Basics & Spread - Sinus Sneak Attack
- Definition: Orbital complications arise from infection or inflammation spreading from the paranasal sinuses to the orbit.
- Causative Organisms: Common culprits include Streptococcus pneumoniae, Haemophilus influenzae, Staphylococcus aureus, and anaerobes.
- Most Common Sinus: Ethmoid sinus.
- Pathways of Spread:
- Direct extension (e.g., through the thin lamina papyracea).
- Thrombophlebitis of valveless veins (e.g., ophthalmic veins).
- Lymphatics (less common).
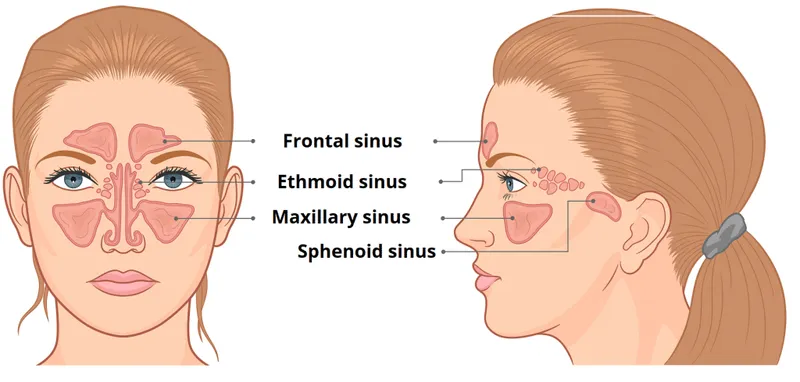
⭐ The ethmoid sinus is most commonly implicated in orbital complications due to the thinness of the lamina papyracea and its valveless venous drainage system facilitating spread of infection.
Chandler's Ladder - Staging the Siege
📌 Mnemonic: POSOC
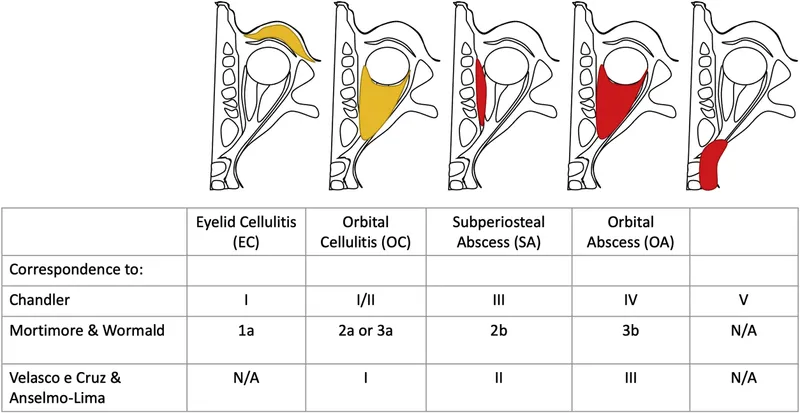
| Stage | Name (Mnemonic) | Key Features & Signs |
|---|---|---|
| I | Inflammatory Edema (Preseptal Cellulitis) (P) | Eyelid swelling, erythema. Normal vision, no proptosis/ophthalmoplegia. |
| II | Orbital Cellulitis (O) | Proptosis, chemosis, ophthalmoplegia, ↓ vision. > ⭐ The orbital septum is the key anatomical landmark differentiating preseptal (Stage I) from orbital (Stage II and beyond) cellulitis. |
| III | Subperiosteal Abscess (S) | Proptosis (often inferolateral), ophthalmoplegia, ↓ vision. Pus between bone & periosteum. |
| IV | Orbital Abscess (O) | Severe proptosis, ophthalmoplegia (often complete), marked ↓ vision/blindness. Pus within orbital tissues. |
| V | Cavernous Sinus Thrombosis (C) | Bilateral signs, proptosis, ophthalmoplegia, severe ↓ vision, CN palsies (III-VI), meningeal signs. |
Signs & Scans - Orbital Investigation
-
Clinical Clues (Chandler Stages):
- Stage 1 (Preseptal): Lid edema, erythema. Normal vision & EOM.
- Stage 2 (Orbital Cellulitis): Proptosis (axial), ophthalmoplegia, chemosis, pain, fever.
⭐ CECT is imaging of choice for diagnosis & delineating disease extent.
- Stage 3 (Subperiosteal Abscess): Non-axial proptosis, diplopia, restricted EOM.
- Stage 4 (Orbital Abscess): Severe proptosis, ophthalmoplegia, ↓VA, RAPD.
- Stage 5 (Cavernous Sinus Thrombosis): Bilateral signs, CN III, IV, V1, VI palsies.
-
Imaging Gold Standard:
- CECT PNS & Orbit (Axial, Coronal, Sagittal): Shows extent, abscess.
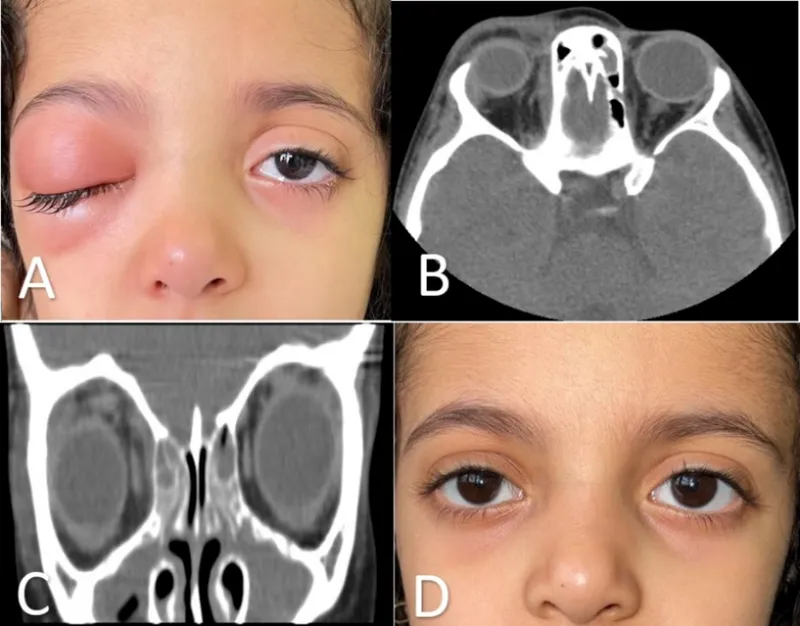
- MRI: If intracranial/cavernous sinus spread suspected.
- CECT PNS & Orbit (Axial, Coronal, Sagittal): Shows extent, abscess.
-
Diagnostic Flow:
Treatment Arsenal - Combatting Complications
Medical Management:
- Immediate Hospitalization.
- IV Antibiotics (e.g., Ceftriaxone + Vancomycin, or Clindamycin); crucial cover for Gram +, Gram -, anaerobes.
- Adjuncts: Nasal decongestants, analgesics.
- Steroids: Controversial; consider for optic neuropathy if no frank abscess.
Surgical Management:
- Indications:
- Orbital/Subperiosteal abscess >10mm or significant volume.
- Vision compromise (↓VA, RAPD, proptosis, ophthalmoplegia).
- No improvement post 24-48h IV antibiotics.
- Intracranial complications.
- Approaches:
- Endoscopic Sinus Surgery (ESS) for drainage (primary).
- External approaches (Lynch, transcaruncular) if ESS fails/inadequate.
⭐ Any evidence of optic nerve compromise (e.g., decreased visual acuity, RAPD) or a significant abscess on imaging (e.g., >10mm) typically warrants prompt surgical drainage.
Grave Threats - Vision & Life
- Cavernous Sinus Thrombosis (CST): Bilateral proptosis, ophthalmoplegia (CN III, IV, VI), V1/V2 loss, fever, sepsis. Rx: IV antibiotics, ?anticoagulation.
- Blindness: Optic neuritis, ischemic neuropathy, compression.
- Intracranial: Meningitis, abscesses (epidural/subdural/brain).
- Prognosis: Stage, treatment speed, CST dependent.
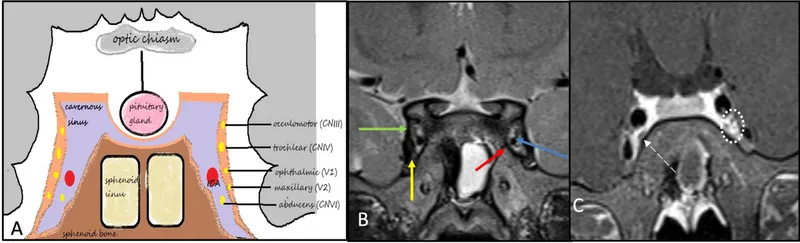
⭐ Bilateral orbital signs, multiple cranial nerve palsies (III, IV, V1, V2, VI), and severe sepsis strongly suggest CST.
High‑Yield Points - ⚡ Biggest Takeaways
- Chandler's classification is key: I-Preseptal, II-Orbital cellulitis, III-Subperiosteal abscess, IV-Orbital abscess, V-Cavernous sinus thrombosis.
- Ethmoid sinusitis is the most common origin.
- CT scan with contrast is crucial for diagnosis.
- Orbital cellulitis features proptosis, ophthalmoplegia, and ↓ vision, unlike preseptal.
- Subperiosteal and orbital abscesses often require urgent surgical drainage.
- Cavernous sinus thrombosis: critical, bilateral signs, multiple CN palsies.
- Management: IV antibiotics; surgical drainage for abscesses or failed medical therapy an indication for surgery
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

