Pre-Anesthetic Evaluation - Patient Check-in
- Patient ID & Valid Consent: Verify patient, procedure. Crucial first step.
- Focused History (AMPLE):
- Allergies.
- Medications: Note anticoagulants, antiplatelets, hypoglycemics.
- PMH: Cardiac, respiratory, OSA, GERD, prior anesthesia issues.
- Last Meal: Confirm NPO.
- Events leading to procedure.
- Airway Assessment:
- Mallampati, TMD (> 6 cm), neck mobility, dentition, beard.
- Fasting Guidelines (NPO): 📌 "2-6-8 Rule"
- Clear liquids: ≥ 2 hrs.
- Light meal/milk: ≥ 6 hrs.
- Heavy/fatty meal: ≥ 8 hrs.
⭐ Strict NPO adherence is vital to minimize aspiration risk in GI endoscopy.
- ASA Physical Status: Assign (I-VI).
- Baseline Vitals & IV Access: Record HR, BP, SpO2. Secure IV line appropriate for procedure and patient condition.
Sedation & Monitoring - The Anesthesia Dashboard
- Goals: Patient comfort, amnesia, stable cardiorespiratory function, rapid recovery. Target: moderate to deep sedation.
- ASA Standard Monitoring:
- Oxygenation: Pulse oximetry (SpO₂ > 92%). Supplemental O₂.
- Ventilation: Capnography (ETCO₂) - vital for early detection of hypoventilation/apnea.
- Circulation: Continuous ECG, NIBP (q3-5 min), Heart Rate.
- Depth of Sedation: Clinical scales (e.g., MOAAS/OAA/S).
- Key Vigilance: Shared airway, aspiration risk, intervention readiness.
⭐ Capnography is the cornerstone for detecting respiratory depression during GI endoscopy sedation, often preceding changes in SpO₂.
Pharmacological Agents - The Sedation Cocktail
- Goal: Conscious to deep sedation.
- Common Agents:
- Benzodiazepines (BZD):
- Midazolam: 0.02-0.1 mg/kg IV. Anxiolysis, amnesia. Onset 1-3 min.
- Reversal: Flumazenil (0.2 mg IV, up to 1 mg). 📌 Flumazenil Frees Benzos.
- Opioids:
- Fentanyl: 0.5-1 mcg/kg IV. Analgesia, sedation. Onset 1-2 min.
- Reversal: Naloxone (0.04-0.4 mg IV). 📌 Naloxone Nixes Narcotics.
- Propofol:
- 0.5-1 mg/kg IV bolus; inf. 25-75 mcg/kg/min. Rapid onset/recovery, antiemetic.
- Risk: Apnea, hypotension. No specific reversal agent.
- Ketamine:
- 0.25-0.5 mg/kg IV. Dissociative sedation, analgesia, airway preserved.
- Risk: Emergence phenomena, ↑secretions.
- Dexmedetomidine:
- 0.2-0.7 mcg/kg/hr IV. Sedation, minimal respiratory depression.
- Risk: Bradycardia, hypotension.
- Benzodiazepines (BZD):
- Combinations (Synergistic Effects):
- BZD + Opioid (e.g., Midazolam + Fentanyl).
- Propofol ± Opioid/BZD.
⭐ Propofol is favored for its rapid recovery profile, making it ideal for high-turnover endoscopy units, but requires careful cardiorespiratory monitoring due to potential for apnea and hypotension.
Procedural Nuances & Complications - Gut Feelings Gone Wrong
- General Risks: Hypoxemia, hypotension, aspiration (esp. upper GI), arrhythmias.
- Procedure-Specifics:
- EGD: Shared airway, ↑aspiration risk. Brief.
- Colonoscopy: Longer, CO2 insufflation preferred (↓distension/pain). Vasovagal common.
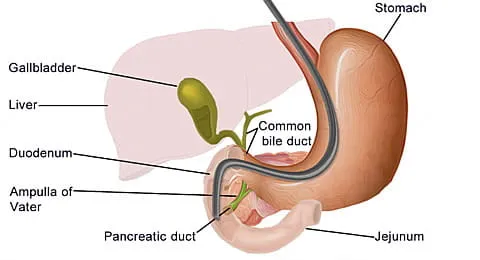
- ERCP/EUS: Prone/left lateral. Prolonged, requires deep sedation/TIVA.
- Risks: Pancreatitis, cholangitis, bleeding, duodenal perforation.
- Sphincter of Oddi relaxation: Glucagon, hyoscine.
- Complications Management:
- Airway: Jaw thrust, O2, LMA/ETT.
- Hemodynamic: Fluids, vasopressors.
- Reversal: Naloxone, Flumazenil.
- Perforation: Surgical consult, antibiotics.
- 📌 PERCS for ERCP Complications: Pancreatitis, Excessive bleeding, Rupture (perforation), Cholangitis, Sepsis.
⭐ Post-ERCP pancreatitis (PEP) is the most common serious complication, incidence 3-5%; up to 15% in high-risk patients.
High‑Yield Points - ⚡ Biggest Takeaways
- Airway management is critical; high aspiration risk with shared airway.
- Monitored Anesthesia Care (MAC) with propofol is standard; General Anesthesia (GA) for complex or prolonged procedures.
- Propofol: rapid onset/offset, antiemetic; risk of apnea, hypotension. Consider etomidate/ketamine in unstable patients.
- Ketamine useful adjunct: preserves airway reflexes, provides analgesia, bronchodilation.
- Monitor for hypoxia, hypercapnia (capnography essential), hypotension, and arrhythmias.
- Difficult airway (e.g., obesity, OSA) and full stomach are major concerns requiring careful planning.
- Barotrauma (perforation) is a rare but serious procedural complication to be aware of during endoscopy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

