚡ Biggest Takeaways
- Optimize Cerebral Perfusion Pressure (CPP), typically 60-80 mmHg, avoiding hypotension.
- Induced hypotension is a key strategy for aneurysm surgery to minimize bleeding.
- Rapid, smooth emergence is vital for immediate neurological assessment.
- Aggressively manage Intracranial Pressure (ICP), targeting <20 mmHg.
- Utilize neuromonitoring (e.g., SSEP, MEP, EEG) to detect ischemia early.
- Maintain normoglycemia and normothermia for optimal neuroprotection.
- Thrombectomy anesthesia: balance between GA and MAC based on patient stability.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

