Myocardial Protection - Heart Shield Basics
- Definition: Protecting the heart from injury, especially during periods of reduced blood flow (ischemia) and subsequent reperfusion.
- Primary Goals:
- Prevent myocardial ischemia & arrhythmias.
- Reduce infarct size if ischemia occurs.
- Preserve left ventricular (LV) function.
- Pathophysiology Core: Imbalance between myocardial oxygen supply ($O_2$ Supply) and demand ($MVO_2$).
- Key determinants of $MVO_2$: Heart Rate (HR), Myocardial Wall Tension (preload/afterload), Contractility.
- 📌 Mnemonic for $MVO_2$ determinants: HWC (HR, Wall tension, Contractility).
- Simplified $MVO_2$ representation: $MVO_2 \approx HR \times SBP \times Contractility$.
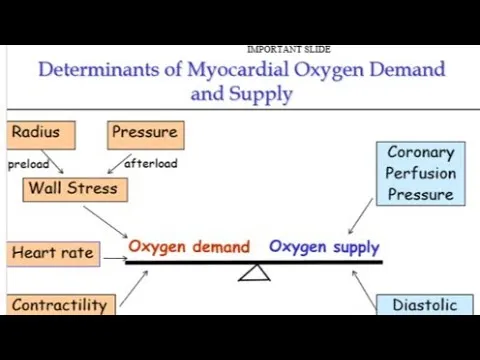
⭐ The primary goal of myocardial protection is to maintain the delicate balance between myocardial oxygen supply and demand, especially during periods of stress like surgery.
Pharmacological Strategies - Drug Defense Force
| Drug Class | Examples | Mechanism of Protection | Key Considerations/Doses |
|---|---|---|---|
| Beta-blockers | Metoprolol, Esmolol | ↓MVO₂, ↓HR, ↓Contractility, ↑Diastolic time, Anti-arrhythmic | Metoprolol 25-50mg PO / 1-5mg IV. Target HR 55-70 bpm. 📌 C/I: ABCDE. |
| Nitrates | GTN | Venodilation (↓Preload), Coronary vasodilation (↑Supply) | GTN IV 5-200 mcg/min. Monitor BP. |
| Statins | Atorvastatin, Rosuvastatin | Pleiotropic: ↓Inflammation, Endothelial & Plaque stabilization | Continue peri-op if chronic use. |
| Antiplatelet Agents | Aspirin, P2Y12 inhibitors (Clopidogrel) | ↓Platelet aggregation, ↓Thrombus formation | Aspirin 75-150mg OD. Balance bleed/ischemia risk. |
| $Ca^{2+}$ Channel Blockers | Diltiazem, Verapamil | Coronary vasodilation, ↓Afterload. Limited role. | Limited role. For vasospasm / β-blocker C/I. |
| ACE inhibitors/ARBs | Ramipril, Losartan | ↓Afterload, ↓Remodeling, Cardioprotective | Hold pre-op (↓BP risk). Restart post-op. |
Anesthetic Techniques - Sleepy Safeguards
Key anesthetic choices significantly impact myocardial protection. Strategies aim to balance myocardial oxygen supply and demand.
| Technique | Protective Mechanism | Clinical Implications |
|---|---|---|
| Volatiles (Iso, Sevo) | Mimic IPC & postconditioning; $\downarrow Ca^{2+}$ overload, $K_{ATP}$ channels, anti-inflammatory | $\downarrow$Infarct size, $\downarrow$arrhythmias, improved LV function |
| TIVA (Propofol) | Antioxidant ($\downarrow ROS$), $\downarrow Ca^{2+}$ overload, anti-inflammatory, $\downarrow$endothelial dysfunction | Neuroprotection, potential cardioprotection |
| Thoracic Epidural (TEA) | Regional sympathetic blockade ($\downarrow HR$, $\downarrow$contractility), $\uparrow$coronary flow, $\downarrow$inflammation | $\downarrow MVO_2$, $\uparrow$supply, analgesia, $\downarrow$arrhythmias |
Hemodynamic Goals:
- Maintain Mean Arterial Pressure (MAP) >65 mmHg.
- Avoid tachycardia (e.g., Heart Rate (HR) <80 bpm).
- Prevent severe hypotension or hypertension.
Advanced Interventions - Critical Care Shields
- Cardioplegia: Induces cardiac arrest for surgical field.
- Types: Blood (↑O₂ carrying, better buffering) vs. Crystalloid (simple).
- Temperature: Cold (4-10°C, ↓metabolism) vs. Warm (↓reperfusion injury).
- Delivery: Antegrade (coronary ostia) or Retrograde (coronary sinus).

- Intra-Aortic Balloon Pump (IABP): Counterpulsation device.
- Mechanism: ↑Diastolic coronary perfusion, ↓Systolic afterload.
- Flowchart for Indications:
- Ventricular Assist Devices (VADs): Mechanical pumps for severe heart failure.
- Temperature Management: Normothermia or mild hypothermia (32-35°C) during CPB.
- Glycemic Control: Maintain blood glucose <180 mg/dL.
⭐ Antegrade cardioplegia is delivered via the coronary ostia, while retrograde cardioplegia is administered through the coronary sinus, often used adjunctively for more uniform myocardial cooling and protection.
High‑Yield Points - ⚡ Biggest Takeaways
- Cardioplegia, typically hyperkalemic, induces diastolic arrest, crucial for reducing MVO2.
- Therapeutic hypothermia (systemic/topical) is a cornerstone, significantly ↓ myocardial oxygen consumption.
- Volatile anesthetics (e.g., Isoflurane, Sevoflurane) provide pharmacological preconditioning, mimicking ischemic preconditioning.
- Controlled reperfusion (warm/cold, substrate-enriched) is vital to mitigate reperfusion injury.
- Key goals: Preserve ATP, limit intracellular Ca2+ overload, reduce oxidative stress.
- Adjuncts include beta-blockers, magnesium, and adenosine for enhanced protection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

