PONV: Risk Factors & Scores - The Queasy Question
Postoperative Nausea & Vomiting (PONV): Distressing, common in outpatients (~30-50%). Impacts: delayed discharge, dissatisfaction, ↑ costs, unplanned admission.
- Key Risk Factors (Apfel Score):
- Female gender
- Non-smoker
- History of PONV / Motion Sickness
- Postoperative opioids
- 📌 Mnemonic: FANS (Female, Anesthesia [opioids], Non-smoker, Sickness Hx)
- Apfel Score & PONV Risk: (Score = sum of positive factors)
- 0 factors: Low risk (~10%)
- 1 factor: Low risk (~20%)
- 2 factors: Moderate risk (~40%)
- 3 factors: High risk (~60%)
- 4 factors: High risk (~80%)
- Simplified scores also exist for rapid assessment.
⭐ Apfel score is the most widely validated tool for predicting PONV risk.
PONV: Pharmacological Prophylaxis - Pill Power Plays
Pharmacological prophylaxis is crucial. Key agents include:
- 5-HT3 Antagonists: Ondansetron (4mg IV/PO, pre-op/end). Block 5-HT3 receptors (periphery/CTZ). Broad efficacy.
- NK-1 Antagonists: Aprepitant (40mg PO, 1-3h pre-op). Block Substance P at NK-1 receptors (brainstem). High-risk, long duration.
- Corticosteroids: Dexamethasone (4-8mg IV, post-induction). Anti-inflammatory, prostaglandin inhibition. Reduces pain.
- Dopamine Antagonists: Metoclopramide (10mg IV, end). D2 receptor blockade (CTZ). Prokinetic; less effective alone. (Avoid Droperidol: QTc risk).
- Antihistamines (H1): Dimenhydrinate (25-50mg PO/IV). H1 blockade (vestibular, CTZ). For motion sickness hx; sedation.
- Anticholinergics: Scopolamine patch (1.5mg TD, pre-op). Muscarinic blockade (vestibular). Motion sickness; dry mouth.
📌 Mnemonic (Classes): Serotonin antags, NK-1 antags, Dexamethasone (Corticosteroids), Antihistamines, Anticholinergics, Dopamine antags (S.N.D.A.A.D - 'Send Dad').
⭐ Combining antiemetics from different classes is more effective than single-agent prophylaxis for high-risk patients.
PONV: Non-Pharmacological Methods - Gentle Guards
- Regional Anesthesia: Utilise whenever feasible; significantly ↓ PONV risk compared to general anesthesia.
- Hydration: Ensure adequate intravenous fluid administration perioperatively.
- Anesthetic Choice:
- Avoid Nitrous Oxide ($N_2O$) if possible.
- Consider TIVA or minimize volatile anesthetics.
- Acupressure/Acupuncture:
- Stimulate P6 (Neiguan) point on the wrist.
- 📌 P6 - 'Pressure 6 stops sick'.
- Supplemental Oxygen: Administer routinely in PACU.
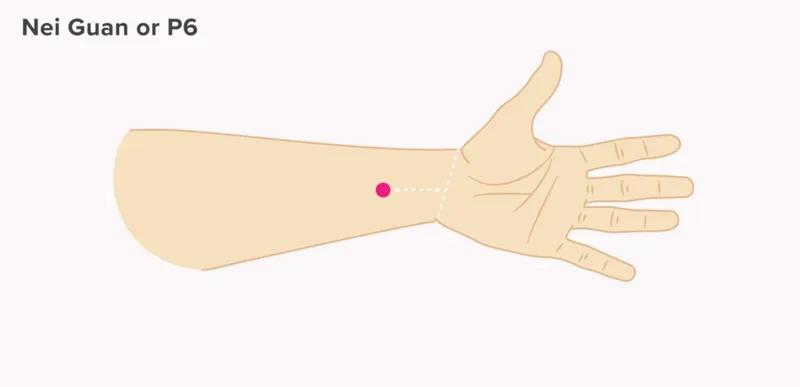
⭐ Acupressure at the P6 (Neiguan) point is a recognized non-pharmacological method for PONV prevention, often comparable to antiemetics for mild to moderate risk_._
PONV: Multimodal & Rescue - Team Tactics Triumph
- Multimodal Prophylaxis: Key for moderate/high PONV risk (≥2 risk factors). Combine ≥2 antiemetics from different classes.
- Risk-Stratified Prophylaxis (Apfel Score):
- Rescue Therapy: If PONV occurs.
- Use agent from a different class than prophylactic drugs.
- Options: Ondansetron 4 mg IV, Promethazine 6.25-12.5 mg IV, Dexamethasone 2-4 mg IV (if not used).
⭐ For rescue treatment, an antiemetic from a different pharmacological class than that used for prophylaxis should be administered.
High-Yield Points - ⚡ Biggest Takeaways
- Risk stratification using tools like the Apfel score is paramount.
- A multimodal approach is superior to single-agent therapy for PONV prevention.
- Administer prophylaxis if ≥2 Apfel risk factors are present.
- Key drugs: Ondansetron (5-HT3 antagonist), Dexamethasone; add Aprepitant (NK-1 antagonist) for high risk.
- Prefer regional anesthesia or TIVA (e.g., propofol) over volatile anesthetics.
- Avoid nitrous oxide and minimize postoperative opioids.
- Ensure adequate hydration and analgesia to reduce baseline nausea triggers_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

