Reconstruction Techniques - Skull Base Fix-Up
- Primary Goals: Watertight dural closure (prevent CSF leak), structural support, neurovascular protection, dead space obliteration.
- Reconstructive Ladder:
- Innermost Layer: Grafts (fascia lata, fat, dermal, AlloDerm®).
- Vascularized Layer:
- Local Flaps: Pericranial, temporalis muscle.
- Regional Pedicled Flaps: Nasoseptal flap (NSF) - endonasal workhorse. Others: Pectoralis major, latissimus dorsi.
- Free Flaps (large/complex defects): Anterolateral thigh (ALT), rectus abdominis.
- Principles: Tension-free closure, vascularized tissue for high-risk defects (prior surgery/radiation, high-flow CSF leak).
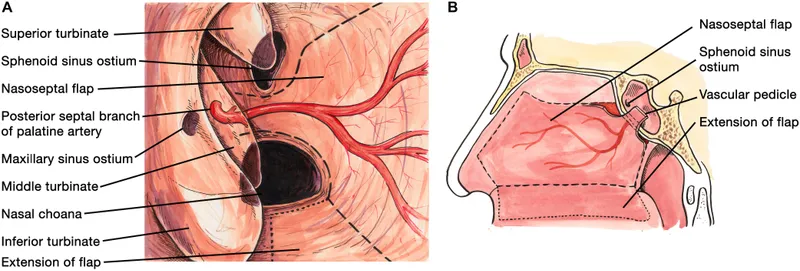
⭐ The Hadad-Bassagasteguy flap (pedicled nasoseptal) revolutionized endoscopic skull base surgery, significantly ↓ CSF leak rates.
Reconstruction Techniques - Simple Patches
- Definition: Single layer of non-vascularized tissue used to seal small dural defects (< 1-1.5 cm).
- Types (Grafts):
- Autografts: Harvested from the patient.
- Fascia lata (thigh)
- Temporalis fascia
- Mucoperichondrium/mucoperiosteum (nasal septum)
- Abdominal fat
- Dura mater (cadaveric - less common now)
- Allografts: From a donor of the same species (e.g., cadaveric dura, acellular dermal matrix).
- Xenografts: From a different species (e.g., porcine dermis).
- Synthetic materials: e.g., collagen matrix, GORE-TEX.
- Autografts: Harvested from the patient.
- Technique:
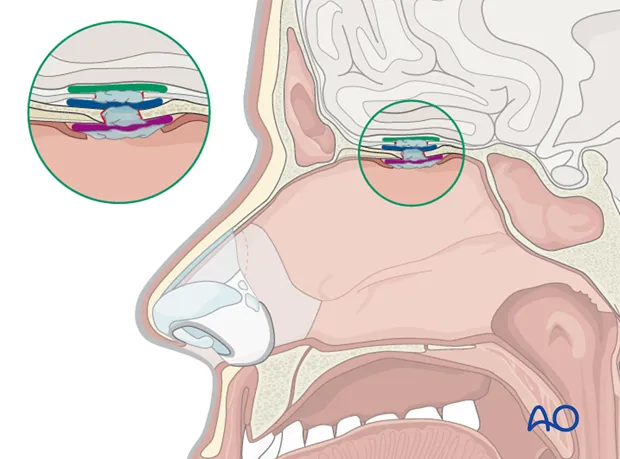
- Underlay: Placed deep to the dural defect.
- Overlay: Placed superficial to the dural defect.
- Inlay: Tucked into the defect.
- Often supported by fibrin glue or sutures.
- Advantages: Simple, readily available, minimal donor site morbidity (for some autografts).
- Disadvantages: No independent blood supply, risk of resorption, CSF leak if seal is inadequate.
⭐ Fascia lata is a commonly used autograft for skull base repair due to its strength and ease of harvest; however, it lacks its own blood supply, relying on the recipient bed for vascularization.
- 📌 Mnemonic (F.A.T.): Fascia, Acellular dermis, Temporalis fascia for common patches.
Reconstruction Techniques - Local Heroes
- Pedicled flaps: Maintain native blood supply; no microanastomosis. Key for multi-layer closure.
- Nasoseptal Flap (NSF) / Hadad-Bassagasteguy Flap
- Artery: Posterior septal a. (br. of sphenopalatine a.)
- Uses: Sella, planum, clivus, olfactory groove.
- 📌 "Workhorse" for endoscopic anterior skull base.
⭐ Most common vascularized flap for endoscopic endonasal skull base repair; robust vascularity, wide arc of rotation.
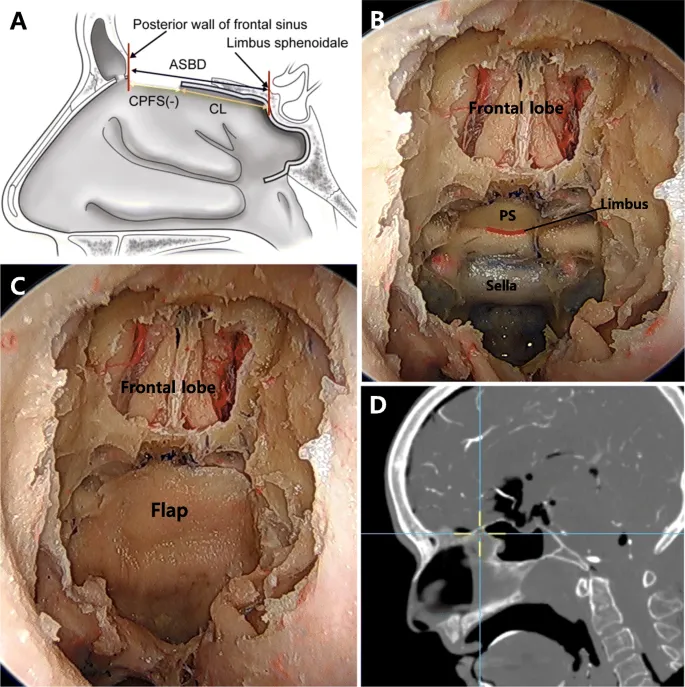
- Pericranial Flap (PCF)
- Artery: Supraorbital & supratrochlear aa.
- Uses: Large anterior cranial fossa defects. Open/endoscopic harvest.
- Temporoparietal Fascia Flap (TPFF)
- Artery: Superficial temporal a.
- Uses: Lateral skull base, orbit, mid-fossa. Thin, pliable.
- Temporalis Muscle Flap
- Artery: Deep temporal aa. (from maxillary a.)
- Uses: Mid-fossa, infratemporal fossa. Provides bulk.
Reconstruction Techniques - Big Guns
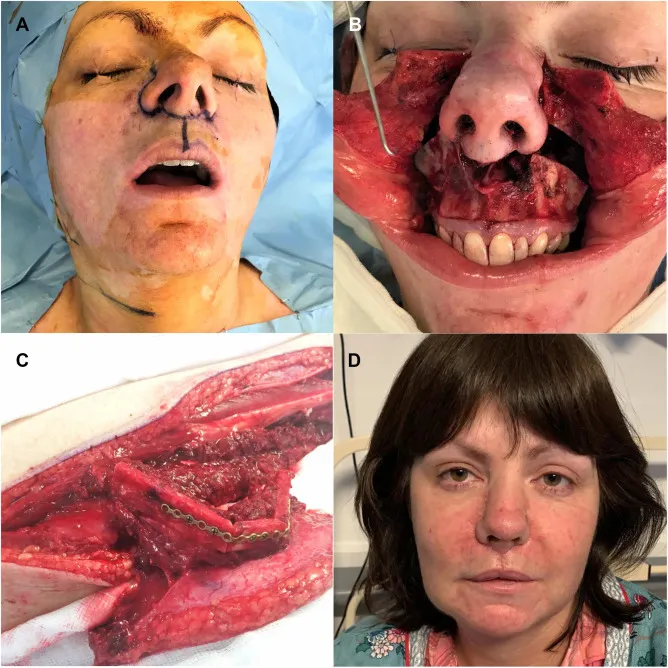
- Free Flaps (Microvascular Anastomosis): Utilized for extensive, complex defects requiring distant tissue transfer and dedicated blood supply.
- Anterolateral Thigh (ALT) Flap:
- Workhorse flap; fasciocutaneous or myocutaneous.
- Versatile, reliable; provides large skin paddle and/or bulk.
- Pedicle: Descending branch of lateral circumflex femoral artery.
- Rectus Abdominis Myocutaneous (RAM) Flap:
- Vertical (VRAM) or Transverse (TRAM).
- Offers significant bulk for dead space obliteration.
- Pedicle: Deep inferior epigastric artery.
- Latissimus Dorsi (LD) Flap:
- Largest potential surface area; muscle or myocutaneous.
- Pedicle: Thoracodorsal artery.
- Radial Forearm Free Flap (RFFF):
- Thin, pliable tissue; excellent for lining or dural reconstruction.
- Pedicle: Radial artery.
- Anterolateral Thigh (ALT) Flap:
- Large Regional Pedicled Flaps:
- Pectoralis Major Myocutaneous (PMMC) Flap:
- Robust, reliable option for anterior and middle cranial fossa defects.
- Pedicle: Thoracoacromial artery.
- Pectoralis Major Myocutaneous (PMMC) Flap:
⭐ The Anterolateral Thigh (ALT) flap is frequently the first choice free flap for skull base reconstruction due to its consistent anatomy, long pedicle, and ability to provide chimeric components (skin, fascia, muscle).
High‑Yield Points - ⚡ Biggest Takeaways
- Vascularized flaps (e.g., Nasoseptal, Pericranial) are superior to free grafts, minimizing CSF leaks.
- Nasoseptal Flap (NSF) is the workhorse for endoscopic endonasal approaches (EEA).
- Pedicled pericranial flap is crucial for open anterior skull base defects.
- Temporoparietal Fascial Flap (TPFF) reconstructs lateral skull base defects.
- Free flaps (e.g., ALT) are for large defects or when local/regional flaps fail.
- Multilayer closure (fascia lata, fat, vascularized flap) is key for robust repair.
- Post-op lumbar drain can reduce CSF pressure, aiding healing_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

