ICS Pathways - Sinus Breach Alert
- Pathways of Infection:
- Direct Extension: Through bony erosion (osteitis/osteomyelitis) or pre-existing dehiscence (e.g., trauma, surgery). Common in chronic sinusitis.
- Leads to: Epidural abscess, subdural empyema, brain abscess.
- Venous Spread (Retrograde Thrombophlebitis): Via valveless diploic veins (of Breschet) & communicating veins. Bacteria travel against blood flow. Most common route in acute sinusitis.
- Leads to: Cavernous sinus thrombosis, cortical vein thrombosis, meningitis, brain abscess.
- Lymphatic Spread: Less significant for ICS.
- Perineural Spread: Along olfactory nerve filaments through cribriform plate (rare).
- Direct Extension: Through bony erosion (osteitis/osteomyelitis) or pre-existing dehiscence (e.g., trauma, surgery). Common in chronic sinusitis.
⭐ Frontal sinus is the most common source of intracranial complications from sinusitis, particularly epidural abscess and subdural empyema.
Pus Pockets - Abscesses Unmasked
| Feature | Epidural Abscess | Subdural Empyema | Brain Abscess |
|---|---|---|---|
| Location | Skull-Dura | Dura-Arachnoid | Brain parenchyma |
| Organisms | Strep, Staph, Anaerobes | Strep, Staph, Anaerobes | Polymicrobial; Strep, Staph, Anaerobes |
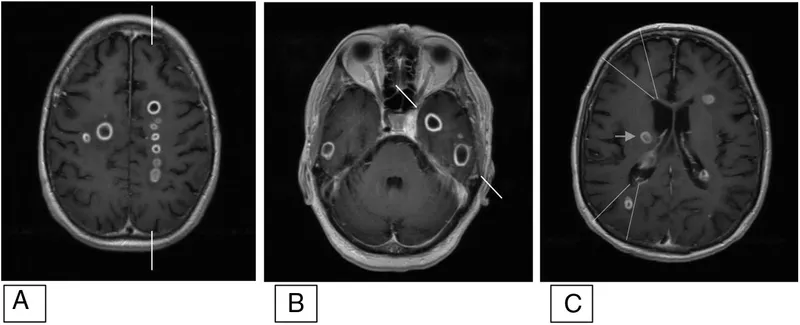
| CT/MRI | Lentiform, biconvex; no suture crossing | Crescentic; crosses sutures, interhemispheric | Ring-enhancing lesion; central necrosis, edema |
| Clinical | Fever, headache, focal signs; Pott's Puffy Tumor | Rapid; high fever, seizures, ↑ICP | Headache, fever, focal deficits; 📌 CLEMA stages |
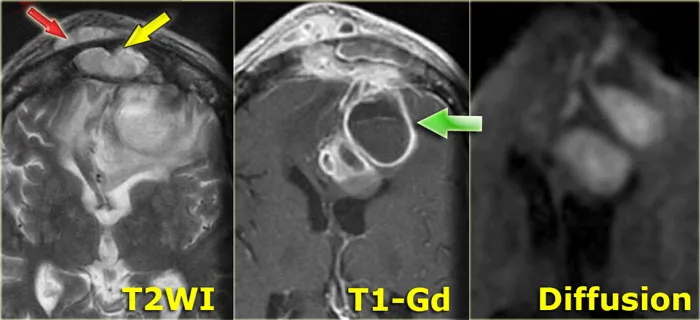
⭐ Pott's Puffy Tumor: Frontal bone subperiosteal abscess (osteomyelitis) with frontal sinusitis, often linked to epidural abscess.
📌 Brain Abscess Stages (CLEMA): Cerebritis Early, Late Cerebritis, Early Capsule, Mature (Late) Capsule, Abscess.
Flow & Fire - Clots & Meningitis
- Cavernous Sinus Thrombosis (CST)
- Spread: Valveless veins from sinus (esp. sphenoid/ethmoid) or facial infection.
- Symptoms: Proptosis, chemosis, painful ophthalmoplegia, fever, headache.
- Signs: CN III, IV, V1, V2, VI palsy. 📌 CNs: 3, 4, 6, V1, V2.
- Imaging: MRI with MRV.

- Meningitis
- Spread: Direct extension from sinuses or hematogenous.
- Symptoms: Fever, headache, nuchal rigidity, Altered Mental Status (AMS).
- CSF Analysis:
- Bacterial: ↑Pressure, ↑PMNs, ↑Protein, ↓Glucose.
- Viral: Normal/↑Pressure, ↑Lymphocytes, Normal/↑Protein, Normal Glucose.

⭐ Cavernous sinus thrombosis classically presents with proptosis, chemosis, ophthalmoplegia, and involvement of CN III, IV, V1, V2, and VI.
Detect & Defeat - Spot & Stop ICS
-
Spot ICS (Red Flags): 📌 Mnemonic: "PAIN"
- Proptosis/Periorbital edema, Papilledema
- Altered mental status (AMS), seizures
- Intense headache (persistent, severe), high Fever
- Neurological deficits (focal, CN palsies)
-
Key Investigations:
- CECT Head & Sinuses: Rapid initial assessment (bone erosion, collections).
- MRI Brain + MRV (Gadolinium): Gold standard for defining extent, type (abscess, meningitis, DVST).
⭐ MRI with gadolinium contrast is the gold standard for suspected intracranial complications of sinusitis.
- Management Approach:
- Treatment Pearls:
- Aggressive, prompt therapy is vital.
- Antibiotics: Broad-spectrum, CNS penetrating, prolonged duration (4-8 weeks).
- Surgery: Drain sinuses (ESS) AND intracranial collections if present & indicated.
High‑Yield Points - ⚡ Biggest Takeaways
- Epidural abscess is the most common intracranial complication of sinusitis.
- Frontal sinus is the most frequent source, linked to Pott's Puffy Tumor.
- Spread occurs via direct extension (osteomyelitis) or retrograde thrombophlebitis (Breschet's veins).
- CECT is initial imaging; MRI with gadolinium is gold standard for diagnosis.
- Severe complications: Meningitis, subdural empyema, brain abscess, cavernous sinus thrombosis.
- Suspect with persistent headache, fever, altered sensorium, or focal neurological deficits.
- Treatment: High-dose IV antibiotics and prompt surgical drainage of sinuses/abscess.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

