Pediatric Sinusitis - Little Noses, Big Woes
- Inflammation of paranasal sinuses in children < 15 yrs.
- Unique Aspects:
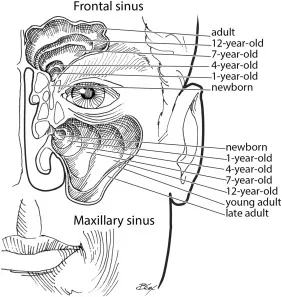
- Ethmoid & maxillary sinuses present at birth; sphenoid by 5 yrs, frontal by 7-8 yrs.
- Immature immune system.
- Shorter, wider Eustachian tubes (↑risk of AOM co-occurrence).
- Pathogens: Viral (most common); S. pneumoniae, H. influenzae, M. catarrhalis (bacterial).
- Predisposing Factors: URI, allergic rhinitis, adenoid hypertrophy, GORD, ciliary dyskinesia, immunodeficiency, daycare.
⭐ Recurrent acute rhinosinusitis (RARS) is defined as ≥ 4 episodes/year with symptom resolution between episodes.
Pediatric Sinusitis - Symptom Spotting & Timelines
- Key Persistent Symptoms (>10 days without improvement):
- Nasal discharge (any quality)
- Cough (daytime and/or nighttime)
- Severe Onset Symptoms (Bacterial Indication):
- Fever ≥39°C (concurrent)
- Purulent nasal discharge
- For ≥3 consecutive days
- Other Common Signs:
- Younger children: Irritability, poor feeding.
- Older children: Facial pain/pressure, headache, halitosis.
- Temporal Classification:
- Acute Rhinosinusitis (ARS): Symptoms <4 weeks, full resolution.
- Subacute Rhinosinusitis: 4-12 weeks, full resolution.
- Chronic Rhinosinusitis (CRS): Symptoms ≥12 weeks, no full resolution.
- Recurrent Acute Rhinosinusitis (RARS): ≥4 episodes/year, with interim resolution.
⭐ Viral URI is the most common predisposing factor for acute bacterial sinusitis in children.
Pediatric Sinusitis - Diagnostic Clues Unveiled
- Primarily clinical diagnosis based on specific criteria:
- Persistent illness: Nasal discharge (any type) AND/OR daytime cough for >10 days without improvement.
- Severe onset: Concurrent fever ≥39°C AND purulent nasal discharge for at least 3-4 consecutive days.
- Worsening course ("double sickening"): New onset fever, headache, or ↑ nasal discharge after initial improvement.
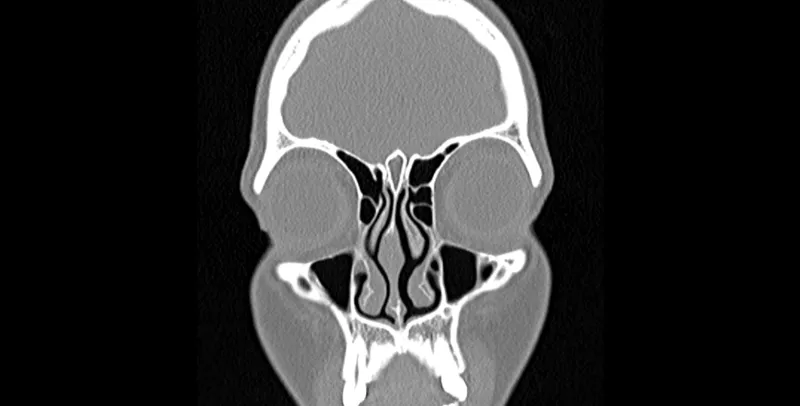
- Imaging (CT scan preferred over X-ray):
- Indicated for suspected orbital or intracranial complications.
- Evaluation of chronic or recurrent sinusitis unresponsive to medical therapy.
- Pre-operative planning for functional endoscopic sinus surgery (FESS).
- Nasal endoscopy: Useful to visualize purulent discharge from middle meatus, polyps, or anatomical obstruction.
⭐ CT scan is the gold standard imaging modality for assessing complicated or chronic pediatric sinusitis and prior to surgical intervention.
Pediatric Sinusitis - Treatment Blueprints
- Acute Bacterial Rhinosinusitis (ABRS):
- First-line: Amoxicillin or Amoxicillin-clavulanate (90 mg/kg/day amoxicillin component). Duration: 10-14 days.
- Severe/No response (48-72h): High-dose Amox-Clav, IV Cephalosporins (e.g., Ceftriaxone).
- Adjunctive Therapy:
- Nasal saline irrigation.
- Intranasal corticosteroids (especially if allergic component).
- Analgesics/antipyretics.
- Chronic Rhinosinusitis (CRS) / Recurrent ARS:
- Medical: Prolonged antibiotics (3-6 weeks), nasal steroids, saline irrigation.
- Surgical:
- Adenoidectomy (first-line for children <6 years or with significant adenoid hypertrophy).
- Functional Endoscopic Sinus Surgery (FESS) for failed medical/adenoidectomy or older children.
⭐ Adenoidectomy is often the first-line surgical treatment for chronic rhinosinusitis in children <6 years, especially with adenoid hypertrophy, before considering FESS.
Pediatric Sinusitis - Complication Watchlist
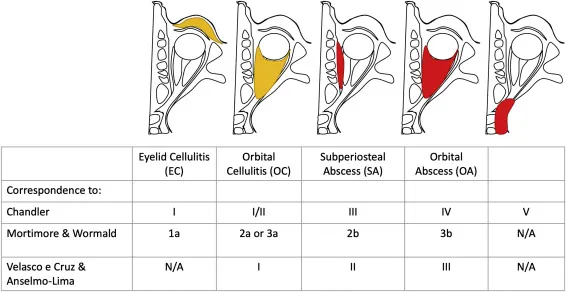
- Orbital (Chandler Classification):
- Group I: Preseptal cellulitis (Inflammatory edema)
- Group II: Orbital cellulitis
- Group III: Subperiosteal abscess
- Group IV: Orbital abscess
- Group V: Cavernous sinus thrombosis
- Intracranial:
- Meningitis
- Epidural abscess
- Subdural empyema
- Brain abscess
- Dural sinus thrombosis
- Bony: Osteomyelitis (Pott's puffy tumor - frontal sinus)
⭐ Preseptal cellulitis is the most common orbital complication of acute sinusitis in children. Urgent ophthalmology & ENT consult if suspected orbital/intracranial spread.
High‑Yield Points - ⚡ Biggest Takeaways
- Viral URIs are the primary trigger for acute bacterial sinusitis in children.
- Maxillary and ethmoid sinuses are most commonly involved due to their early development.
- Diagnosis: Persistent symptoms >10 days, severe onset, or biphasic (worsening) illness.
- Key pathogens: Streptococcus pneumoniae, non-typable Haemophilus influenzae, Moraxella catarrhalis.
- First-line antibiotic: Amoxicillin or Amoxicillin-clavulanate.
- Orbital complications like cellulitis or abscess are the most serious.
- Chronic pediatric sinusitis is defined by symptoms lasting >12 weeks.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more