Vocal Fold Anatomy - Anatomy Unlayered
- Paired mucosal folds within the larynx, crucial for phonation (voice production).
- Extend from thyroid cartilage (anteriorly) to arytenoid cartilages (posteriorly).
- Length: Adult males 17-23 mm; adult females 12-17 mm.
- Layers (Hirano's Body-Cover Theory): 5 distinct histological layers, grouped into 3 functional sections.
- Cover (Vibratory segment):
- Epithelium: Stratified squamous, non-keratinized.
- Superficial Lamina Propria (SLP) / Reinke's Space: Gelatinous, highly pliable. 📌 Site of Reinke's Edema.
- Transition (Vocal Ligament - provides resilience):
- Intermediate Lamina Propria (ILP): Elastic fibers.
- Deep Lamina Propria (DLP): Collagenous fibers.
- Body (Muscular core - provides bulk & tension):
- Thyroarytenoid (Vocalis) Muscle.
- Cover (Vibratory segment):
- Glottis: Airway space between the true vocal folds.
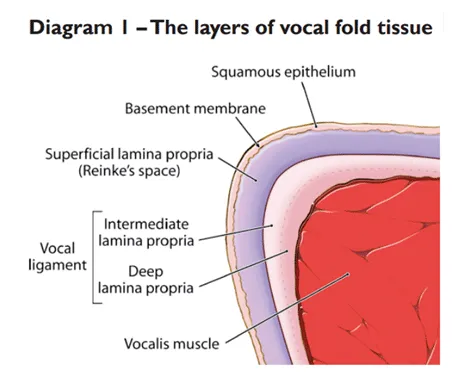
⭐ Reinke's Space (SLP) is the primary vibrating layer; its condition critically impacts voice quality. Fluid accumulation (edema) here is common.
Phonation Physiology - Voice Mechanics
- Myoelastic-Aerodynamic Theory: Voice production via interplay of muscle (myoelastic) & airflow (aerodynamic) forces.
- Vocal folds (VFs) adduct (LCA, IA muscles).
- Subglottic pressure ($P_{sub}$) builds.
- $P_{sub}$ overcomes glottic resistance → VFs open (inferiorly then superiorly).
- Air puff released, $P_{sub}$ drops.
- Bernoulli Principle: ↑ airflow velocity in constricted glottis → ↓ pressure.
- This negative pressure sucks VFs medially, aiding closure (inferiorly first).
- Mucosal Wave: Rippling of VF mucosa over the vocalis muscle.
- Essential for clear, resonant voice; assessed by stroboscopy.
- Reduced/absent in VF stiffness (e.g., scar, sulcus).
⭐ The myoelastic-aerodynamic theory is the most widely accepted model explaining voice production, highlighting the interplay of muscle tension, elasticity, and airflow.
Innervation & Blood Supply - Power & Pipes
-
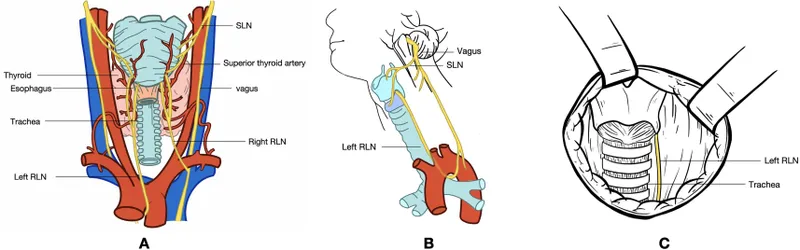
Innervation (Vagus Nerve - CN X):
- Superior Laryngeal Nerve (SLN):
- Internal br: Sensory to supraglottic mucosa (cough reflex).
- External br: Motor to Cricothyroid m. (VF tensor, ↑pitch).
- Recurrent Laryngeal Nerve (RLN):
- Motor: All intrinsic laryngeal muscles (except Cricothyroid); controls VF abduction/adduction.
- Sensory: Infraglottic mucosa & vocal folds.
- 📌 L RLN longer (aortic arch); R RLN (subclavian a.).
⭐ Cricothyroid m. (pitch elevation) is the sole muscle innervated by External SLN.
- Superior Laryngeal Nerve (SLN):
-
Blood Supply:
- Arteries:
- Sup. Laryngeal A. (from Sup. Thyroid A.): Supraglottis; with Int. SLN.
- Inf. Laryngeal A. (from Inf. Thyroid A.): Infraglottis; with RLN.
- Veins:
- Veins parallel arteries: drain to Sup. Thyroid V. (→IJV), Inf. Thyroid V. (→Brachiocephalic V.).
- Arteries:
High‑Yield Points - ⚡ Biggest Takeaways
- Vocal folds: 5 layers (Epithelium, Superficial LP/Reinke's space, Intermediate LP, Deep LP, Vocalis muscle).
- Reinke's space (Superficial LP): key for mucosal wave; site of Reinke's edema.
- Vocal ligament: formed by Intermediate and Deep Lamina Propria.
- RLN innervates most intrinsic muscles; SLN (External branch) innervates Cricothyroid.
- Cricothyroid tenses folds, ↑ pitch; Vocalis muscle forms the fold's body.
- Voice production relies on Myoelastic-Aerodynamic theory & Bernoulli effect.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

