Introduction - Brain's Unwanted Tenant
- Most common primary intracranial tumors; generally benign & slow-growing.
- Origin: Arachnoid (meningothelial) cap cells.
- Peak incidence: 40-60 years; F:M ratio ~2:1 (intracranial), ~10:1 (spinal).
- Common skull base locations:
- Sphenoid wing
- Olfactory groove
- Tuberculum sellae
- Petroclival region
- Foramen magnum
- WHO Classification: Grade I (benign, ~90%), Grade II (atypical), Grade III (malignant).
⭐ Multiple meningiomas or association with schwannomas/gliomas suggests Neurofibromatosis type 2 (NF2).
Pathology & Grading - Growth's True Colors
- Origin: Arachnoid cap cells.
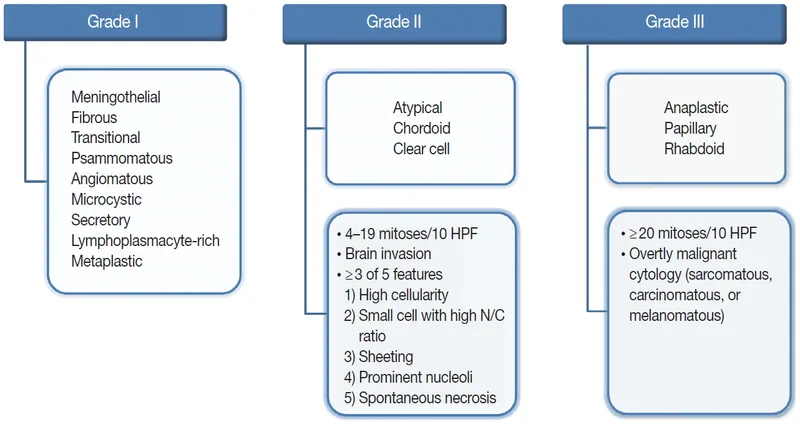
- WHO Grading (2021):
- Grade I (Benign, ~80%): Meningothelial, Fibroblastic, Transitional, Psammomatous. Slow growth.
- Grade II (Atypical, ~15-20%): Mitotic index ≥4/10 HPF, brain invasion, or 3+ atypical features (e.g. ↑cellularity). Includes Chordoid, Clear Cell.
- Grade III (Malignant, ~1-3%): Mitotic index ≥20/10 HPF, anaplasia. Includes Papillary, Rhabdoid.
- IHC: EMA+, Vimentin+, SSTR2A+. Ki-67 index correlates with grade.
- Risk: NF2 mutation, radiation.
⭐ Brain invasion automatically upgrades a meningioma to WHO Grade II, irrespective of other histological features.
Clinical Features - Cranial Nerve Chaos
Symptoms reflect tumor location & compressed cranial nerves (CNs).
- Olfactory Groove: Anosmia (CN I), personality changes.
- Tuberculum Sellae/Suprasellar: Visual loss (CN II), bitemporal hemianopia, optic atrophy.
- Sphenoid Wing: Proptosis; CN II, III, IV, V, VI deficits (vision loss, diplopia, facial numbness).
- Cavernous Sinus: Multiple ophthalmoplegias (CN III, IV, VI), trigeminal sensory loss (V1/V2).
- Petroclival: CN V-VIII dysfunction (facial pain, diplopia, hearing loss, facial weakness), ataxia.
- Foramen Magnum: Lower CN palsies (IX-XII), motor deficits, hydrocephalus.
⭐ Foster Kennedy Syndrome: Ipsilateral anosmia & optic atrophy + contralateral papilledema (olfactory groove meningioma).
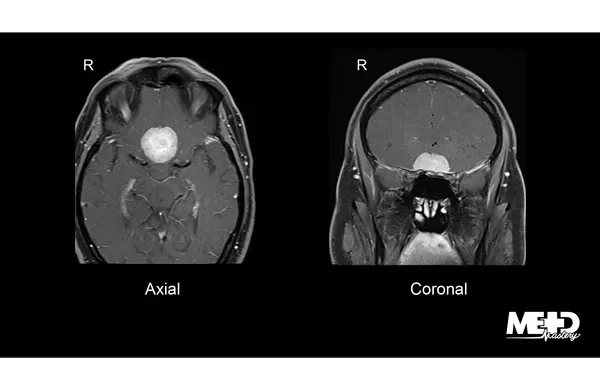
Diagnostic Imaging - Spotting the Shadow
- MRI (Gold Standard):
- T1: Iso/hypointense.
- T2: Iso/hyperintense; peritumoral edema.
- T1 C+ (Gad): Intense, homogenous enhancement.
- Dural Tail Sign: Enhancing adjacent dural thickening (📌).
- CT Scan:
- Often hyperdense.
- Calcification, bony hyperostosis/erosion.
- Angiography (DSA):
- Feeding vessels (ECA branches).
- Pre-op embolization.
- Sunburst/Mother-in-law sign.

⭐ The "dural tail sign" on contrast-enhanced MRI, seen in ~60-70% of cases, is highly suggestive but not pathognomonic for meningioma.
Management Strategies - Taming the Tumor
- Goal: Symptom relief, tumor control, preserve/improve neurological function.
- Options: Observation, Surgery, Radiotherapy.
- Surgery:
- Aim: Maximal safe resection to achieve GTR.
- Approaches: Transcranial, Endoscopic Endonasal.
- Complications: Cranial nerve deficits, CSF leak.
- Radiotherapy:
- Stereotactic Radiosurgery (SRS) or Fractionated (FSRT).
- Indications: Adjuvant post-STR, recurrent, primary for inoperable/high-risk tumors.
- Consider for WHO Grade II/III.

⭐ Simpson Grade I resection (complete tumor removal including dural attachment and abnormal bone) offers the lowest recurrence rate for benign meningiomas.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common benign intracranial tumor, frequently at the skull base.
- WHO Grade I is most common; Grades II & III have higher recurrence.
- Characteristic histology: Psammoma bodies.
- Simpson grading of surgical resection predicts recurrence rates.
- Symptoms often include cranial nerve deficits depending on tumor location.
- Maximal safe surgical resection is the goal; radiotherapy for adjuvant/salvage.
- Higher incidence in females; associated with Neurofibromatosis Type 2 (NF2).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

