Physicochemical Properties - Chemical Keys Unlock Action
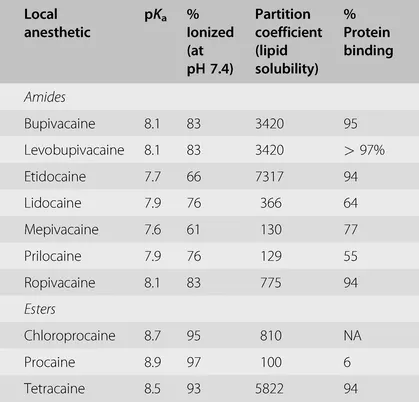
- pKa: Acidity constant; typical LA range 7.6-8.9. Governs onset speed.
- Lower pKa → more non-ionized drug at physiologic pH → faster nerve penetration → quicker onset. 📌 Low pKa = Earlier Start.
- Lipid Solubility: Higher solubility → greater potency (easier membrane passage).
- Protein Binding: Higher binding (mainly to α1-acid glycoprotein) → longer duration of action.
- Ionization: LAs are weak bases. Ionized (cationic) form is active intracellularly; non-ionized form crosses membranes. Governed by Henderson-Hasselbalch: $pH = pKa + log([A⁻]/[HA])$.
- Impact Summary:
Property Primary Effect Clinical Implication ↓ pKa Onset Faster onset ↑ Lipid Solubility Potency More potent ↑ Protein Binding Duration Longer duration
⭐ Local anesthetics with lower pKa values have a faster onset of action because a higher fraction of the drug is in the non-ionized form at physiological pH, allowing for more rapid diffusion across nerve membranes.
Absorption of LAs - Getting into System
- Factors:
- Site Vascularity: ↑ vascularity → ↑ absorption.
- Dose: ↑ dose → ↑ absorption.
- Lipid Solubility: ↑ solubility → ↑ absorption.
- Vasoconstrictors: Epinephrine (e.g., 1:200,000) ↓ absorption, prolongs action, ↓ toxicity.
⭐ Vasoconstrictors (e.g., epinephrine) decrease LA systemic absorption, prolonging anesthesia and reducing toxicity.
- Site Absorption Rate (Fastest → Slowest): 📌 IV TICS EBS: IV > Tracheal > Intercostal > Caudal > Epidural > Brachial Plexus > Sciatic > Subcutaneous.
Distribution of LAs - Spreading the Numbness
- Tissue Perfusion: High perfusion (brain, liver) = rapid uptake.
- Protein Binding: Binds α1-acid glycoprotein (AAG); ↑ binding = ↓ free drug, longer action.
- Lipid Solubility: ↑ lipid solubility = ↑ potency, ↑ duration, ↑ Vd, ↑ protein binding.
- Volume of Distribution (Vd): ↑ with lipid solubility.
- Special Barriers:
- Placental Transfer: Crosses placenta; fetal risk.
- Blood-Brain Barrier (BBB) Penetration: Crosses BBB; CNS toxicity risk.
⭐ Highly lipid-soluble local anesthetics generally have a larger volume of distribution (Vd), greater protein binding, and a longer duration of action.
Metabolism of LAs - Breaking It Down
📌 Mnemonic: Esters (one 'i', e.g., Procaine) vs. Amides (two 'i's, e.g., Lidocaine). Articaine: amide with ester linkage.
Key differences in metabolism:
| Feature | Ester LAs | Amide LAs |
|---|---|---|
| Enzyme | Plasma Pseudocholinesterase | Liver Microsomal Enzymes (CYP450) |
| Location | Plasma | Liver |
| Speed | Rapid | Slower |
| Byproduct | PABA (→ Allergic reactions) | Various (less allergenic) |
| Clinical Note | Caution: Pseudocholinesterase deficiency | Caution: Liver disease, enzyme interactions |
| %%{init: {'flowchart': {'htmlLabels': true}}}%% | ||
| flowchart TD |
Start["💉 Local Anesthetics
• Pain management• Sodium blockers"]
Route{"🔄 Route?
• Metabolism path• Chemical class"}
EsterEnz["🧪 Ester Enzyme
• Pseudocholinesterase• Plasma location"]
EsterSpeed["⚡ Ester Speed
• Rapid hydrolysis• Short duration"]
EsterBy["⚠️ Ester Byproduct
• PABA byproduct• High allergy risk"]
AmideEnz["🧪 Amide Enzyme
• Hepatic CYP450• Liver location"]
AmideSpeed["⏳ Amide Speed
• Slower clearance• Longer duration"]
AmideBy["📦 Amide Byproducts
• Various metabolites• Lower allergy rate"]
AmideNote["🩺 Clinical Note
• Liver disease risk• Drug interactions"]
Start --> Route Route -->|Ester LAs| EsterEnz EsterEnz --> EsterSpeed EsterSpeed --> EsterBy
Route -->|Amide LAs| AmideEnz AmideEnz --> AmideSpeed AmideSpeed --> AmideBy AmideBy --> AmideNote
style Start fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534 style Route fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style EsterEnz fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style EsterSpeed fill:#F6F5F5, stroke:#E7E6E6, stroke-width:1.5px, rx:12, ry:12, color:#525252 style EsterBy fill:#FDF4F3, stroke:#FCE6E4, stroke-width:1.5px, rx:12, ry:12, color:#B91C1C style AmideEnz fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style AmideSpeed fill:#F6F5F5, stroke:#E7E6E6, stroke-width:1.5px, rx:12, ry:12, color:#525252 style AmideBy fill:#F6F5F5, stroke:#E7E6E6, stroke-width:1.5px, rx:12, ry:12, color:#525252 style AmideNote fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8
> ⭐ Prilocaine, an amide LA, has a metabolite (o-toluidine) that can cause methemoglobinemia, especially at **high doses**.
## Excretion & Special Populations - Final Exit & Tweaks
* **Primary Route**: Renal excretion of metabolites and small amounts of unchanged drug.
- Urinary pH: Affects ionization; crucial for ion trapping.
- Renal function: Impairment ↓ excretion.
> ⭐ Acidification of urine increases the ionized fraction of local anesthetics (weak bases), thereby enhancing their renal excretion (ion trapping).
* **Special Populations**:
- Renal Disease: ↓ excretion of metabolites & some LAs; risk of toxicity.
- Liver Disease: ↓ amide LA metabolism (e.g., lignocaine); esters less affected.
- Pregnancy: ↑Vd (Volume of distribution), altered protein binding, ↑cardiac output; may require dose adjustment.
- Elderly: ↓ clearance, potentially ↑ sensitivity.
- Neonates: Immature metabolic pathways, ↓ Alpha-1-Acid Glycoprotein (AAG) levels (↑ free drug fraction).
## High‑Yield Points - ⚡ Biggest Takeaways
> * **Absorption** depends on **vascularity**, **dose**, and **vasoconstrictors** (e.g., epinephrine).
> * Higher **lipid solubility** means ↑ **potency** and ↑ **duration of action**.
> * Greater **protein binding** (to AAG) leads to ↑ **duration of action**.
> * Lower **pKa** results in a **faster onset** (more unionized form at physiological pH).
> * **Esters** (e.g., Procaine, one 'i') are metabolized by **plasma pseudocholinesterase**; **Amides** (e.g., Lidocaine, two 'i's) by **hepatic enzymes**.
> * **Systemic toxicity** correlates with **plasma drug levels**; CNS symptoms typically precede cardiotoxicity.
> * **Vasoconstrictors** (e.g., epinephrine) decrease **systemic absorption**, prolong **anesthetic duration**, and reduce **potential toxicity**.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

