Introduction to POI - Gut Gone Quiet
Postoperative Ileus (POI): A common, temporary impairment of gastrointestinal motility following surgery, leading to a functional (non-mechanical) obstruction.
- Definition: Cessation of coordinated bowel peristalsis.
- Duration: Normal physiological ileus resolves within 24-72 hours. Prolonged POI if symptoms persist >3 days.
- Symptoms: Nausea, vomiting, abdominal distension, inability to tolerate oral diet, absent flatus or bowel movement.
- Impact: Significantly ↑ hospital Length of Stay (LOS), ↑ patient morbidity, and ↑ healthcare costs.
⭐ Prolonged postoperative ileus is a major driver of increased length of hospital stay and healthcare costs after abdominal surgery.
Pathophysiology of POI - Why Guts Freeze
Postoperative Ileus (POI), or "frozen guts," is a complex multifactorial response to surgical stress, delaying recovery. Key mechanisms:
- Inflammation: Surgical trauma → pro-inflammatory cytokines (IL-6, TNF-α) ↑ & macrophage activation in gut wall.
- Neurogenic Dysregulation:
- Sympathetic overactivity ↑ (inhibits motility).
- Vagal tone ↓ (reduces prokinetic signals).
- Hormonal: Corticotropin-Releasing Hormone (CRH) ↑.
- Pharmacological:
⭐ Opioids are a primary contributor to POI by binding to mu-receptors in the gut, decreasing peristalsis and increasing sphincter tone.
- Iatrogenic: Fluid overload, electrolyte imbalances (e.g., K⁺↓).

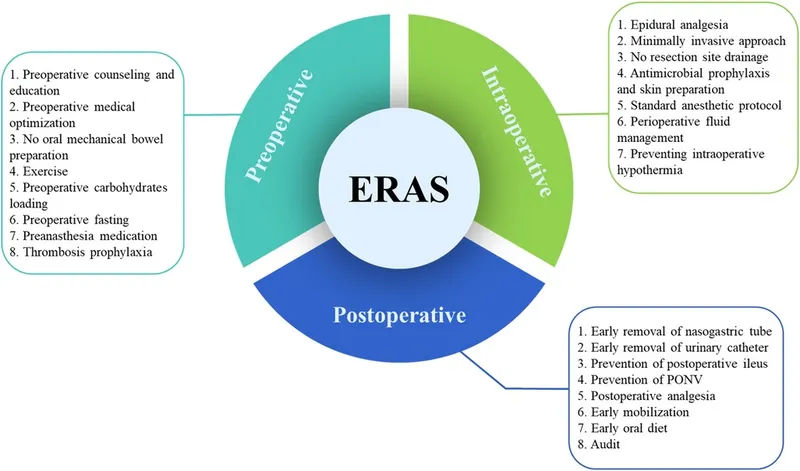
ERAS Interventions for POI - Moving Matters
A multimodal approach is key, targeting various factors across perioperative phases to prevent Postoperative Ileus (POI).
- Pre-operative:
- No Prolonged Fasting: Standard: solids 6h, clear fluids 2h pre-op. Reduces insulin resistance.
- Carbohydrate Loading: Oral carbohydrate drinks (e.g., maltodextrin) 2-3h pre-op.
- Intra-operative:
- Opioid-Sparing/Opioid-Free Anesthesia: Crucial to minimize gut dysmotility.
- Regional Anesthesia: Epidural or TAP blocks for effective, opioid-reducing analgesia.
- Goal-Directed Fluid Therapy (GDFT): Maintain euvolemia; avoid both overload and deficit.
- Minimally Invasive Surgery (MIS): Laparoscopic/robotic techniques reduce trauma.
- Post-operative:
- Early Oral Nutrition: Initiate clear liquids/diet within 24 hours.
- Early Mobilization: Ambulate from Day 0-1. 📌 Move Early And Liberally (MEAL).
- Gum Chewing: Stimulates cephalic-vagal reflex (e.g., 3 times/day for 15-30 min).
- Selective NG Tube Use: Avoid routine use; early removal if placed.
- NSAIDs/COX-2 Inhibitors: Part of multimodal analgesia to reduce opioid requirements.
⭐ Early oral feeding (within 24 hours post-surgery) is a cornerstone of ERAS protocols and significantly reduces POI.
Pharmacological Management in ERAS for POI - Drug Nudges
- Alvimopan: Peripheral mu-opioid antagonist (12mg dose) for post-bowel resection; accelerates GI recovery.
- NSAIDs: Opioid-sparing; reduce opioid-related gut dysmotility.
- IV Lidocaine Infusion: Anti-inflammatory and analgesic properties, may improve gut function.
- Magnesium: Potential benefits for gut motility, evidence evolving.
- Avoid Routine Prokinetics:
- Metoclopramide, Erythromycin.
- Limited evidence of benefit in ERAS for preventing Postoperative Ileus (POI).
⭐ Alvimopan, a peripherally acting mu-opioid receptor antagonist, is FDA-approved for accelerating GI recovery after bowel resection, typically given as a 12mg dose pre-operatively or immediately post-operatively_._
High‑Yield Points - ⚡ Biggest Takeaways
- Opioid-sparing multimodal analgesia is critical to minimize ileus.
- Prioritize early enteral feeding and ensure euvolemia, avoiding fluid overload.
- Implement early and frequent mobilization to stimulate gut motility.
- Restrict routine use of nasogastric tubes post-operatively.
- Gum chewing can act as sham feeding, promoting faster bowel function return.
- Alvimopan (selective mu-opioid antagonist) is beneficial after bowel resection.
- Thoracic epidural analgesia can reduce ileus duration and improve gut perfusion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

