Variations in Vascular Anatomy - Artery Antics
- Circle of Willis: Highly variable; key for cerebral collateral flow.
⭐ A complete Circle of Willis, ensuring robust collateral cerebral circulation, is present in only about 20-25% of individuals.
- Common: Hypoplastic/absent Anterior Communicating Artery (AComA), Posterior Communicating Artery (PComA).
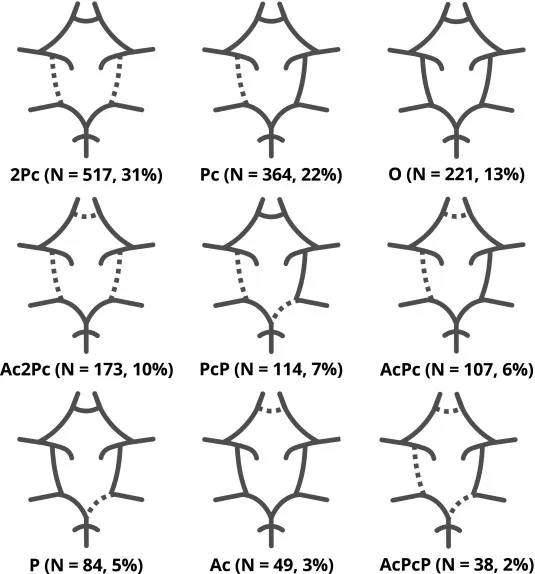
- Common: Hypoplastic/absent Anterior Communicating Artery (AComA), Posterior Communicating Artery (PComA).
- Coronary Arteries:
- Dominance patterns: Right (~60-70%), Left (~10-15%), Co-dominant (~15-20%).
- Variable origins: Conus artery, SA nodal artery, AV nodal artery.
- Renal Arteries: Accessory arteries common (~30%); polar arteries, early branching.
- Hepatic Arteries (Michels Classification):
- Common variations: Replaced Right Hepatic Artery (RHA) from Superior Mesenteric Artery (SMA) (Type III); Replaced Left Hepatic Artery (LHA) from Left Gastric Artery (LGA) (Type II).
- 📌 Michels: Remember common alternative origins (SMA for RHA, LGA for LHA).
- Celiac Trunk:
- Variations: Hepatosplenic trunk, celiacomesenteric trunk (common origin with SMA).
- Subclavian Artery:
- Arteria Lusoria: Aberrant right subclavian artery (retroesophageal course, may cause dysphagia).
Variations in Vascular Anatomy - Vein Ventures
- Superior Vena Cava (SVC) Anomalies:
- Persistent Left SVC (PLSVC): Most common. Usually drains to coronary sinus.
- 📌 Mnemonic: "Left SVC stays, to CS it strays."
- 📌 Mnemonic: "Left SVC stays, to CS it strays."
- Persistent Left SVC (PLSVC): Most common. Usually drains to coronary sinus.
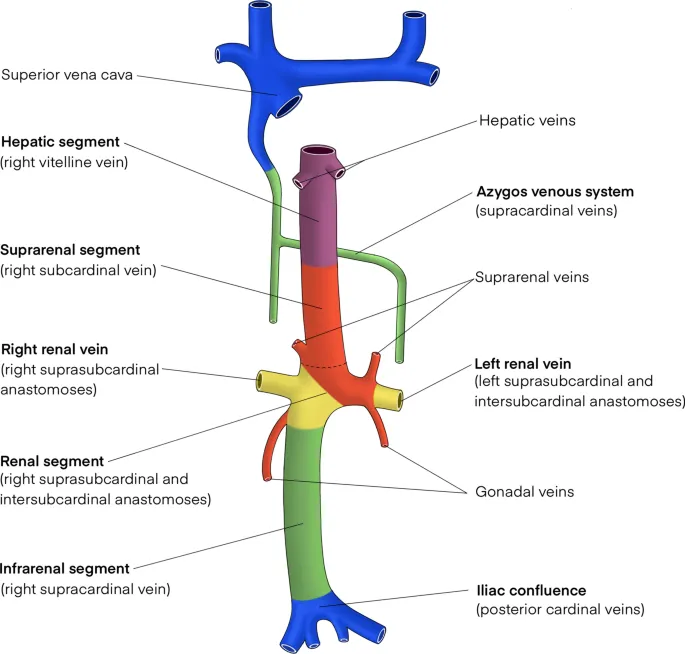
- Inferior Vena Cava (IVC) Anomalies:
- Double IVC: Persistence of both supracardinal veins.
- Left IVC: Regression of right supracardinal vein.
- Azygos/Hemiazygos continuation: Infrahepatic IVC interruption; shunts via azygos.
- Retroaortic left renal vein: Posterior to aorta; compression risk.
- Portal Vein Variations:
- Preduodenal portal vein: Anterior to duodenum; surgical risk.
- Trifurcation, Duplications: Branching variations.
- Hepatic Vein Variations:
- Accessory inferior right hepatic vein: Drains to IVC; common.
- Dural Venous Sinus Variations:
- Hypoplasia/aplasia of transverse sinus: Often left; affects outflow.
⭐ A persistent left superior vena cava (PLSVC) is the most common systemic venous anomaly, typically draining into the coronary sinus, and its presence is crucial to identify during central venous catheterization or cardiac pacemaker implantation.
Variations in Vascular Anatomy - Surgical Surprises
- Surgical Implications: Awareness is critical.
- Unexpected variations: ↑ bleeding risk, altered surgical planes, risk of iatrogenic injury.
- Modified techniques often required in:
- Nephrectomy (e.g., multiple/aberrant renal arteries).
- Liver resection/transplant (e.g., variant hepatic arteries - see below ⭐).
- CABG (coronary artery anomalies).
- Pancreatic surgery (celiac trunk/SMA variations).
- Diagnostic Challenges:
- Potential for misinterpretation of angiograms, CT, or MRI scans.
- Anomalies can mimic pathological conditions, leading to diagnostic errors.
- Predisposition to Pathology:
- Aneurysms (e.g., Circle of Willis variations).
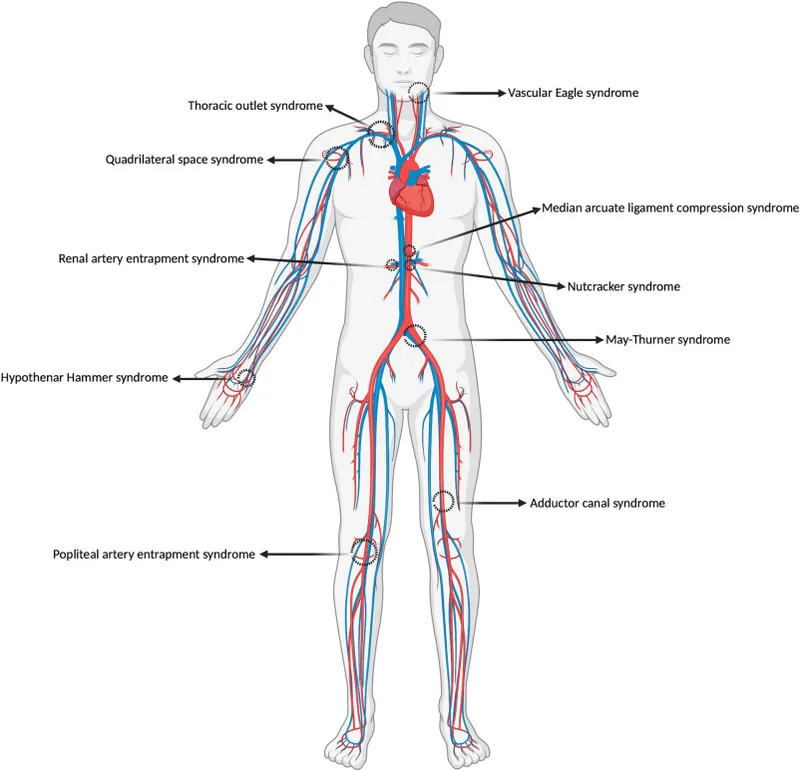
- Vascular Compression Syndromes:
- Nutcracker syndrome: Left Renal Vein (LRV) compression by SMA/Aorta.
- May-Thurner syndrome: Left Common Iliac Vein (LCIV) compression by RCIA.
- Arteria Lusoria (aberrant R. subclavian a.): Can cause dysphagia lusoria.
- Interventional Radiology Considerations:
- Crucial for pre-procedural mapping and guiding interventions.
- Key in managing complications from vascular anomalies.
⭐ An aberrant right hepatic artery originating from the SMA (Michels Type III) courses posterior to the portal vein and common bile duct; its inadvertent ligation during cholecystectomy or pancreaticoduodenectomy can lead to severe hepatic ischemia or biliary stricture.
High‑Yield Points - ⚡ Biggest Takeaways
- Coronary artery variations: Ramus intermedius and high take-off are notable.
- Aortic arch anomalies: Double aortic arch (vascular rings) and aberrant right subclavian artery (dysphagia lusoria) are key.
- Multiple renal arteries are common; accessory lower pole arteries can cause UPJ obstruction.
- Hepatic artery variations: Replaced RHA from SMA or LHA from left gastric are surgically vital.
- Circle of Willis: PCOM hypoplasia and fetal PCA origin are frequent findings.
- A persistent median artery can contribute to carpal tunnel syndrome.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

