History & Initial Exam - The First Listen
- Voice History:
- Onset, duration, severity.
- Associated symptoms: Pain, dysphagia, GERD, cough.
- Vocal hygiene: Vocal load, smoking, hydration.
- Med/Surg Hx: Thyroid surg, intubation, neuro.
- Social/Occ impact: Prof. voice users.
- "First Listen" (Auditory):
- Pitch, loudness, quality (hoarse, breathy, strained).
- H&N Exam (Voice-Relevant):
- Oral cavity/oropharynx.
- Neck: Masses, tenderness, laryngeal crepitus.
- CN IX, X, XII screen.
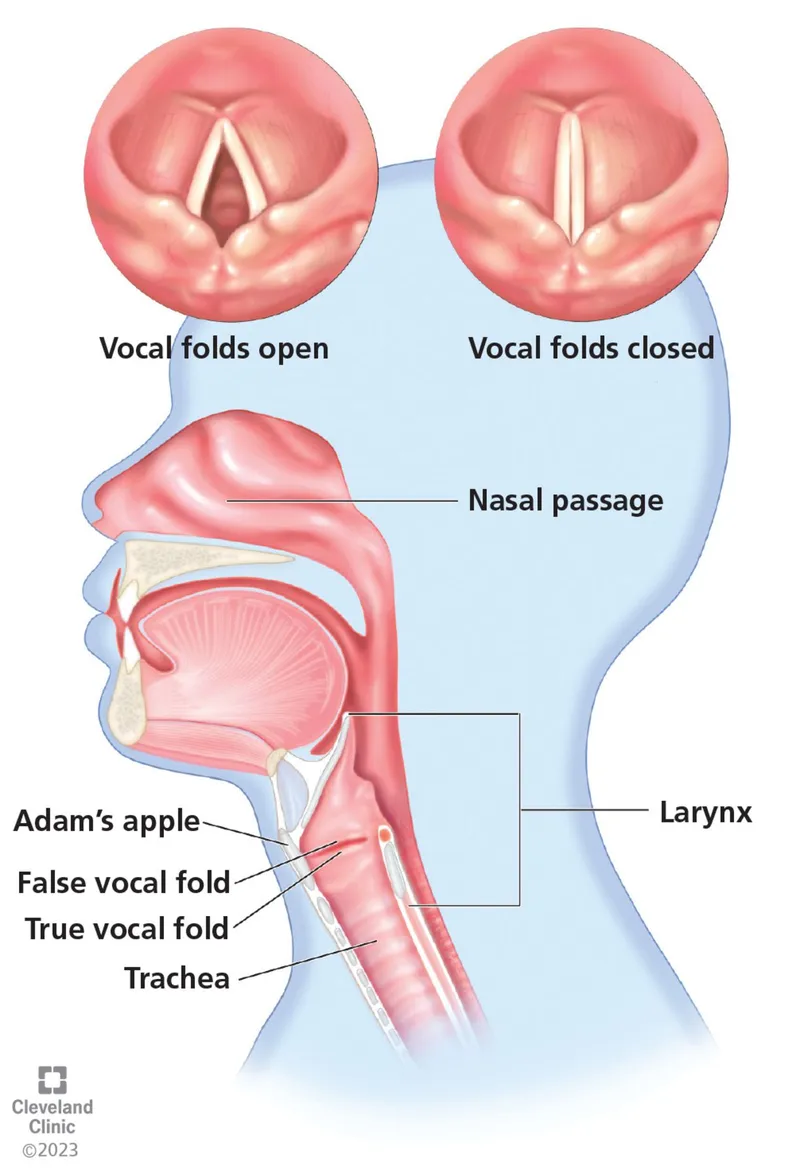
⭐ Hoarseness > 3 weeks, esp. in smokers or with red flags (e.g., pain, hemoptysis), mandates laryngoscopy.
Perceptual Evaluation - Ear on Quality
-
Subjective assessment of voice quality by listening.
-
GRBAS Scale: 📌 Great Rhinos Bellow At Sunsets. Assesses five parameters:
- Grade: Overall hoarseness severity.
- Roughness: Perceived vocal fold vibration irregularity.
- Breathiness: Audible air escape during phonation.
- Asthenia: Vocal weakness or lack of power.
- Strain: Perception of excessive vocal effort.
- Each scored 0 (Normal) to 3 (Severe).
Score Description 0 Normal 1 Mild 2 Moderate 3 Severe -
CAPE-V (Consensus Auditory-Perceptual Evaluation of Voice):
- More detailed; uses a 100mm Visual Analog Scale (VAS).
- Parameters: Overall Severity, Roughness, Breathiness, Strain, Pitch, Loudness.
⭐ GRBAS is widely used for its simplicity and speed in clinical settings, making it a valuable tool for initial voice assessment and tracking treatment progress over time based on auditory-perceptual changes noted by the clinician or patient (though primarily clinician-rated).
Laryngeal Imaging - Visual Vibes
Visualizes vocal fold structure & function for diagnosis.
- Videostroboscopy:
- Principle: Talbot's law (illusory slow motion).
- Parameters: Symmetry, Amplitude, Periodicity, Mucosal wave, Glottic closure, Non-vibrating portion.
- High-Speed Videoendoscopy (HSV):
- Actual vocal fold vibration (>2000 fps).
- Best for aperiodic voices.
- Narrow Band Imaging (NBI):
- Enhances mucosal/vascular patterns.
- Detects early dysplasia/malignancy.
- Kymography:
- Single-line vocal fold vibration over time.
| Feature | Videostroboscopy | High-Speed Videoendoscopy (HSV) |
|---|---|---|
| Principle | Talbot's Law (apparent) | Actual motion |
| Aperiodic Voice | Limited | Ideal |
Acoustic & Aerodynamic - Data Driven Diagnosis
| Parameter | Normal Value(s) | Significance of Abnormality |
|---|---|---|
| Acoustic Analysis | ||
| Fundamental Frequency (F0) | Varies (age, sex) | Altered pitch disorders |
| Jitter | < 1% | ↑ vocal instability, mucosal wave changes |
| Shimmer | < 0.5 dB / < 5% | ↑ vocal instability, mass lesions, stiffness |
| HNR (NHR inverse) | > 20 dB | ↓ hoarseness, breathiness (↑ NHR) |
| Aerodynamic Measures | ||
| MPT | 15-25s | ↓ poor glottal closure, respiratory issues |
| s/z Ratio | ~1; > 1.4 (📌) | > 1.4 suggests laryngeal pathology |
| PTP | 3-5 $cm\ H_2O$ | ↑ vocal fold stiffness, edema, mass lesions |
| Laryngeal Airway Resist. | 20-60 $dyne \cdot s/cm^5$ | ↑ hyperfunction, glottic constriction |
Standardized Scales & Special Tests - Holistic View
- Patient-Reported Outcome Measures (PROMs):
- Voice Handicap Index (VHI): Self-perceived voice handicap.
- Domains: Functional, Physical, Emotional (📌 FPE).
- Scoring: 0-30 (Mild), 31-60 (Moderate), 61-120 (Severe).
- Voice-Related Quality of Life (V-RQOL): Impact on voice-related QOL.
- Pediatric VHI (pVHI): For children.
- Voice Handicap Index (VHI): Self-perceived voice handicap.
- Special Tests:
- Laryngeal Electromyography (LEMG):
- Indications: Vocal fold paralysis/paresis, movement disorders.
- Muscles tested: Thyroarytenoid (TA), Cricothyroid (CT), Posterior Cricoarytenoid (PCA).
- Auditory Brainstem Response (ABR): Central neurological causes.
- Laryngeal Electromyography (LEMG):
⭐ VHI scoring: 0-30 (Mild), 31-60 (Moderate), 61-120 (Severe) indicates perceived handicap severity.
High‑Yield Points - ⚡ Biggest Takeaways
- GRBAS scale is crucial for subjective voice assessment (Grade, Roughness, Breathiness, Asthenia, Strain).
- Videostroboscopy is key for visualizing vocal fold vibration and mucosal wave integrity.
- Maximum Phonation Time (MPT), normally >15 seconds, indicates glottic efficiency.
- An S/Z ratio >1.4 strongly suggests laryngeal pathology over respiratory causes.
- The Voice Handicap Index (VHI) measures patient-perceived disability from voice disorders.
- Acoustic analysis provides objective data: jitter, shimmer, and Harmonics-to-Noise Ratio (HNR).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

