MRI/CT Environment & Risks - Remote Control Anesthesia
- MRI Suite Hazards:
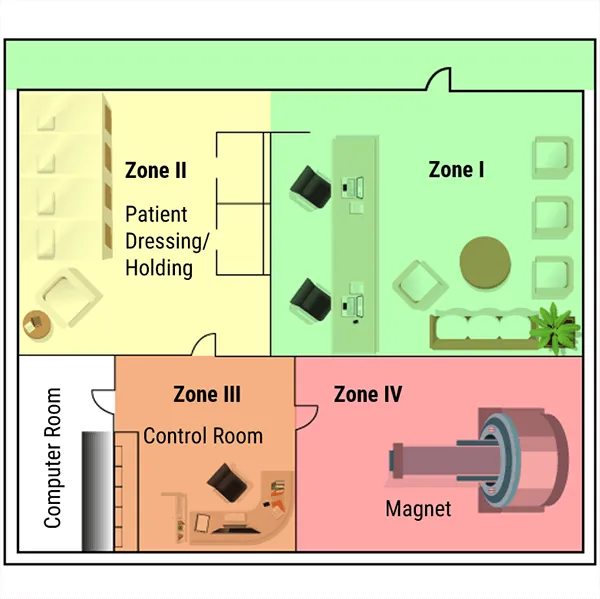
- 📌 MRI Zones (I-IV):
- Zone I: Public.
- Zone II: Unscreened pts.
- Zone III: Screened personnel/patients; restricted access.
- Zone IV: Scanner room; >5 Gauss line; highest risk.
- Projectile Risk: Ferromagnetic objects become dangerous projectiles.
- RF Heating: Tissue burn risk (implants, ECG leads).
- Acoustic Noise: 90-130 dB; hearing protection essential.
- Quench: Helium escape; asphyxia, frostbite risk.
⭐ The main static magnetic field in clinical MRI scanners typically ranges from 1.5T to 3T.
- 📌 MRI Zones (I-IV):
- CT Suite Hazards:
- Ionizing Radiation: ALARA principle.
- Contrast Media: Allergy/CIN risk.
- Patient Access: Limited.
- Remote Anesthesia:
- MRI-compatible equipment (anesthesia machine, monitors) essential.
- Long breathing circuits; vigilant remote monitoring crucial.
Patient Screening & Prep - Shield & Screen Carefully
MRI Safety:
- Screening: Implants (clips, coils), pacemakers/ICDs (verify MRI-conditional status), ferromagnetic foreign bodies (ocular, shrapnel), pregnancy.
- 📌 Mnemonic: NO METAL - Metallic implants, Electronic devices, Tattoos (old, metallic ink), Aneurysm clips, Loose foreign bodies.
CT Specifics:
- Contrast:
- Allergy Hx: Premedicate if prior mild reaction.
- Renal: Check eGFR. Gadolinium: avoid if eGFR < 30 mL/min/1.73m². Iodinated: Contrast-Induced Nephropathy (CIN) risk.
- Metformin: Hold if eGFR < 30 mL/min/1.73m², AKI, or iodinated contrast given with eGFR < 45 mL/min/1.73m².
Universal Prep:
- ASA Fasting Guidelines adhered to.
- Informed Consent obtained.

⭐ Absolute contraindications for MRI include most cardiac pacemakers (unless MRI-conditional and programmed appropriately), cochlear implants, and intraocular metallic foreign bodies.
Anesthetic Techniques & Drugs - Tunnel Vision Techniques
- Anesthesia Spectrum:
- General Anesthesia (GA): For complete immobility, controlled ventilation.
- Sedation: Deep (unresponsive, purposeful response to pain) vs. Conscious (responds to verbal commands).
- Key Agents & Delivery:
- Propofol: TIVA/TCI (Targets: Sedation 1.5-4.5 mcg/mL; GA 3-6 mcg/mL).
- Dexmedetomidine: Sedation with minimal respiratory depression.
- Remifentanil: Ultra-short-acting opioid, adjunct.
- Volatiles: Sevoflurane/Desflurane (low flow, efficient scavenging essential).
- Airway Management:
- LMA: MRI-compatible (non-ferromagnetic materials).

- ETT: For definitive airway control, especially if aspiration risk.
- LMA: MRI-compatible (non-ferromagnetic materials).
- Equipment Considerations:
- MRI Suite: MRI-compatible anesthesia machine, ventilator, and monitors.
- CT Suite: Standard machine; long breathing circuits may be needed.
⭐ Total Intravenous Anesthesia (TIVA) with propofol and remifentanil is often preferred for MRI to avoid interference from volatile agents and ensure rapid recovery.
NORA Monitoring & Crisis - Eyes, Ears, Emergencies
Monitoring Essentials:
- MRI Suite:
- ECG: Special filtered leads/algorithms.
- SpO2: Fiber-optic probes.
- NIBP: Extended tubing, automated.
- EtCO2: Long sampling lines, sidestream.
- Temperature: Fiber-optic/non-metallic probes.
- CT Suite:
- Standard ASA monitors; often requires remote patient observation.
Key Complications & Management:
- MRI-Specific Hazards:
- Thermal Burns: From looped wires or direct cable-skin contact. 📌 NO LOOPS (Avoid looping wires).
- Acoustic Damage: Noise >90-120 dB (use ear protection).
- Projectile Effect: Ferromagnetic objects become missiles.
- Quench: Cryogen release → asphyxia, frostbite, barotrauma.
- Claustrophobia.
⭐ To prevent RF-induced burns in MRI, ensure no direct skin contact with cables, avoid cable loops, and use appropriate padding.
- CT-Specific Hazards:
- Contrast Media Reactions: Allergic to anaphylactic.
- Radiation Exposure: Patient and staff.
- General NORA Risks:
- Hypoxia, hypotension, airway obstruction, emergence delirium/agitation.
Flowchart: Managing Acute Contrast Reaction
High‑Yield Points - ⚡ Biggest Takeaways
- MRI environment: Potent magnetic fields, RF energy, and loud noise (>100 dB) are major hazards.
- Strictly no ferromagnetic items; ensure all equipment is MRI-compatible.
- Patient monitoring is challenging due to limited access and RF interference.
- Gadolinium contrast may cause Nephrogenic Systemic Fibrosis (NSF) in renal impairment.
- CT anesthesia aims for immobility, with attention to radiation safety for all.
- Total Intravenous Anesthesia (TIVA) is often favored for MRI; hearing protection is vital.
- Emergency preparedness for events like quenching is crucial.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

