LFS Basics - Vocal Framework Fixes
- Laryngeal Framework Surgery (LFS): Surgical procedures that adjust the laryngeal cartilages (thyroid, cricoid, arytenoids) to alter vocal fold position, length, or tension, aiming to improve voice quality without direct surgery on the vocal folds themselves.
- Primary Goals:
- Medialization (e.g., for vocal fold paralysis)
- Lateralization
- Shortening/Relaxation (e.g., for pitch lowering)
- Lengthening/Tensioning (e.g., for pitch raising)
- General Indications:
- Unilateral vocal fold paralysis (UVFP)
- Vocal fold atrophy/bowing
- Sulcus vocalis
- Glottic insufficiency
- Pre-operative Assessment: Crucial; involves laryngoscopy, stroboscopy, acoustic/aerodynamic analysis, and patient's vocal needs.
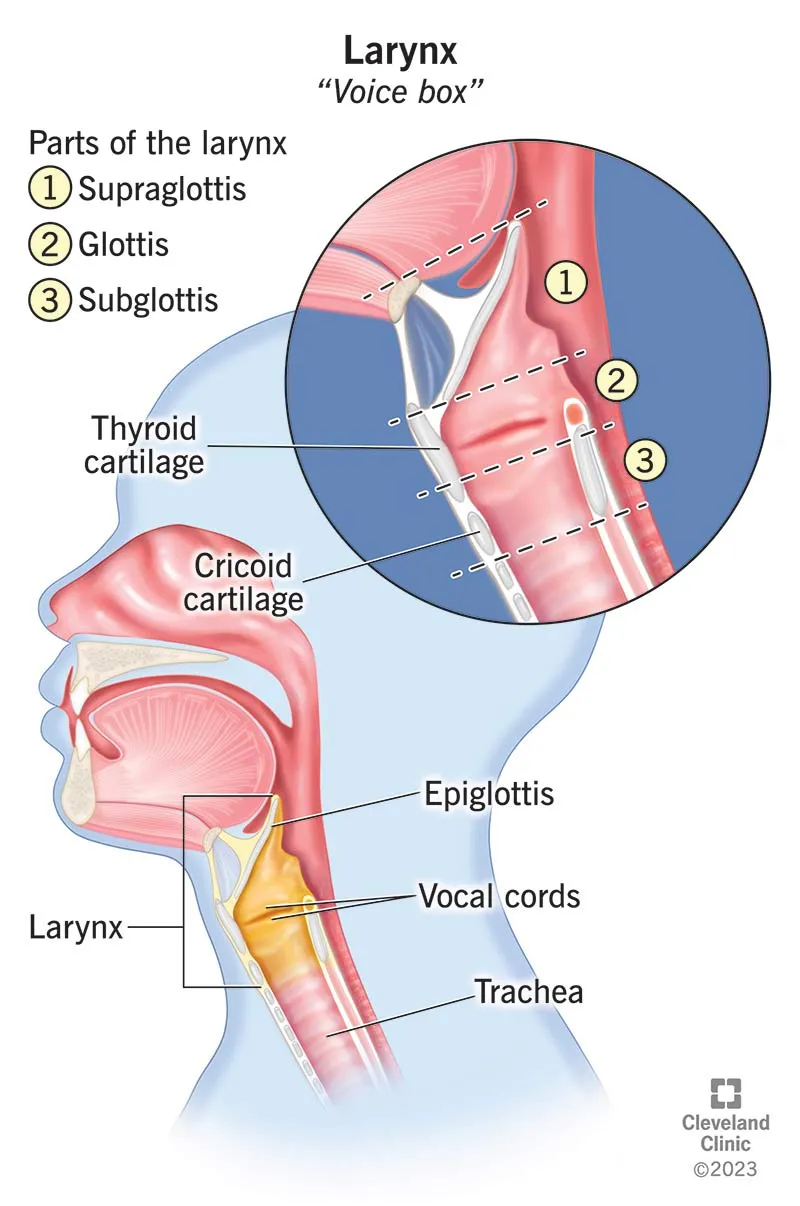
⭐ Most LFS procedures are performed under local anesthesia with sedation, enabling intra-operative voice monitoring to fine-tune the surgical outcome immediately.
Thyroplasty Types - Isshiki's Innovations
Isshiki described four thyroplasty types to alter vocal cord position/tension without mucosal surgery.
| Type | Procedure | Effect on Cord | Key Indication(s) | Material |
|---|---|---|---|---|
| I | Medialization | Adducts (medial shift) | UVCP, Glottic Insufficiency | Silastic, Gore-Tex |
| II | Lateralization | Abducts (lateral shift) | Bilat. Abductor Paralysis, Airway Obstruction, Adductor SD | Suture, Bone |
| III | Shortening | Relaxes (↓ pitch) | Pubophonia, High pitch | Cartilage flap |
| IV | Lengthening | Tensions (↑ pitch) | Androphonia, Bowing, Sulcus | Suture, Implant |
- Type I → Medialization
- Type II → Lateralization
- Type III → Relaxation (Shortening, ↓ pitch)
- Type IV → Tensioning (Lengthening, ↑ pitch)
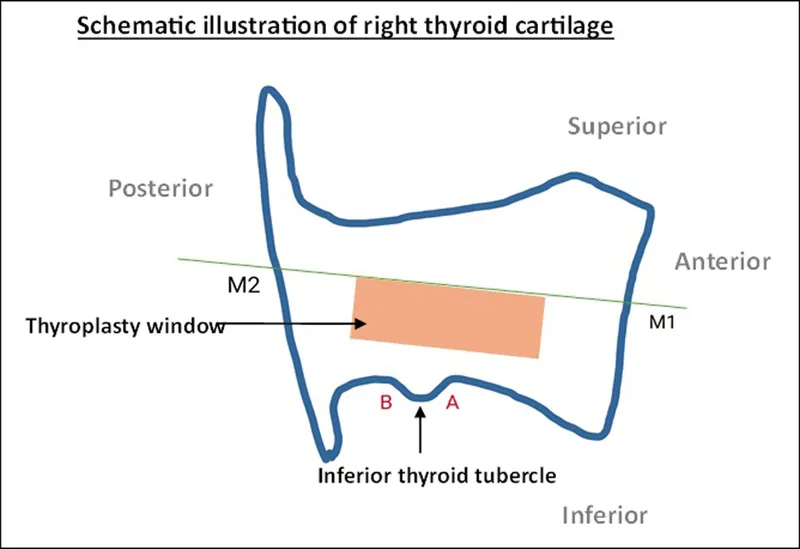
⭐ Type I thyroplasty is the most frequently performed, primarily to correct glottic incompetence in unilateral vocal cord paralysis.
Arytenoid & Other Adjustments - Cartilage Control
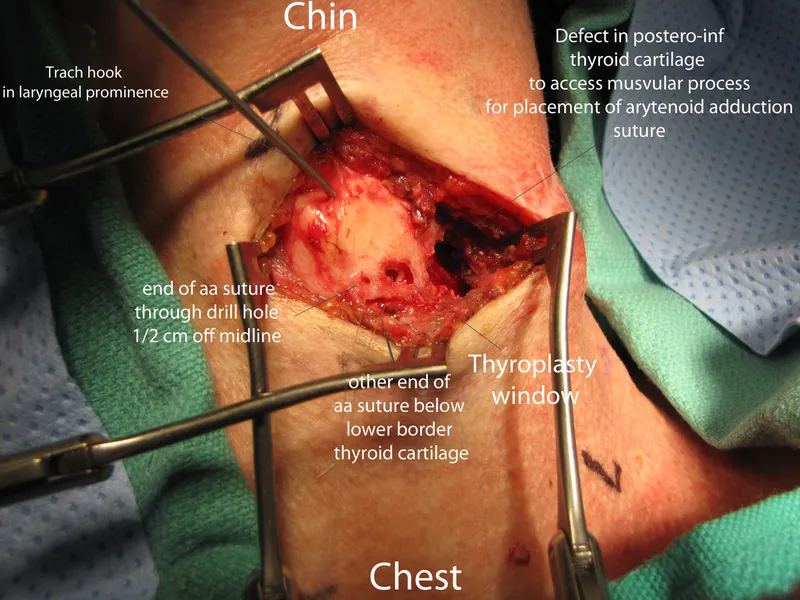
- Arytenoid Adduction (AA):
- Indication: Unilateral Vocal Fold Paralysis (UVFP) with large posterior glottic gap.
- Technique: Suture from muscular process of arytenoid to thyroid cartilage.
- Effect: Medializes & rotates arytenoid, closing posterior gap.
⭐ Often combined with Type I Thyroplasty for optimal voice in UVFP.
- Arytenopexy:
- Indication: Arytenoid subluxation/dislocation.
- Technique: Fixes arytenoid to cricoid or thyroid cartilage.
- Cricothyroid (CT) Subluxation/Approximation:
- Indication: To ↑ pitch (e.g., voice feminization, CT paralysis).
- Technique: Sutures approximate anterior cricoid & thyroid cartilages.
- Effect: Lengthens & tenses vocal folds.
- 📌 Mnemonic "A-A for P-G": Arytenoid Adduction for Posterior Gap.
LFS Hurdles & Healing - Complications & Care
- Early Complications:
- Hematoma, seroma, wound infection.
- Airway compromise (edema, spasm) - ⚠️ critical!
- Implant issues: malposition, early extrusion.
- Nerve injury (SLN/RLN) - uncommon.
- Late Complications:
- Granuloma formation.
- Persistent dysphonia, dysphagia.
- Implant migration/late extrusion.
- Laryngeal scarring/stenosis.
- Post-operative Care:
- Voice rest: Absolute (e.g., 3-7 days), then relative.
- Antibiotics, analgesics, anti-reflux therapy.
- Humidification, close airway watch.
- Speech therapy: essential for voice outcomes.
- Regular follow-up laryngoscopy.
- Outcomes:
- Improved voice quality (pitch, loudness, stability).
- Reduced vocal effort.
⭐ Airway compromise (e.g., laryngeal edema, hematoma) is a critical early post-LFS complication requiring vigilant monitoring and prompt management.
High‑Yield Points - ⚡ Biggest Takeaways
- Isshiki Thyroplasty: Type I (Medialization) for UVCP/glottic gap; Type II (Lateralization); Type III (Relaxation/pitch lowering); Type IV (Tensioning/pitch raising).
- Unilateral Vocal Cord Paralysis (UVCP) is a prime indication for Type I Thyroplasty.
- LFS is reversible, adjustable; performed under local anesthesia with intraoperative phonation.
- Arytenoid Adduction (AA) often augments Type I for large posterior glottic gaps.
- Goals: Improved voice quality and reduced aspiration.
- Type IV Thyroplasty is also termed Cricothyroid Subluxation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

