Pediatric Obstructive Sleep Apnea - POSA Basics & Scope
- Recurrent episodes of partial/complete upper airway obstruction during sleep.
- Disrupts normal breathing patterns & sleep architecture.
- Prevalence: Affects 1-5% of children; peak age 2-8 years.
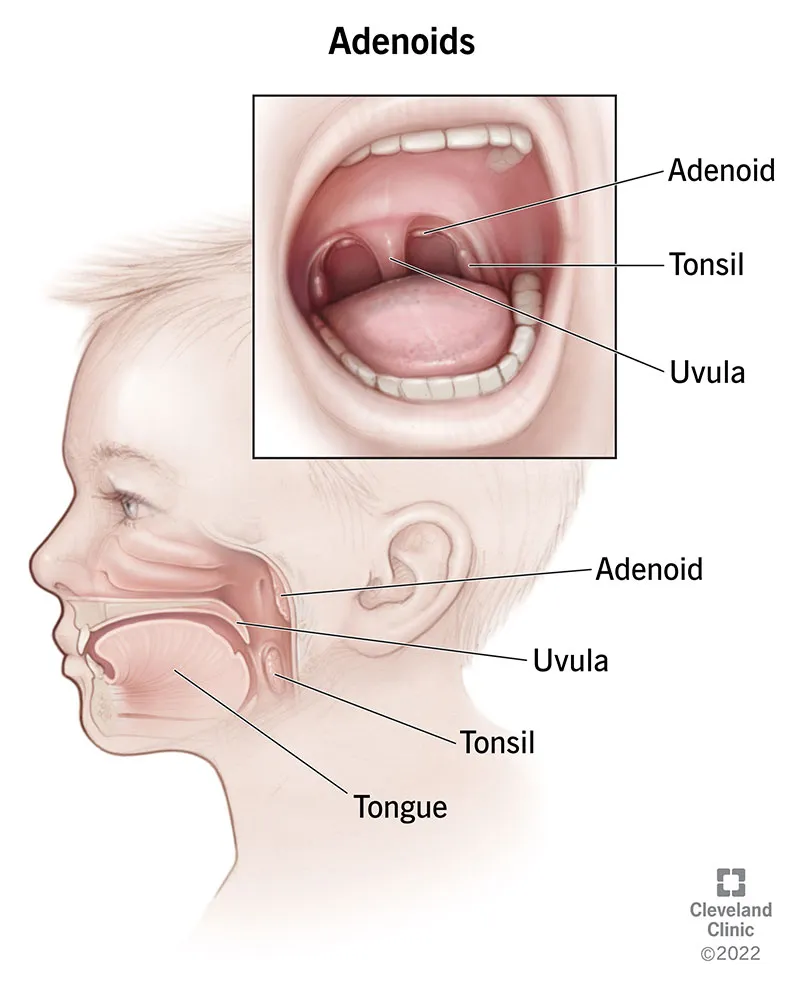
- Major cause: Adenotonsillar hypertrophy.
- Consequences: Can lead to neurocognitive deficits (ADHD-like symptoms), behavioral issues, failure to thrive, & cardiovascular problems (e.g., cor pulmonale in severe cases).
⭐ Untreated POSA can significantly impact a child's learning ability and school performance due to daytime sleepiness and attention deficits. Nightly snoring with apneic pauses is a key indicator for referral and evaluation (Polysomnography - PSG is gold standard).
Pediatric Obstructive Sleep Apnea - Key Causes & Risks
-
Dominant Cause:
- Adenotonsillar hypertrophy (ATH): Accounts for >80% of cases.
- Enlarged tonsils and adenoids physically narrow the pharyngeal airway.
- Adenotonsillar hypertrophy (ATH): Accounts for >80% of cases.
-
Contributing Anatomical Factors:
- Craniofacial anomalies: Micrognathia, retrognathia (e.g., Pierre Robin), midface hypoplasia.
- Nasal obstruction: Chronic rhinitis, septal deviation, turbinate hypertrophy.
-
Systemic & Neuromuscular Factors:
- Obesity: Increasingly prevalent contributor.
- Neuromuscular disorders: Hypotonia (e.g., Down syndrome, cerebral palsy).
- Genetic syndromes: Prader-Willi, mucopolysaccharidoses.
-
Key Risk Factors:
- Family history of OSA.
- Prematurity.
- Passive smoking.
- Uncontrolled allergic rhinitis.
⭐ The presence of adenotonsillar hypertrophy is the single most significant etiological factor in pediatric OSA, often correctable by adenotonsillectomy (T&A).
Pediatric Obstructive Sleep Apnea - Symptoms & Diagnosis
Symptoms:
- Nighttime:
- Loud, habitual snoring (>3 nights/week)
- Witnessed apneas, gasping, choking
- Mouth breathing, restless sleep, enuresis (secondary)
- Daytime:
- Hyperactivity, inattention, learning difficulties
- Morning headaches, daytime sleepiness (less common than adults)
- Failure to thrive (severe cases)
Diagnosis:
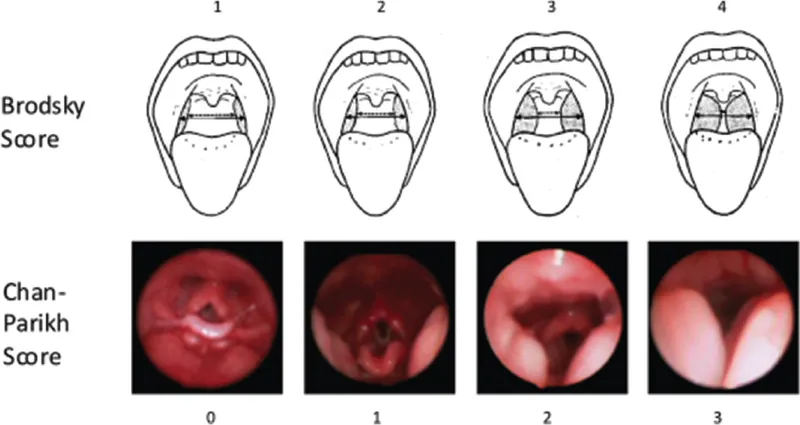
- Clinical Assessment: Detailed history, physical exam (adenotonsillar hypertrophy - Brodsky grade, craniofacial anomalies, obesity)
- Polysomnography (PSG): Gold Standard
- Apnea-Hypopnea Index (AHI) > 1 event/hour: Diagnostic
- Severity: Mild (1-5), Moderate (>5-10), Severe (>10 events/hr)
- Screening tools: Overnight oximetry, validated questionnaires (limited diagnostic value alone)
⭐ Polysomnography (PSG) is the gold standard for diagnosing pediatric OSA; an Apnea-Hypopnea Index (AHI) > 1 event/hour is diagnostic in children.
Pediatric Obstructive Sleep Apnea - Treatment & Outcomes
Treatment Goals: Normalize breathing, improve sleep quality & daytime symptoms.
- First-line:
- Adenotonsillectomy (T&A): Primary treatment if adenotonsillar hypertrophy. Success ~80%.
⭐ T&A is curative in most uncomplicated pediatric OSA cases due to adenotonsillar hypertrophy.
- Adenotonsillectomy (T&A): Primary treatment if adenotonsillar hypertrophy. Success ~80%.
- Second-line/Adjunctive:
- CPAP/BiPAP: For persistent OSA post-T&A, or if T&A contraindicated/ineffective.
- Weight Management: Crucial for obese children.
- Intranasal Corticosteroids: Mild OSA or rhinitis.
- Rapid Maxillary Expansion (RME): For specific craniofacial anomalies.
- Montelukast: May be used for mild OSA.
- Observation: For very mild cases (AHI <5/hr without significant desaturation or comorbidities).
Management Flowchart:
Outcomes of Untreated OSA:
- Neurocognitive: ↓Attention, learning difficulties, behavioral issues (ADHD-like).
- Cardiovascular: ↑BP, endothelial dysfunction; rarely pulmonary hypertension.
- Growth: Failure to thrive or obesity.
- Metabolic: Insulin resistance.
High-Yield Points - ⚡ Biggest Takeaways
- Adenotonsillar hypertrophy is the most common cause of pediatric OSA.
- Nocturnal symptoms include snoring, witnessed apneas, restless sleep, and enuresis.
- Daytime manifestations include mouth breathing, hyponasal speech, neurobehavioral issues (e.g., ADHD-like symptoms), and poor school performance.
- Polysomnography (PSG) is the gold standard for diagnosis.
- An Apnea-Hypopnea Index (AHI) > 1 event/hour is diagnostic in children.
- Adenotonsillectomy is the first-line treatment for most cases.
- Untreated pediatric OSA can lead to failure to thrive, cardiovascular complications (like cor pulmonale), and neurocognitive deficits.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

