Male Reproductive Functional Anatomy - Testes & Tubes
- Testes: Paired; sperm (spermatogenesis) & testosterone production.
- Seminiferous Tubules: Sperm production. Contain Sertoli cells.
- Sertoli Cells: Support spermatogenesis; blood-testis barrier; secrete inhibin, ABP.
⭐ Sertoli cells form the blood-testis barrier, protecting sperm from immune attack.
- Leydig Cells: Interstitial; testosterone production (LH-driven).
- Duct System:
- Epididymis: Sperm maturation (motility), storage.
- Vas Deferens: Transports sperm to ejaculatory duct.
- Ejaculatory Duct: Vas deferens + seminal vesicle duct; via prostate.
- Accessory Glands: Contribute to semen.
- Seminal Vesicles: Alkaline, fructose fluid (~65-75% vol).
- Prostate Gland: Milky fluid, enzymes (PSA) (~25-30% vol).
- Bulbourethral Glands: Pre-ejaculate; neutralizes urethral acid.


- Sperm Pathway: 📌 SEVEN UP
*(S: Seminiferous tubules, E: Epididymis, V: Vas deferens, E: Ejaculatory duct, N: Nothing, U: Urethra, P: Penis)*
Female Reproductive Functional Anatomy - Ovaries & Uterus
- Ovaries: Paired gonads.
- Folliculogenesis: Primordial follicle → Graafian follicle. Ovulation (LH surge).
- Corpus Luteum: Secretes progesterone & estrogen; regresses to corpus albicans if no fertilization.
- Fallopian Tubes (Uterine Tubes):
- Parts: Infundibulum (fimbriae), Ampulla, Isthmus, Intramural part.
- Function: Oocyte transport via ciliary action & peristalsis.
⭐ Fertilization typically occurs in the ampulla.
- Uterus:
- Layers: Perimetrium (outer serosa), Myometrium (smooth muscle, contractions), Endometrium (inner lining; stratum basalis & functionalis).
- Cyclical Changes (Endometrium):
- Menstrual (Days 1-5): Stratum functionalis shed.
- Proliferative (Days 6-14): Estrogen-driven regrowth of functionalis.
- Secretory (Days 15-28): Progesterone-driven; glandular, vascular, ready for implantation.

- Cervix: Lower, narrow part of uterus; cyclical mucus changes.
- Vagina: Fibromuscular tube; birth canal; acidic pH (Döderlein's bacilli).
- Support & Vasculature (Functional Relevance):
- Ligaments: Broad lig. (drape), Round lig. (maintains anteversion), Cardinal lig. (main support), Ovarian lig. (ovary to uterus), Suspensory lig. (contains ovarian vessels).
- Blood Supply: Ovarian artery (from abdominal aorta), Uterine artery (from internal iliac artery).
Gametogenesis Functional Aspects - Making Babies 101
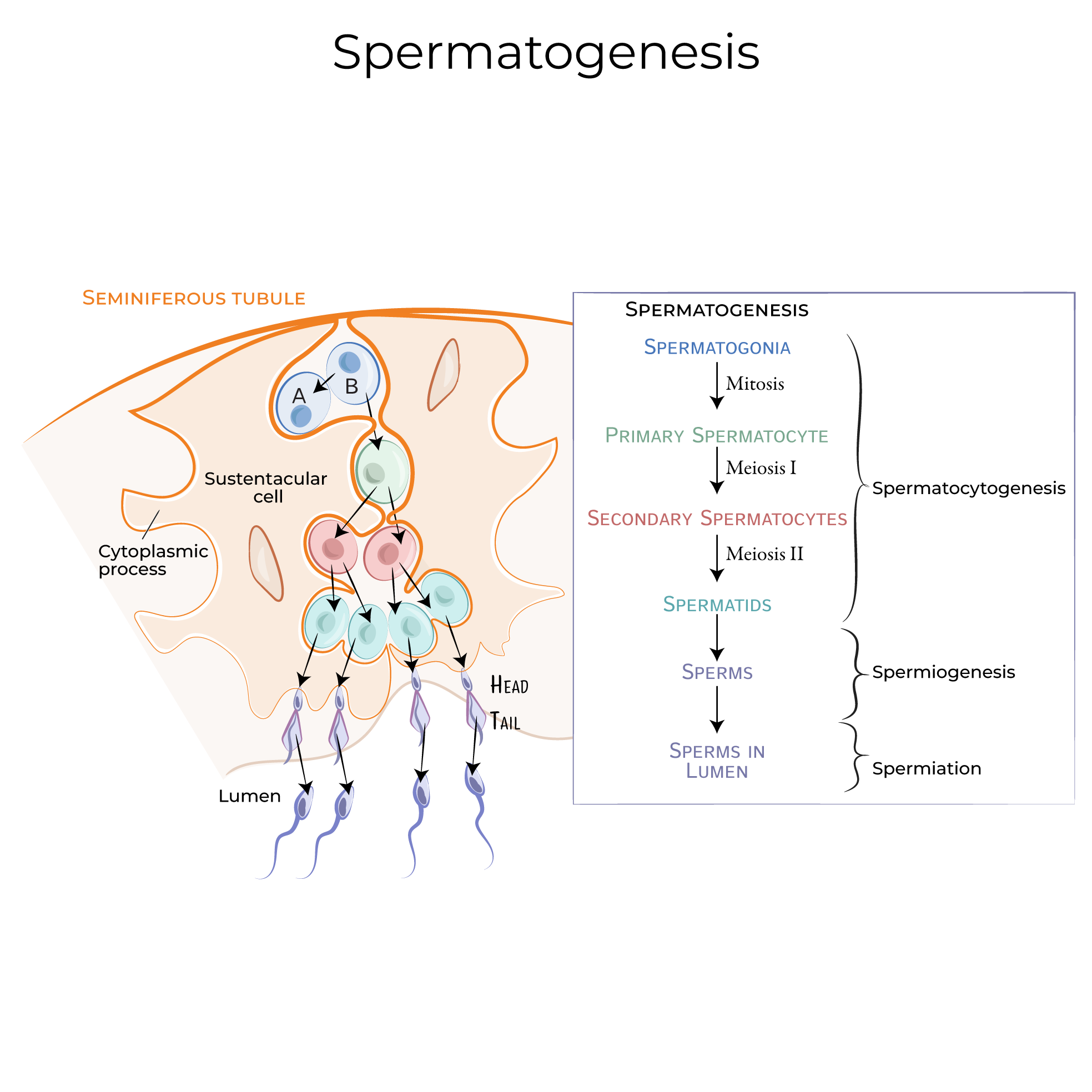
Spermatogenesis:
- Site: Seminiferous tubules. Continuous from puberty. Duration: ~74 days.
- Stages: Spermatogonia (2n) → Primary spermatocyte (2n) → Secondary spermatocyte (n) → Spermatid (n) → Spermatozoa (n).
- Spermiogenesis: Spermatid maturation (acrosome, flagellum). Yields 4 sperm.
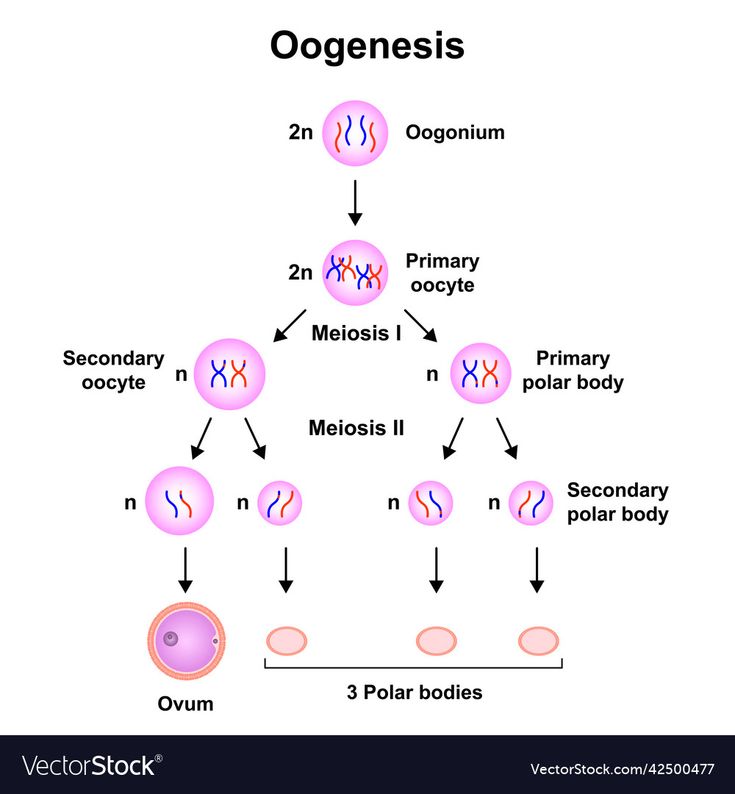
Oogenesis:
- Site: Ovary. Discontinuous; starts prenatally, resumes at puberty.
- Stages: Oogonium (2n) → Primary oocyte (2n) → Secondary oocyte (n) + 1st polar body. Yields 1 ovum.
⭐ Key Arrests: Primary oocytes in Prophase I (birth to puberty); Secondary oocytes in Metaphase II (ovulation to fertilization).
Mature Gametes:
- Sperm: Head (acrosome, nucleus n=23), Midpiece (mitochondria), Tail.
- Ovum: Zona pellucida, Corona radiata, nucleus (n=23).

Reproductive Hormonal Control - Reproductive Orchestra
HPG Axis: Hypothalamus (GnRH) → Pituitary (LH/FSH) → Gonads (Steroids, Inhibin).
-
Key Hormones & Roles:
- GnRH (Hypothalamus): Stimulates LH/FSH release.
- LH (Ant. Pituitary): M: Testosterone (Leydig). F: Ovulation trigger, corpus luteum.
- FSH (Ant. Pituitary): M: Spermatogenesis (Sertoli), Inhibin. F: Follicular growth, Estrogen (Granulosa).
- Testosterone (Leydig): Male characteristics, spermatogenesis.
- Estrogen (Ovarian follicles/Corpus Luteum): Female characteristics, endometrial proliferation.
- Progesterone (Corpus Luteum/Placenta): Maintains pregnancy, endometrial secretory phase.
- Inhibin (Sertoli/Granulosa): ↓FSH. Activin (Sertoli/Granulosa): ↑FSH.
-
Menstrual Cycle: Coordinated E, P, LH, FSH changes regulate follicular, ovulatory, luteal phases.
⭐ LH Surge: A rapid ↑ in LH, triggered by sustained high estrogen (positive feedback), is crucial for ovulation.

High‑Yield Points - ⚡ Biggest Takeaways
- Spermatogenesis occurs in seminiferous tubules; sperm matures in the epididymis.
- Leydig cells synthesize testosterone; Sertoli cells support spermatogenesis.
- Oogenesis: primary oocytes arrest in prophase I; secondary oocytes in metaphase II.
- Fertilization most commonly occurs in the ampulla of the uterine tube.
- Corpus luteum produces progesterone, essential for maintaining early pregnancy.
- Endometrium: stratum functionalis sheds; stratum basalis regenerates the lining.
- Pampiniform plexus cools arterial blood to testes via countercurrent exchange_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

