UAS Fundamentals - Nerve Zapper Intro
- Upper Airway Stimulation (UAS): Implantable neurostimulation device for treating Obstructive Sleep Apnea (OSA).
- Indication: For moderate to severe OSA patients who are intolerant or non-adherent to CPAP therapy.
- Mechanism: Delivers mild electrical stimulation to the hypoglossal nerve (CN XII) during sleep.
- Stimulation is synchronized with the patient's breathing.
- Prevents airway collapse, especially at the tongue base.
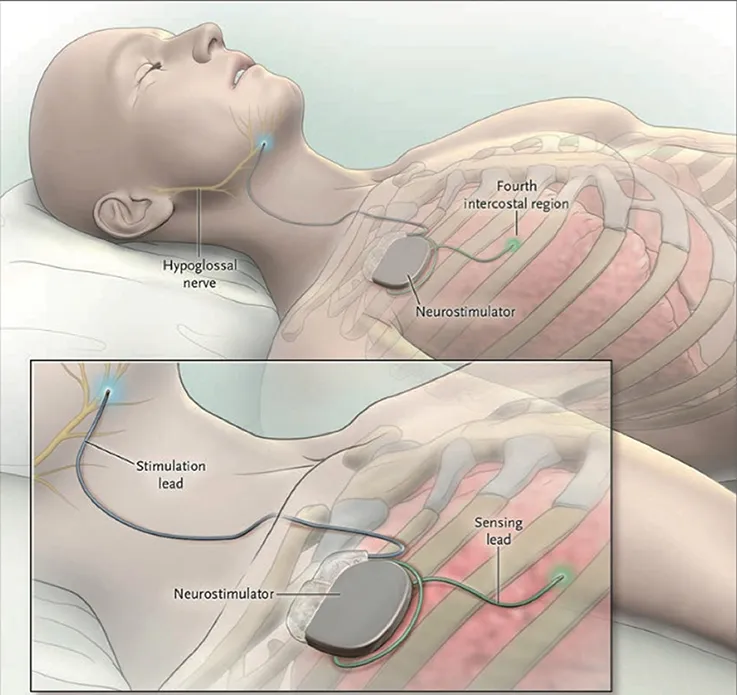
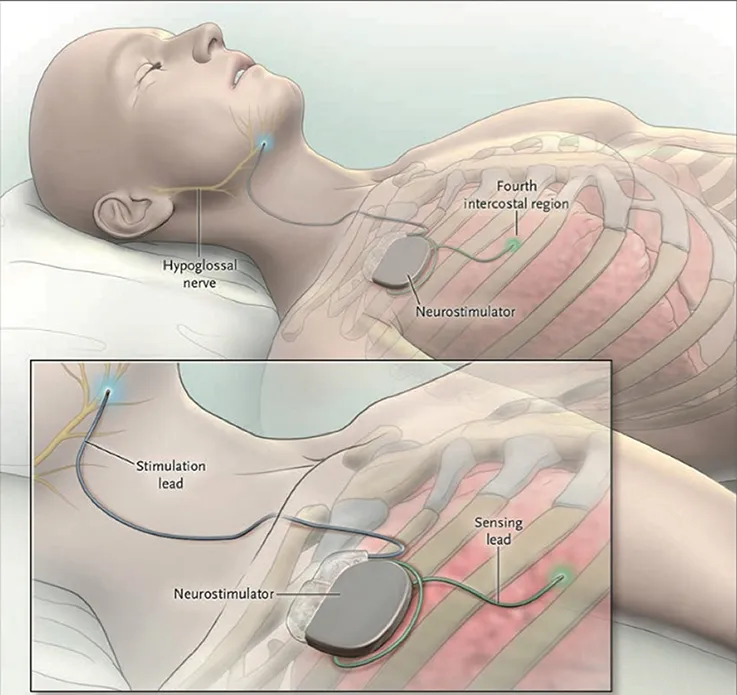
- Components:
- Implantable pulse generator (IPG) - usually placed in the chest.
- Sensing lead - detects respiratory effort.
- Stimulation lead - activates genioglossus muscle for tongue movement.
- Goal: Improve airway patency by stiffening and protruding the tongue.
⭐ UAS primarily targets the genioglossus muscle via hypoglossal nerve stimulation.
- "Nerve Zapper": Colloquial term describing its electrical action on the nerve.
Patient Selection - The "Who's Who"
Key to successful Upper Airway Stimulation (UAS) is meticulous patient selection.
- Inclusion Criteria:
- Age: ≥18 years
- Moderate to Severe OSA: AHI 15-65/hr, predominantly obstructive
- BMI: <32-35 kg/m² (device-specific, e.g., Inspire uses <32)
- CPAP failure or intolerance (documented)
- Patient motivation & realistic expectations
- Exclusion Criteria (Key):
- Anatomical:
- Complete Concentric Collapse (CCC) of soft palate on DISE
- Physiological:
- Significant central sleep apnea (>25% of events)
- Hypoventilation syndromes
- BMI > 32-35 kg/m²
- Certain neuromuscular diseases
- Anatomical:
⭐ Drug-Induced Sleep Endoscopy (DISE) is mandatory to exclude complete concentric collapse (CCC) at the velopharynx, a key contraindication.
The Device & Procedure - Implant Insights
- UAS System Components:
- Implantable Pulse Generator (IPG): Placed in a subcutaneous chest wall pocket.
- Stimulation Lead: Cuff electrode on hypoglossal nerve (HGN XII), specifically targeting branches innervating the genioglossus muscle (tongue protrusor).
- Respiratory Sensing Lead: Placed between intercostal muscles; detects respiratory effort to synchronize stimulation.
- Surgical Implantation:
- Procedure performed under general anesthesia.
- Typically involves two to three incisions: submandibular (for HGN lead), infraclavicular (for IPG), and lateral thoracic (for sensing lead).
- Intraoperative nerve integrity monitoring is essential.
- Activation & Titration:
- Device typically activated ~1 month post-operatively to allow for healing.
- Optimal stimulation settings are determined via a titration study in a sleep laboratory.
⭐ The UAS system consists of three main components: a stimulation electrode cuff on the hypoglossal nerve, a respiratory sensing lead, and an implantable pulse generator (IPG).
Outcomes & Hurdles - Zapping Success?
- Positive Outcomes:
- ↓ AHI (Apnea-Hypopnea Index).
- ↓ ODI (Oxygen Desaturation Index).
- ↓ ESS (Epworth Sleepiness Scale) scores.
- ↑ QoL (Quality of Life).
- Snoring reduction.
- Sustained long-term efficacy in responders.
- Defining Success:
⭐ Successful UAS therapy is often defined by a >50% reduction in AHI to <20/hr and significant improvement in ODI and subjective sleepiness (ESS).
- Potential Hurdles & Complications:
- Strict patient selection: BMI <32-35 kg/m², AHI 15-65/hr, specific collapse patterns (no CCC at velum).
- Surgical risks: Hypoglossal nerve (CN XII) injury (transient/rare), infection, pain.
- Device-related: Discomfort, lead issues (fracture/migration), battery depletion.
- Titration period post-implantation.
- Cost.
- Tongue stimulation awareness.
High‑Yield Points - ⚡ Biggest Takeaways
- UAS treats OSA via hypoglossal nerve (CN XII) stimulation, improving airway patency.
- Synchronous tongue protrusion with inspiration relieves retrolingual obstruction.
- For moderate-severe OSA (AHI 15-65), BMI <32-35 kg/m², with CPAP failure/intolerance.
- DISE is essential to exclude Complete Concentric Collapse (CCC) at the palate.
- Significantly reduces AHI and Oxygen Desaturation Index (ODI), improving sleep quality.
- Implantable system: pulse generator, sensing lead (intercostal), and CN XII stimulation cuff_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more