Thoracic Trauma Overview - Chest Case Chaos
Thoracic trauma is a major cause of mortality, often requiring immediate life-saving interventions. Rapid assessment using the ATLS® ABCDE protocol is paramount to identify and manage critical injuries, focusing on the "lethal six".
- Key Life Threats & Initial Management:
- Tension Pneumothorax: Needle decompression (e.g., 14-16G needle, 2nd ICS MCL), then chest tube (5th ICS MAL).
- Open Pneumothorax ("sucking chest wound"): Three-sided occlusive dressing, then chest tube.
- Massive Hemothorax: >1500 mL initial loss or >200 mL/hr for 2-4 hrs; chest tube, urgent thoracotomy.
- Flail Chest: Paradoxical chest wall motion; aggressive pain control, O2, consider PPV.
- Cardiac Tamponade: Beck's triad (hypotension, JVD, muffled heart sounds); pericardiocentesis or thoracotomy.
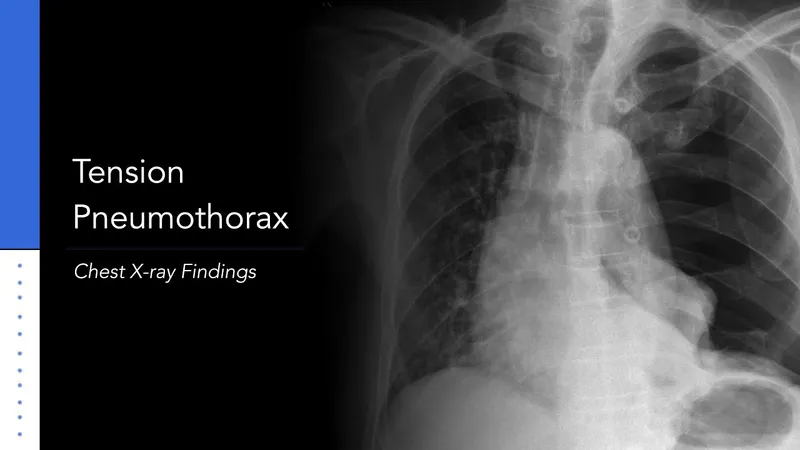
⭐ In tension pneumothorax, clinical diagnosis trumps radiological confirmation for immediate needle decompression.
Airway & Ventilation Strategies - Breathless Battles
- Rapid Sequence Intubation (RSI): Standard for full stomach; apply cricoid pressure (Sellick's).
- Difficult Airway: Anticipate (trauma, tumors). Backup: supraglottic airway (SGA), videolaryngoscope, cricothyroidotomy.
- Lung Isolation: Essential for unilateral pathology (e.g., massive hemoptysis, empyema, giant bullae).
- Double Lumen Tube (DLT): Preferred for adults; common sizes 35-41F.
- Bronchial Blockers (BB): Alternative with existing ETT, difficult airway, or pediatric cases.
- One-Lung Ventilation (OLV):
- Challenges: Hypoxemia (↑shunt), hypercapnia, ↓venous return.
- Manage with: ↑FiO2 to 1.0, PEEP to dependent lung, CPAP to non-dependent lung, recruitment maneuvers.
- Lung Protective Ventilation (LPV): $V_T$ 4-6 mL/kg predicted body weight, $P_{plat}$ < 30 cmH₂O.

⭐ Fiberoptic bronchoscopy (FOB) is gold standard for confirming DLT position and troubleshooting during thoracic surgery requiring lung isolation.
Key Thoracic Crises - Thoracic Terrors
- Massive Hemoptysis: >100-600 mL/24h.
- Airway: Rigid bronchoscope, Double-Lumen Tube (DLT), or Bronchial Blocker (BB).
- 📌 Position: Bleeding lung Down.
- Ventilation: Spontaneous if possible; avoid coughing.
- Tracheobronchial Injury (TBI): High mortality. Suspect: trauma, subcut. emphysema.
- Airway: Awake Fiberoptic Intubation (AFOI) preferred. Endotracheal Tube (ETT) distal to injury.
- Ventilation: Spontaneous preferred; gentle, low pressures. Avoid initial muscle relaxants.
- Esophageal Perforation: High sepsis risk.
- Airway: Rapid Sequence Intubation (RSI) (aspiration risk).
- Management: Fluids, antibiotics. DLT for repair.
- Tension Pneumothorax: Clinical Dx (hypotension, JVD, ↓breath sounds, tracheal shift).
- Immediate needle decompression (2nd ICS MCL / 5th ICS AAL), then chest tube.
- Anesthesia: 100% O2. Avoid N2O. Positive Pressure Ventilation (PPV) worsens pre-decompression.
- Cardiac Tamponade: Beck's triad (hypotension, JVD, muffled heart sounds).
- Anesthesia: Maintain preload, contractility, HR. Ketamine good. Avoid vasodilators/myocardial depressants. PPV cautiously.
⭐ In massive hemoptysis, the primary immediate goal is to protect the contralateral (healthy) lung from aspiration of blood by appropriate patient positioning and definitive airway management (e.g., DLT).
Perioperative Management - Recovery Roadmap
- Intraoperative Focus:
- Monitoring: Standard ASA, arterial line, CVP. TEE/PA catheter for high-risk patients.
- One-Lung Ventilation (OLV): Maintain SaO2 > 90%. Use FiO2 1.0 initially, PEEP 5-10 cmH2O to dependent lung. Consider permissive hypercapnia.
- Fluid Therapy: Restrictive, goal-directed (e.g., crystalloids < 3 ml/kg/hr). Avoid overload to prevent pulmonary edema.
- Postoperative Pathway:
- Pain Control (Multimodal is key):
- Thoracic Epidural Analgesia (TEA) or Paravertebral Block (PVB) - cornerstone.
- NSAIDs, paracetamol, opioids (e.g., PCA).
- Respiratory Care:
- Extubation Criteria: Awake, alert, PaO2 > 60 mmHg on FiO2 ≤ 0.4-0.5, adequate tidal volume, RR < 30/min.
- Aggressive chest physiotherapy, incentive spirometry, early mobilization to prevent atelectasis.
- Complication Management: Vigilance for atelectasis, pneumonia, persistent air leaks, arrhythmias (especially Atrial Fibrillation), DVT.
- Pain Control (Multimodal is key):
⭐ Epidural analgesia (local anesthetic + opioid) significantly improves postoperative respiratory function and reduces pulmonary complications after thoracotomy operations for thoracic emergencies like empyema or lung abscess drainage.
High‑Yield Points - ⚡ Biggest Takeaways
- Double-lumen tubes (DLT) or bronchial blockers are essential for one-lung ventilation (OLV).
- Preserve hypoxic pulmonary vasoconstriction (HPV); high-dose volatile anesthetics can blunt this reflex.
- Rapid Sequence Intubation (RSI) is crucial in patients with a full stomach or trauma.
- Tension pneumothorax requires immediate needle decompression, followed by chest tube insertion.
- In massive hemoptysis, the priority is protecting the contralateral lung, often using a DLT.
- Traumatic airway injury may necessitate awake fiberoptic intubation or a surgical airway.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

