IFS Overview - Fungal Foes
- Life-threatening fungal infection with invasion of sinonasal mucosa, submucosa, vasculature, and bone.
- Primarily affects immunocompromised individuals (diabetes, neutropenia, steroid use).
- Key Fungal Agents:
- Aspergillus spp. (commonest worldwide)
- Mucorales (e.g., Rhizopus, Mucor; prominent in India, esp. post-COVID)
- Major Clinical Types:
- Acute Invasive Fungal Sinusitis (AIFS): Rapid onset (<4 weeks), angioinvasion, necrosis.
- Chronic Invasive Fungal Sinusitis (CIFS): Indolent (>12 weeks), may involve granulomas or be non-granulomatous.
⭐ Acute Invasive Fungal Sinusitis (AIFS) is a medical emergency requiring prompt intervention.
 ## IFS Overview - Fungal Foes
## IFS Overview - Fungal Foes
- Life-threatening fungal infection with invasion of sinonasal mucosa, submucosa, vasculature, and bone.
- Primarily affects immunocompromised individuals (diabetes, neutropenia, steroid use).
- Key Fungal Agents:
- Aspergillus spp. (commonest worldwide)
- Mucorales (e.g., Rhizopus, Mucor; prominent in India, esp. post-COVID)
- Major Clinical Types:
- Acute Invasive Fungal Sinusitis (AIFS): Rapid onset (<4 weeks), angioinvasion, necrosis.
- Chronic Invasive Fungal Sinusitis (CIFS): Indolent (>12 weeks), may involve granulomas or be non-granulomatous.
⭐ Acute Invasive Fungal Sinusitis (AIFS) is a medical emergency requiring prompt intervention.
(image)[2931967b-4999-43ac-b7fc-7221e1105eb7]
Risk Factors & Pathogens - Susceptible Sinuses
- Key Risk Factors: Severe immunocompromise.
- Diabetes Mellitus (esp. DKA 📌)
- Hematological malignancies (leukemia, lymphoma)
- Neutropenia (ANC <500/µL)
- Solid organ/stem cell transplant recipients
- Prolonged high-dose corticosteroids
- HIV/AIDS (CD4 <200 cells/µL)
- Common Pathogens:
- Mucorales (e.g., Rhizopus oryzae, Mucor): Broad, non-septate hyphae, right-angle branching. Angioinvasion common.
⭐ Mucormycosis shows a strong predilection for patients with diabetic ketoacidosis (DKA) due to the acidic, glucose-rich environment.
- Aspergillus spp. (e.g., A. fumigatus, A. flavus): Septate hyphae, acute (45°) angle branching.
- Mucorales (e.g., Rhizopus oryzae, Mucor): Broad, non-septate hyphae, right-angle branching. Angioinvasion common.
- Sinus Predilection:
- Maxillary (most common), Ethmoid, Sphenoid, Frontal.
- Typically unilateral onset.

Clinical Picture - Sinister Signs
- Rapidly progressive symptoms (hours to days).
- Severe facial pain, headache, facial numbness (CN V).
- Periorbital edema, proptosis, ophthalmoplegia (CN III, IV, VI), diplopia.
- Acute visual loss (CN II).
- Nasal:
- Black necrotic eschar on turbinates/septum.
- Purulent, bloody, or foul discharge.
- Palatal or gingival necrosis (black lesions).
- Fever (often low-grade/absent).
- Altered mental status (late, poor prognosis).
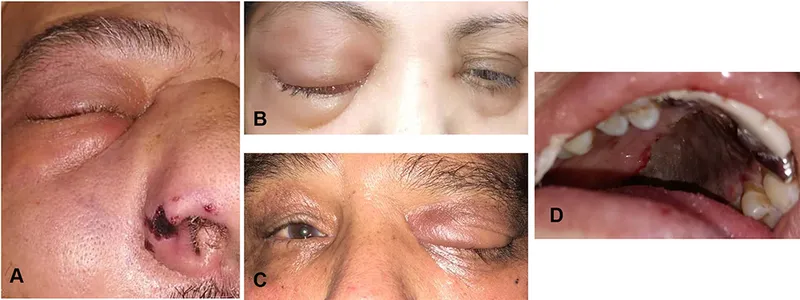
⭐ The presence of a black necrotic eschar in the nasal cavity or on the palate is a hallmark sign highly suggestive of mucormycosis.
Diagnosis & Imaging - Unmasking Invaders
- Nasal Endoscopy: Crucial first step. Look for pale, dusky, or black necrotic tissue (turbinates, septum), eschar formation. Insensitivity of mucosa.
- Biopsy (Urgent & Multiple): From suspicious areas. Send for:
- HPE (Frozen section if available): Shows hyphal invasion of tissue, vessels.
⭐ Histopathological examination (HPE) of a biopsy specimen demonstrating fungal hyphae invading tissue is the gold standard for diagnosing IFS.
- Microbiology: KOH mount (rapid), fungal culture & sensitivity.
- Imaging:
- CECT (PNS, Orbit, Brain): Initial. Bone erosion/destruction, unilateral opacification, perisinus fat stranding.

- MRI with Gadolinium (PNS, Orbit, Brain): Superior for soft tissue, early intracranial/orbital spread, cavernous sinus thrombosis. T2 hypointensity (fungal elements), variable enhancement.
- CECT (PNS, Orbit, Brain): Initial. Bone erosion/destruction, unilateral opacification, perisinus fat stranding.
Treatment & Prognosis - Fungus Fightback
- Core Strategy: Aggressive, multimodal.
- Surgical Debridement: Prompt, wide excision of necrotic tissue.
- Systemic Antifungals: Liposomal Amphotericin B (L-AMB); Voriconazole/Posaconazole as alternatives.
- Control Predisposing Factors: E.g., manage diabetes, neutropenia.
- Prognosis: Guarded. Early, aggressive intervention is key.
- Mortality: High; depends on host immunity, disease extent.
- Poor Prognosis: Intracranial/orbital spread, delayed Rx.
⭐ Liposomal Amphotericin B is generally preferred over conventional Amphotericin B for treating IFS due to its improved renal safety profile and better tissue penetration.
High‑Yield Points - ⚡ Biggest Takeaways
- Affects immunocompromised patients, especially with uncontrolled diabetes or neutropenia.
- Mucor and Aspergillus species are the most common causative fungi.
- Classic sign: black necrotic eschar in the nasal cavity or palate.
- Characterized by rapid angioinvasion causing tissue necrosis and orbital/intracranial spread.
- Diagnosis: Biopsy for histopathology (hyphal invasion) is key, with CT/MRI imaging.
- Treatment: Urgent, aggressive surgical debridement plus systemic IV Amphotericin B.
- Carries high mortality despite prompt, aggressive management.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

