Sedation & Analgesia ICU - Setting the Stage
- Goals: Ensure patient comfort, safety, anxiolysis; facilitate mechanical ventilation & procedures; reduce physiological stress.
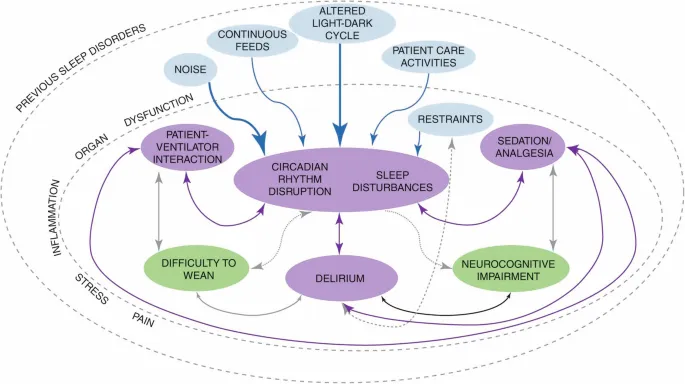
- PADIS Framework: Address Pain, Agitation/Sedation, Delirium, Immobility, and Sleep disruption.
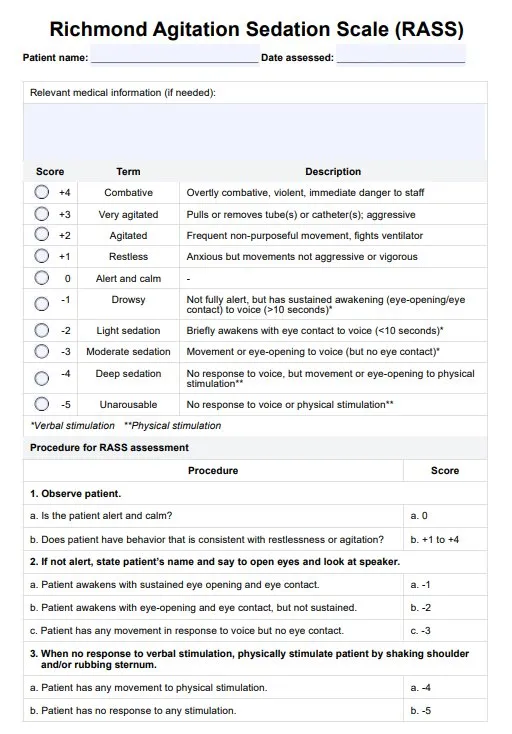
- Assessment is Key: Regularly use validated scales (e.g., CPOT/BPS for pain, RASS/SAS for sedation, CAM-ICU for delirium).
⭐ Routine pain and sedation assessment using validated scales is crucial for optimizing patient outcomes and preventing complications like prolonged ventilation.
- Analgesia First: Treat pain before sedating. "Analgosedation."
- Target Light Sedation: Aim for RASS 0 to -2 when possible. Avoid deep sedation (RASS -4 to -5) unless indicated.
- Minimize iatrogenic complications.
Sedation & Analgesia ICU - Pain Management Parade
- Pain Assessment: Use validated tools:
- Behavioral Pain Scale (BPS) for ventilated patients.
- Critical-Care Pain Observation Tool (CPOT) for all ICU patients.
- Target: BPS <5, CPOT <3.
- Analgesia-First Principle: Prioritize pain relief over sedation.
- Non-Pharmacological: Positioning, calm environment.
- Pharmacological:
- Non-Opioids: Paracetamol, NSAIDs (Ketorolac - renal/GI caution).
- Opioids (titrate to effect): Fentanyl (rapid onset, short duration), Morphine (longer; histamine, active metabolites - renal caution), Remifentanil (ultra-short; organ-independent metabolism).
- Adjuvants: Ketamine (low-dose), Gabapentinoids, Lidocaine.
⭐ Fentanyl is a common first-line ICU opioid due to its rapid onset (1-2 min IV), short duration of action (30-60 min), minimal histamine release, and lack of active metabolites, making it suitable for acute pain and hemodynamically unstable patients.
Sedation & Analgesia ICU - Sedation Station
- Goal: Titrate to RASS (Richmond Agitation-Sedation Scale) target, often -2 to 0 (light sedation).
- Key Sedatives Comparison:
| Agent | Mechanism | Onset/Duration | Metabolism | Advantages | Disadvantages | Monitoring |
|---|---|---|---|---|---|---|
| Propofol | GABA-A agonist | Rapid/Short (<10min) | Hepatic, Extrahepatic | ↓ICP, antiemetic | Hypotension, PRIS (Propofol Infusion Syndrome) | RASS, TGs, CK |
| Midazolam | GABA-A agonist | Rapid/Short-Intermed. | Hepatic (CYP3A4) | Anxiolysis, amnesia | Resp. depression, delirium, accumulation | RASS |
| Lorazepam | GABA-A agonist | Intermed./Long | Hepatic (Glucuronidation) | Longer duration | Propylene glycol toxicity (IV), delirium | RASS, renal fxn |
| Dexmedetomidine | α2-agonist | Intermed./Intermed. | Hepatic | Cooperative sedation, no resp. depression | Bradycardia, hypotension | RASS, HR, BP |
Sedation & Analgesia ICU - Smart Sedation Strategies
- Goal: Light sedation (RASS -2 to 0), analgesia-first approach.
- Key Protocols:
- Daily Spontaneous Awakening Trials (SATs) & Spontaneous Breathing Trials (SBTs).
- Prefer non-benzodiazepines (e.g., propofol, dexmedetomidine) over benzodiazepines to reduce delirium.
- ABCDEF Bundle: 📌 Awakening & Breathing Coordination, Choice of analgesia/sedation, Delirium assessment, Early mobility, Family engagement.

- Delirium Management:
- Screen daily (e.g., CAM-ICU).
- Prioritize non-pharmacological interventions.
- Use antipsychotics (e.g., haloperidol) cautiously for severe agitation.
⭐ Daily sedation interruption (SATs) significantly reduces ventilator days and ICU length of stay.
High‑Yield Points - ⚡ Biggest Takeaways
- Aim for light sedation (RASS -1 to 0) to improve ICU outcomes.
- Implement analgesia-first strategies; treat pain adequately before sedating.
- Daily sedation interruptions (SATs) reduce ventilation time and ICU stay.
- Propofol: rapid control, risk of PRIS; monitor triglycerides and CK.
- Avoid benzodiazepines if possible due to ↑ delirium and prolonged ventilation.
- Dexmedetomidine: cooperative sedation, minimal respiratory depression; watch for hypotension/bradycardia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more