Stridor Basics - Noisy Breaths Intro
- Stridor: High-pitched sound from turbulent airflow in a narrowed airway.
- Types & Site:
- Inspiratory: Extrathoracic (e.g., supraglottis, glottis). Loudest on inspiration.
- Expiratory: Intrathoracic (e.g., trachea, bronchi). Loudest on expiration.
- Biphasic: Fixed lesion (glottis, subglottis, upper trachea). Heard in both phases.
- 📌 Mnemonic: Inspiratory = Extrathoracic. Expiratory = Intrathoracic. Biphasic = Fixed lesion.
illustrating stridor sound generation)
⭐ Laryngomalacia is the most common cause of chronic stridor in infants, typically inspiratory.
Stridor Causes - Airway Obstruction Agents
Stridor, a high-pitched sound from turbulent airflow, signals airway obstruction. Causes vary by age and anatomical site:
| Cause | Age of Onset | Stridor Type | Key Features |
|---|---|---|---|
| Laryngomalacia | Neonate/Infant | Inspiratory | Omega epiglottis, improves prone. 📌 Most common. |
| Vocal Cord Palsy | Neonate | Biphasic/Insp. | Weak cry, often iatrogenic (birth/cardiac surgery). |
| Subglottic Stenosis | Neonate/Infant | Biphasic | Hx of intubation, may have barking cough. |
| Croup (LTB) | 6m - 3y | Inspiratory | Barking cough, steeple sign (X-ray). |
| Epiglottitis | 2y - 6y | Inspiratory | Drooling, tripod, thumb sign (X-ray). ⚠️ Medical emergency. |
| Foreign Body Aspiration | Any age | Variable | Sudden onset, unilateral wheeze/↓ breath sounds. |
| Bacterial Tracheitis | < 6y | Inspiratory/Biphasic | Toxic, purulent secretions, often follows URI. |
⭐ Laryngomalacia is the most common cause of chronic stridor in infants, typically presenting with inspiratory stridor that worsens in supine position or with agitation, and improves when prone or calm.
Clinical Clues - Spotting Stridor Signs
- History:
- Onset: Acute vs. Chronic? Duration?
- Cry: Muffled, weak, aphonia?
- Feeding: Difficulty, choking?
- Symptoms: Fever, barking cough, cyanosis?
- Examination:
- Vitals: RR ↑, SpO2 < 92%?
- Work of Breathing: Nasal flaring, retractions (suprasternal, intercostal).
- Auscultation: Stridor type (inspiratory/expiratory/biphasic), air entry.
- Red Flags: Tripod, drooling, altered sensorium, severe distress. 📌 ABCDE.
⭐ Laryngomalacia: most common cause of chronic stridor in infants; inspiratory, worsens with agitation/feeding.
Diagnostic Tools - Peeking Inside Airways
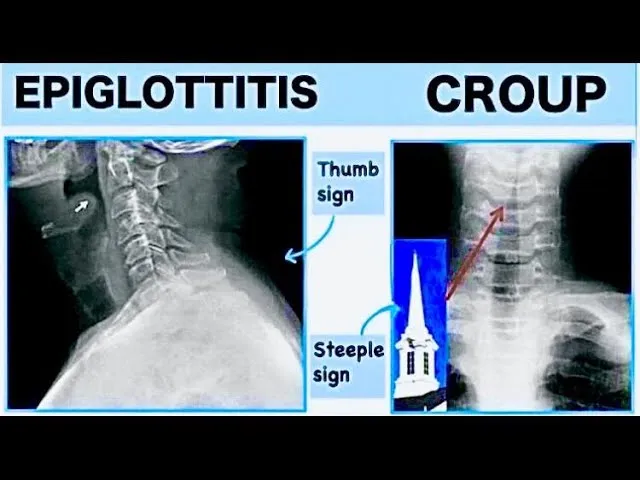
- Plain X-rays (Neck AP/Lat, Chest): Initial screen.
- Steeple sign (Croup)
- Thumb sign (Epiglottitis)
- Radio-opaque foreign body
- Endoscopy (Flexible/Rigid Laryngoscopy & Bronchoscopy):
- Gold standard for direct visualization, biopsy, or foreign body removal.
- Indications: persistent/severe stridor, suspected foreign body.
- Other Modalities:
- CT/MRI: Complex cases, suspected masses, extrinsic compression.
- Barium Swallow: Suspected vascular rings/slings.
⭐ Flexible fiberoptic laryngoscopy (FFL) can often be performed in an awake child in clinic to diagnose laryngomalacia.
Treatment Tactics - Clearing Tiny Tunnels
- General: ABCDE, O2, positioning, minimal disturbance.
- Specifics:
- Laryngomalacia: Conservative; rarely surgery.
- Croup: Dexamethasone 0.6 mg/kg, nebulized epinephrine. 📌 S.E.O (Steroids, Epinephrine, Oxygen).
- Epiglottitis: Secure airway (often intubation), IV antibiotics (e.g., Ceftriaxone).
- Foreign Body: Heimlich maneuver; rigid bronchoscopic removal.
- Subglottic Stenosis: Observation; endoscopic dilation; laryngotracheal reconstruction.
⭐ For croup, a single dose of dexamethasone 0.6 mg/kg (max 10-12 mg) is effective; nebulized budesonide is an alternative.
High‑Yield Points - ⚡ Biggest Takeaways
- Laryngomalacia: Most common cause of chronic infantile stridor; typically inspiratory.
- Stridor type: Inspiratory (supraglottic/glottic), Expiratory (intrathoracic), Biphasic (subglottic/tracheal).
- Croup: Barking cough, hoarseness, steeple sign on X-ray; primarily viral.
- Acute Epiglottitis: Tripod position, drooling, dysphagia, thumb sign on X-ray; bacterial.
- Foreign Body Aspiration: Sudden onset stridor/cough; consider unilateral wheeze.
- Flexible laryngoscopy: Key for diagnosis of persistent or atypical stridor_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

