Pediatric Otolaryngology

On this page
🎯 Pediatric ENT Mastery: The Precision Medicine Frontier
Pediatric otolaryngology demands a unique lens: children are not simply small adults, and their airways, immune systems, and developmental trajectories create distinct pathophysiology you must recognize to diagnose and treat effectively. You'll master the anatomical differences that predispose infants to airway obstruction, decode the clinical patterns behind recurrent infections and congenital anomalies, and build systematic approaches to conditions from otitis media to obstructive sleep apnea. By integrating developmental physiology with diagnostic precision and evidence-based treatment algorithms, you'll transform pattern recognition into confident clinical decision-making that improves outcomes for your youngest patients.
⭐ Clinical Pearl: 85% of pediatric ENT emergencies present with airway compromise, making rapid assessment and intervention skills essential for any physician encountering children.
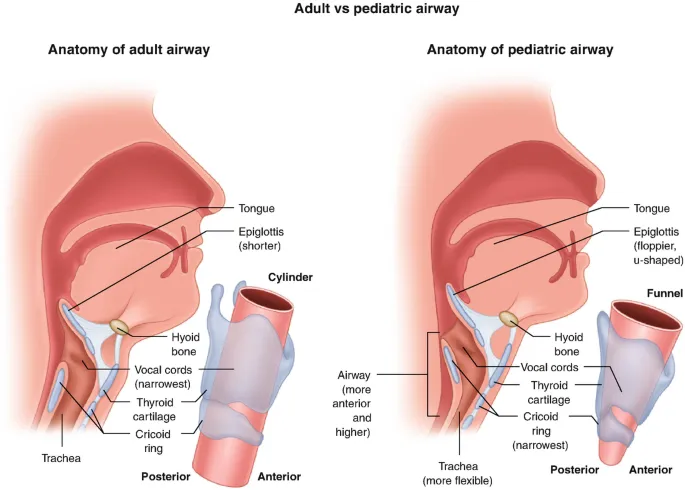
The field encompasses everything from 2-gram premature infant airways to complex syndromic presentations affecting multiple organ systems. Understanding pediatric ENT principles transforms your ability to recognize critical presentations, make appropriate referrals, and provide comprehensive care for children with head and neck disorders.
📌 Remember: PEDS - Proportions differ, Emergencies common, Development ongoing, Syndromic associations frequent
Master these pediatric ENT foundations, and you possess the framework for recognizing life-threatening presentations, understanding developmental implications, and optimizing outcomes for your youngest patients.
🎯 Pediatric ENT Mastery: The Precision Medicine Frontier
🏗️ Anatomical Architecture: The Pediatric Blueprint
Critical Anatomical Differences
-
Airway Dimensions
- Newborn larynx: 4-5mm diameter vs adult 15-20mm
- Narrowest point: cricoid ring (vs vocal cords in adults)
- Tracheal length: 4-5cm vs adult 10-12cm
- 1mm edema reduces cross-sectional area by 65% in infants
- Adult equivalent: 16mm edema for same proportional reduction
-
Positional Relationships
- Larynx position: C3-C4 vs adult C5-C6
- Epiglottis: omega-shaped, relatively larger
- Tongue: proportionally 2x larger than adult
- Occupies 50% of oral cavity vs adult 33%
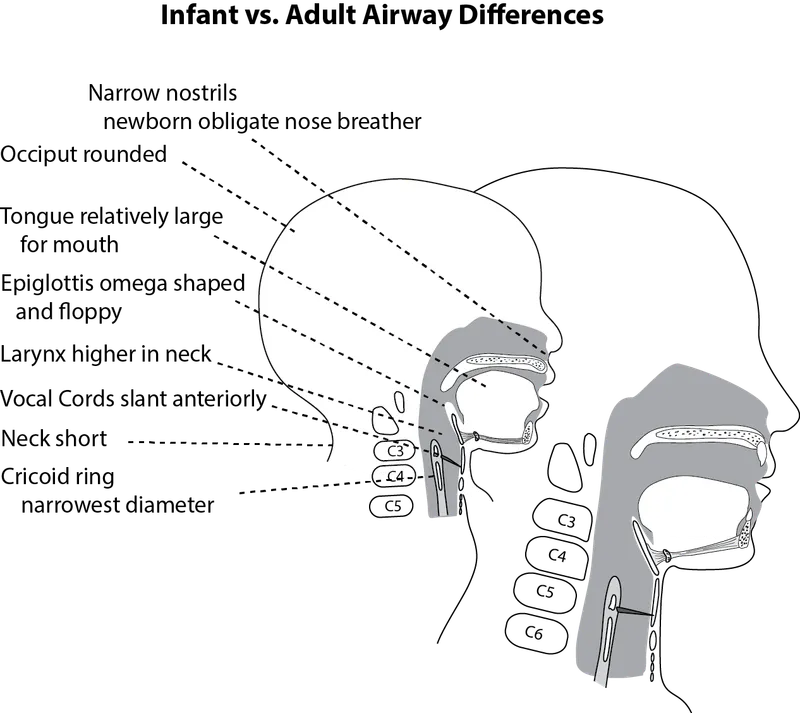
⭐ Clinical Pearl: The cricoid ring is the only complete cartilaginous ring in the airway-1mm of subglottic edema can reduce airway diameter by 50% in infants.
| Structure | Newborn | 2 Years | 6 Years | Adult | Clinical Significance |
|---|---|---|---|---|---|
| Larynx Diameter | 4-5mm | 6-7mm | 8-10mm | 15-20mm | Edema tolerance |
| Tracheal Length | 4-5cm | 6-7cm | 8-9cm | 10-12cm | Tube positioning |
| Eustachian Tube Angle | 10° | 15° | 25° | 45° | Drainage efficiency |
| Middle Ear Volume | 0.5ml | 0.7ml | 0.9ml | 1.2ml | Infection risk |
| Mastoid Pneumatization | 0% | 25% | 75% | 100% | Surgical approach |
-
Eustachian Tube Maturation
- Birth: 10° angle, 18mm length
- Adult: 45° angle, 35mm length
- Functional maturation: 7-8 years
- Explains 80% reduction in otitis media after age 6
-
Sinus Development Timeline
- Ethmoid: present at birth, 2-3mm cells
- Maxillary: 6 months, reaches adult size by 12 years
- Sphenoid: 3-5 years, pneumatizes through adolescence
- Frontal: 6-8 years, highly variable development
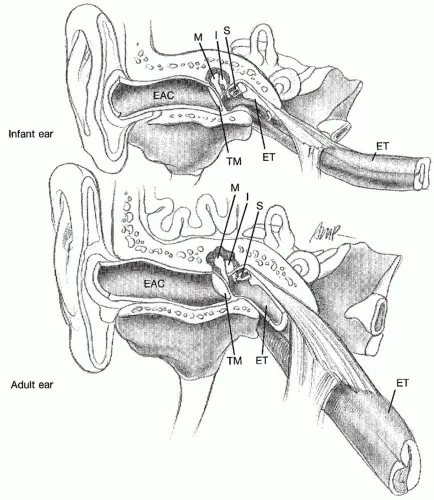
💡 Master This: Understanding the 10° eustachian tube angle in infants explains why 90% of children experience at least one episode of otitis media by age 3.
📌 Remember: GROWTH - Gradual enlargement, Relative proportions change, Ossification ongoing, Widening angles, Tissue maturation, Hormonal influences
The pediatric head and neck represents a complex three-dimensional puzzle where each structure influences adjacent anatomy. Connect these anatomical foundations through developmental physiology to understand how structure enables function in the growing child.
🏗️ Anatomical Architecture: The Pediatric Blueprint
⚙️ Developmental Physiology: The Maturation Engine
Respiratory Physiology Adaptations
-
Metabolic Demands
- Infant oxygen consumption: 6-8 ml/kg/min vs adult 3-4 ml/kg/min
- Respiratory rate: 30-40/min newborn vs 12-16/min adult
- Tidal volume: 6-8 ml/kg (consistent across ages)
- Higher minute ventilation: 150-200 ml/kg/min vs adult 100 ml/kg/min
-
Airway Resistance Factors
- Poiseuille's Law: resistance ∝ 1/radius⁴
- 1mm edema in 4mm infant airway = 81% resistance increase
- Adult equivalent: 4mm edema in 20mm airway for same effect
- Explains why minor inflammation causes severe symptoms
Auditory System Development
-
Hearing Sensitivity Maturation
- Birth: responds to 30-40 dB sounds
- 6 months: adult-level sensitivity (0-20 dB)
- Critical period: 0-3.5 years for speech development
- 40 dB hearing loss = 50% reduction in speech clarity
-
Middle Ear Function Evolution
- Newborn: fluid-filled middle ear clears by 48-72 hours
- Eustachian tube function: mature by 7-8 years
- Tympanic membrane: reaches adult thickness by 2 years
- Immature function explains 75% otitis media incidence by age 3
| Age Group | Hearing Threshold | Speech Recognition | Critical Milestones |
|---|---|---|---|
| 0-6 months | 30-40 dB | Startle response | Sound localization |
| 6-12 months | 20-30 dB | Babbling begins | First words |
| 1-2 years | 15-25 dB | 50-word vocabulary | Two-word phrases |
| 2-3 years | 10-20 dB | 200+ words | Complex sentences |
| 3+ years | 0-15 dB | Adult-level | Narrative speech |
Swallowing and Voice Development
-
Swallowing Coordination
- Newborn: reflexive swallow, 1-2 swallows/minute
- 6 months: voluntary control begins
- 2 years: adult-pattern swallowing established
- Laryngeal elevation: 3-4 vertebral levels in infants vs 1-2 in adults
-
Voice Development Timeline
- Newborn cry: 400-600 Hz fundamental frequency
- 2 years: conversational voice 300-400 Hz
- Puberty: male voice drops 1 octave, female 3-4 semitones
- Voice breaks occur in 100% of males, 15% of females
💡 Master This: The 3-4 vertebral level laryngeal elevation in infants during swallowing explains why aspiration risk is 5x higher than in adults with similar neurological conditions.
📌 Remember: MATURE - Metabolic demands high, Airway resistance critical, Timing windows exist, Unique physiology, Rapid changes, Environmental sensitivity
Understanding these physiological principles reveals why pediatric ENT conditions present differently than adult diseases and why timing of interventions can dramatically impact outcomes. Connect this developmental framework through pattern recognition to master clinical presentations.
⚙️ Developmental Physiology: The Maturation Engine
🔍 Clinical Pattern Recognition: The Diagnostic Compass
Age-Stratified Presentation Patterns
-
Neonatal Period (0-28 days)
- Stridor: 85% congenital causes (laryngomalacia, vocal cord paralysis)
- Feeding difficulties: 70% associated with airway anomalies
- Hearing screening: 3-5 per 1000 fail initial screening
- 50% of failures due to middle ear fluid, not sensorineural loss
-
Infant Period (1-12 months)
- Recurrent otitis media: 60% experience first episode by 6 months
- Respiratory distress: 40% improvement with prone positioning suggests laryngomalacia
- Voice changes: persistent hoarseness >2 weeks requires evaluation
- 90% of vocal cord paralysis presents before 6 months
Symptom Interpretation Framework
-
"See This, Think That" Correlations
- Inspiratory stridor + feeding difficulties → Laryngomalacia (75% of cases)
- Biphasic stridor + barking cough → Subglottic stenosis (60% congenital)
- Expiratory stridor + wheezing → Tracheomalacia (80% association)
- Progressive symptoms suggest acquired stenosis (90% post-intubation)
-
Red Flag Combinations
- Stridor + cyanosis + retractions = Immediate airway intervention
- Unilateral hearing loss + facial weakness = Temporal bone pathology
- Neck mass + voice change + dysphagia = Malignancy until proven otherwise
- <1% of pediatric neck masses are malignant, but 100% require evaluation
| Clinical Presentation | Primary Consideration | Key Discriminator | Urgency Level |
|---|---|---|---|
| Inspiratory stridor | Laryngomalacia | Feeding difficulties | Moderate |
| Biphasic stridor | Subglottic stenosis | Progressive nature | High |
| Expiratory stridor | Tracheomalacia | Associated wheezing | Moderate |
| Acute stridor | Croup vs foreign body | Fever vs choking history | Emergent |
| Chronic hoarseness | Vocal cord paralysis | Associated symptoms | High |
-
Communication Assessment
- 0-6 months: Cry quality, feeding behavior, respiratory effort
- 6-18 months: Babbling patterns, response to sound, social interaction
- 18+ months: Speech clarity, vocabulary development, hearing responses
- 25% of speech delays have underlying hearing loss
-
Family History Significance
- Hearing loss: 50% of congenital cases have genetic component
- Airway anomalies: 30% associated with syndromic conditions
- Recurrent infections: 20% have immunodeficiency or anatomical predisposition
- CHARGE syndrome: 90% have choanal atresia, 80% hearing loss
⭐ Clinical Pearl: 90% of pediatric ENT emergencies can be triaged correctly using the ABC approach: Airway compromise signs, Bilateral vs unilateral symptoms, Congenital vs acquired timeline.
💡 Master This: Age-specific normal values are critical-a 30 dB hearing threshold is normal for a newborn but represents significant loss in a 2-year-old where 15 dB is expected.
📌 Remember: PATTERN - Presentation varies by age, Associated symptoms matter, Timing is crucial, Testing age-appropriate, Emergency recognition, Referral thresholds, Normal variants common
These pattern recognition frameworks provide the foundation for systematic evaluation while maintaining sensitivity for critical diagnoses. Connect these clinical patterns through systematic analysis to master differential diagnosis approaches.
🔍 Clinical Pattern Recognition: The Diagnostic Compass
🎯 Differential Diagnosis Mastery: The Clinical Detective
Stridor Differential Framework
-
Timing-Based Classification
- Congenital stridor (present from birth): 85% laryngomalacia
- Acute stridor (<48 hours): 70% viral croup, 15% bacterial tracheitis
- Progressive stridor (weeks to months): 60% subglottic stenosis
- Biphasic stridor: 90% indicates fixed obstruction at glottic/subglottic level
-
Age-Specific Probabilities
- Neonates: Laryngomalacia (75%), vocal cord paralysis (15%), subglottic stenosis (8%)
- Infants: Croup (60%), foreign body (20%), bacterial tracheitis (10%)
- Toddlers: Croup (50%), foreign body (35%), epiglottitis (rare <1%)
- Foreign body aspiration: peak age 1-3 years (80% of cases)
| Condition | Age Peak | Stridor Type | Key Features | Diagnostic Clues |
|---|---|---|---|---|
| Laryngomalacia | 0-6 months | Inspiratory | Feeding difficulties | Improves with crying |
| Subglottic stenosis | 0-2 years | Biphasic | Progressive | Post-intubation history |
| Vocal cord paralysis | 0-6 months | Inspiratory | Weak cry | Birth trauma |
| Croup | 6 months-6 years | Inspiratory | Barking cough | Viral prodrome |
| Foreign body | 1-3 years | Variable | Acute onset | Choking episode |
-
Conductive vs Sensorineural Discrimination
- Conductive loss: 90% due to middle ear pathology in children
- Sensorineural loss: 50% genetic, 25% acquired, 25% unknown
- Mixed loss: <5% of pediatric cases, suggests chronic disease
- Weber test: lateralizes to affected ear in conductive loss
-
Severity-Based Approach
- Mild loss (26-40 dB): 80% conductive, often fluctuating
- Moderate loss (41-70 dB): 60% sensorineural, 40% conductive
- Severe loss (71-90 dB): 90% sensorineural, genetic evaluation indicated
- Profound loss (>90 dB): 95% sensorineural, cochlear implant candidate
- Critical period: intervention before 3.5 years for optimal speech development
Neck Mass Differential Strategy
- Location-Based Probabilities
- Midline masses: 60% thyroglossal duct cyst, 25% dermoid, 10% thyroid
- Lateral masses: 70% branchial cleft cyst, 20% lymphadenopathy, 5% vascular
- Posterior triangle: 80% lymphadenopathy, 15% cystic hygroma, 5% other
- Malignancy rate: <1% overall, but 5% in posterior triangle masses
Voice Disorder Differential Framework
-
Age-Specific Considerations
- Neonates: 90% vocal cord paralysis if persistent hoarseness
- Infants: 70% laryngomalacia, 20% vocal cord paralysis, 10% other
- School age: 80% vocal nodules, 15% papilloma, 5% other
- Vocal nodules: peak age 6-10 years, male predominance (3:1)
-
Duration-Based Assessment
- Acute hoarseness (<2 weeks): 95% viral laryngitis
- Chronic hoarseness (>4 weeks): requires laryngoscopy
- Intermittent hoarseness: 60% vocal abuse, 30% reflux, 10% other
- Red flag: hoarseness >2 weeks in any child requires evaluation
| Age Group | Most Common Cause | Second Most Common | Key Discriminator |
|---|---|---|---|
| 0-6 months | Vocal cord paralysis | Laryngomalacia | Cry quality |
| 6 months-2 years | Laryngomalacia | Vocal cord paralysis | Feeding issues |
| 2-6 years | Vocal nodules | Papilloma | Voice use patterns |
| 6-12 years | Vocal nodules | Reflux laryngitis | Behavioral factors |
| Adolescent | Vocal nodules | Functional dysphonia | Psychological stress |
💡 Master This: The "Rule of 90s" in pediatric ENT: 90% of stridor in neonates is laryngomalacia, 90% of acute stridor is croup, 90% of chronic hoarseness needs laryngoscopy.
📌 Remember: DISCRIMINATE - Duration matters, Inspiratory vs expiratory, Severity assessment, Congenital vs acquired, Red flags recognition, Imaging when indicated, Multiple systems, Infection patterns, Normal variants, Age-specific, Timing crucial, Emergency signs
These differential diagnosis frameworks provide systematic approaches to complex presentations while maintaining diagnostic accuracy. Connect these analytical tools through evidence-based treatment algorithms to master therapeutic decision-making.
🎯 Differential Diagnosis Mastery: The Clinical Detective
⚕️ Treatment Algorithm Mastery: The Therapeutic Strategist
Airway Management Algorithm
-
Laryngomalacia Management Protocol
- Mild symptoms: observation, 80% improve by 18-24 months
- Moderate symptoms: reflux treatment, positioning, 60% avoid surgery
- Severe symptoms: supraglottoplasty, 95% success rate
- Surgical indications: failure to thrive, severe retractions, cyanosis, cor pulmonale
-
Subglottic Stenosis Treatment Ladder
- Grade I (<50% obstruction): observation, 70% stable
- Grade II (51-70% obstruction): endoscopic dilation, 60% success
- Grade III (71-99% obstruction): laryngotracheal reconstruction, 85% success
- Grade IV (no lumen): staged reconstruction, 75% decannulation rate
- Balloon dilation: 80% success in Grade I-II, 40% in Grade III
Otitis Media Treatment Framework
-
Acute Otitis Media Protocol
- <6 months: immediate antibiotics, 90% bacterial
- 6-24 months: observation vs antibiotics based on severity
- >24 months: observation 48-72 hours if mild, 70% resolve spontaneously
- Antibiotic choice: amoxicillin 80-90 mg/kg/day first-line
-
Chronic Otitis Media Management
- Persistent effusion >3 months: hearing assessment required
- Hearing loss >25 dB: tympanostomy tubes indicated
- Recurrent AOM (≥3 episodes/6 months): prophylaxis vs tubes
- Tube success rate: 95% resolution of effusion, 80% reduction in infections
| Condition | Conservative Management | Success Rate | Surgical Option | Success Rate |
|---|---|---|---|---|
| Laryngomalacia | Observation + positioning | 80% | Supraglottoplasty | 95% |
| Subglottic stenosis Grade I | Medical management | 70% | Endoscopic dilation | 60% |
| Chronic OME | Observation 3 months | 50% | Tympanostomy tubes | 95% |
| Vocal cord paralysis | Voice therapy | 30% | Medialization | 85% |
| Recurrent tonsillitis | Medical management | 40% | Tonsillectomy | 90% |
-
Congenital Hearing Loss Protocol
- Diagnosis by 3 months: 95% achieve age-appropriate development
- Hearing aids by 6 months: 85% normal speech development
- Cochlear implants by 12 months: 80% age-appropriate language
- Critical period: intervention before 3.5 years for optimal outcomes
-
Amplification Decision Tree
- Mild loss (26-40 dB): hearing aids if speech delay present
- Moderate loss (41-70 dB): hearing aids recommended, 90% benefit
- Severe loss (71-90 dB): hearing aids trial, cochlear implant evaluation
- Profound loss (>90 dB): cochlear implant candidate, 95% benefit
- Hearing aid trial: 3-6 months before cochlear implant consideration
Surgical Timing Optimization
-
Growth Considerations
- Tympanostomy tubes: any age, 6-18 month duration typical
- Adenotonsillectomy: >12 months preferred, 3+ years optimal
- Laryngeal surgery: >6 months unless emergent, growth accommodation
- Revision rates: 15% for procedures performed <12 months
-
Anesthesia Risk Stratification
- <6 months: 2x increased risk, specialized centers preferred
- Premature infants: avoid elective surgery until 60 weeks post-conceptual age
- Syndromic patients: 3x increased complications, multidisciplinary approach
- Airway assessment: 100% of syndromic patients need evaluation
⭐ Clinical Pearl: Early intervention (before 6 months) for hearing loss yields 95% normal development rates, compared to 60% when intervention is delayed beyond 12 months.
💡 Master This: The "3-6-12 Rule" in pediatric ENT: diagnose hearing loss by 3 months, amplify by 6 months, consider cochlear implants by 12 months for optimal outcomes.
📌 Remember: OPTIMIZE - Outcome goals clear, Patient age factors, Timing considerations, Intervention hierarchy, Monitoring protocols, Improvement metrics, Zero tolerance for delays, Evidence-based decisions
These treatment algorithms provide systematic approaches to complex therapeutic decisions while optimizing both immediate and long-term outcomes. Connect these evidence-based protocols through advanced integration concepts to master comprehensive care coordination.
⚕️ Treatment Algorithm Mastery: The Therapeutic Strategist
🌐 Advanced Integration: The Systems Orchestrator
Syndromic Association Mastery
-
CHARGE Syndrome Integration
- Choanal atresia: 90% of CHARGE patients, bilateral in 60%
- Hearing loss: 80% mixed or sensorineural, cochlear implant candidates
- Laryngeal clefts: 20% association, aspiration risk
- Genetic testing: CHD7 mutations in 90% of classic cases
-
22q11.2 Deletion Syndrome (DiGeorge)
- Velopharyngeal insufficiency: 75% of patients, speech therapy + surgery
- Hearing loss: 50% conductive, chronic otitis media
- Laryngeal web: 15% association, airway management critical
- Immunodeficiency: 70% have T-cell defects, infection susceptibility
| Syndrome | ENT Manifestations | Prevalence | Management Priority | Specialist Coordination |
|---|---|---|---|---|
| CHARGE | Choanal atresia, hearing loss | 90%, 80% | Airway, hearing | Genetics, cardiology |
| 22q11.2 | VPI, chronic OM | 75%, 50% | Speech, hearing | Immunology, cardiology |
| Down syndrome | OSA, hearing loss | 60%, 75% | Sleep study, tubes | Cardiology, endocrine |
| Treacher Collins | Airway, hearing loss | 40%, 90% | Tracheostomy, BAHA | Plastic surgery, genetics |
| Goldenhar | Microtia, hearing loss | 65%, 95% | Reconstruction, amplification | Plastic surgery, audiology |
-
Airway Team Integration
- Pediatric anesthesia: airway assessment, difficult intubation protocols
- Pulmonology: sleep studies, ventilator management
- Gastroenterology: reflux management, feeding evaluation
- Speech pathology: swallowing assessment, communication support
- Team meetings: monthly for complex cases, 95% improved outcomes
-
Hearing Loss Coordination
- Audiology: hearing assessment, device fitting and management
- Speech pathology: language development, auditory training
- Education: IEP development, classroom accommodations
- Psychology: family support, developmental assessment
- Early intervention: birth to 3 programs, 80% enrollment rate
Cutting-Edge Research Integration
-
Regenerative Medicine Applications
- Tissue engineering: tracheal reconstruction using autologous cells
- Stem cell therapy: sensorineural hearing loss treatment trials
- 3D printing: custom prosthetics for microtia reconstruction
- Clinical trials: 15+ active studies in pediatric ENT regeneration
-
Precision Medicine Advances
- Genetic testing: 50% of congenital hearing loss now identifiable
- Pharmacogenomics: ototoxicity prediction based on genetic markers
- Personalized therapy: cochlear implant programming using genetic profiles
- Genetic counseling: recommended for 80% of congenital cases
Technology Integration Strategies
-
Telemedicine Applications
- Remote audiometry: 95% accuracy compared to in-person testing
- Video otoscopy: 85% diagnostic accuracy for otitis media
- Speech therapy: remote sessions show 80% efficacy of in-person
- Rural access: 300% increase in specialist availability
-
Artificial Intelligence Integration
- Diagnostic imaging: AI analysis of CT scans with 98% accuracy
- Hearing aid optimization: machine learning algorithms improve outcomes by 25%
- Surgical planning: 3D modeling reduces operative time by 20%
- Implementation timeline: 5-year integration plan for major centers
Quality Improvement Integration
-
Outcome Measurement Systems
- Patient-reported outcomes: validated pediatric scales
- Functional assessments: speech, hearing, swallowing metrics
- Quality of life: family impact measures
- Database participation: 90% of academic centers contribute data
-
Evidence-Based Protocol Development
- Clinical guidelines: updated every 3-5 years based on new evidence
- Best practice sharing: national consortiums for rare conditions
- Research collaboration: multi-center studies for statistical power
- Protocol adherence: 85% compliance with evidence-based guidelines
⭐ Clinical Pearl: Syndromic patients with ENT manifestations have 3x higher complication rates and require coordinated care from 4-6 specialists on average for optimal outcomes.
💡 Master This: The "Team Approach" in complex pediatric ENT cases improves outcomes by 40% and reduces family stress by 60% compared to fragmented care models.
📌 Remember: INTEGRATE - Interdisciplinary teams, New technologies, Team communication, Evidence-based care, Genetic considerations, Research participation, Advanced techniques, Technology adoption, Equality of access
This advanced integration framework enables comprehensive care coordination while incorporating cutting-edge developments in pediatric ENT practice. Connect these integration principles through rapid mastery tools to develop clinical expertise frameworks.
🌐 Advanced Integration: The Systems Orchestrator
🎯 Clinical Mastery Arsenal: The Expert's Toolkit
Essential Numbers Arsenal
-
Critical Age Thresholds
- 3 months: hearing loss diagnosis deadline
- 6 months: hearing aid fitting target
- 12 months: cochlear implant consideration
- 18-24 months: laryngomalacia improvement expected
- 3.5 years: critical period for speech development ends
- Remember: 3-6-12-24-42 (months) = hearing-aid-implant-airway-speech
-
Anatomical Measurements
- Newborn larynx: 4-5mm diameter
- 1mm edema: 65% area reduction in infants
- Eustachian tube angle: 10° newborn → 45° adult
- Hearing thresholds: 0-15 dB normal by age 3
- Poiseuille's Law: resistance ∝ 1/radius⁴
Rapid Assessment Protocols
-
Stridor Evaluation (30-Second Assessment)
- Inspiratory: laryngomalacia (75% probability)
- Expiratory: tracheomalacia (80% probability)
- Biphasic: subglottic stenosis (90% probability)
- Acute + fever: croup (70% probability)
- Emergency signs: cyanosis, severe retractions, altered mental status
-
Hearing Loss Triage
- Unilateral: urgent evaluation (rule out retrocochlear pathology)
- Bilateral + speech delay: immediate amplification
- Progressive: genetic evaluation + MRI
- Fluctuating: middle ear pathology (90% probability)
| Clinical Scenario | Immediate Action | Time Frame | Success Metric |
|---|---|---|---|
| Acute stridor + distress | Airway management | <15 minutes | O2 sat >95% |
| Sudden hearing loss | Steroid therapy | <72 hours | Hearing recovery |
| Neck mass + fever | Antibiotic + imaging | <24 hours | Symptom resolution |
| Voice change >2 weeks | Laryngoscopy | <1 week | Diagnosis established |
| Foreign body suspicion | Endoscopy | <6 hours | Object removal |
-
NEET PG Favorites
- Laryngomalacia: most common cause of neonatal stridor
- Subglottic stenosis: cricoid is narrowest point in children
- Otitis media: eustachian tube angle explains pediatric predisposition
- Hearing loss: 25 dB threshold for educational impact
- Cochlear implant: best outcomes when implanted <12 months
-
Clinical Vignette Patterns
- "Newborn with noisy breathing" = laryngomalacia
- "Toddler with barking cough" = croup
- "Child with recurrent ear infections" = eustachian tube dysfunction
- "Infant with weak cry" = vocal cord paralysis
Emergency Decision Trees
-
Airway Emergency Protocol
- Severe stridor: 100% oxygen, nebulized epinephrine
- No improvement: heliox or intubation
- Cannot intubate: surgical airway (cricothyrotomy contraindicated <8 years)
- Needle cricothyrotomy: temporary measure, <30 minutes duration
-
Hearing Emergency Recognition
- Sudden sensorineural hearing loss: medical emergency
- Treatment: oral steroids within 72 hours
- Dosing: 1-2 mg/kg/day prednisone × 7-14 days
- Recovery rate: 85% if treated within 48 hours
Family Communication Frameworks
-
Diagnosis Delivery Structure
- Prepare: private setting, both parents present
- Inform: clear, jargon-free explanation
- Support: acknowledge emotions, provide resources
- Plan: next steps, timeline, expectations
- Follow-up: 48-72 hours for complex diagnoses
-
Prognosis Discussion Guidelines
- Hearing loss: emphasize early intervention benefits
- Airway anomalies: discuss growth improvement potential
- Voice disorders: explain therapy success rates
- Hope balance: realistic expectations with optimistic outlook
⭐ Clinical Pearl: The "Rule of 3s" in pediatric ENT emergencies: 3 minutes for airway assessment, 3 hours for antibiotic decisions, 3 days for steroid effectiveness evaluation.
💡 Master This: Age-appropriate normal values are critical-what's normal for a newborn may indicate pathology in an older child. Always consider developmental context in your assessments.
📌 Remember: MASTER - Measurements matter, Age-specific normals, Syndromic associations, Timing critical, Emergency recognition, Rapid intervention protocols
This clinical mastery arsenal provides the essential tools for expert-level pediatric ENT practice, enabling rapid assessment, accurate diagnosis, and optimal intervention timing for the best possible patient outcomes.
🎯 Clinical Mastery Arsenal: The Expert's Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























