Decompression 101 - Nerve Under Pressure
- Definition: Surgical relief of pressure on facial nerve (CN VII) within its bony fallopian canal.
- Goal: Preserve/restore nerve function; prevent axonal degeneration & synkinesis.
- Mechanism: Unroofing the nerve by removing overlying bone.
- Key Indications:
- Bell's Palsy: >90% ENoG degeneration within 14 days & no voluntary EMG.
- Traumatic Injury: Temporal bone fracture, iatrogenic injury.
- Ramsay Hunt Syndrome: Severe, selected cases.
⭐ Facial palsy in acute otitis media/mastoiditis unresponsive to medical therapy (IV antibiotics, myringotomy) within 24-48h is an indication for decompression if no improvement is seen after these measures and mastoidectomy (if coalescent mastoiditis is present).
Facial Nerve Anatomy - The Critical Path
- Intracranial & Meatal: Brainstem to Internal Auditory Canal (IAC); travels with CN VIII.
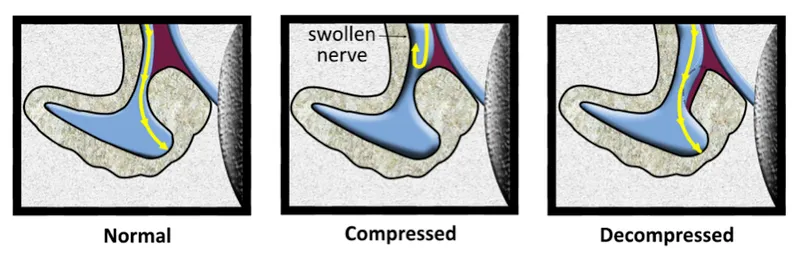
- Labyrinthine Segment:
- Narrowest part (~0.68 mm); contains geniculate ganglion (taste, parasympathetic fibers).
- Most vulnerable to compression (e.g., viral inflammation).
- Tympanic Segment:
- Horizontal course; superior to oval window, medial to incus.
- Bony Fallopian canal dehiscence common here (~50%), risk during surgery.
- Mastoid Segment:
- Vertical course; gives off nerve to stapedius, chorda tympani.
- Exits skull base at stylomastoid foramen.
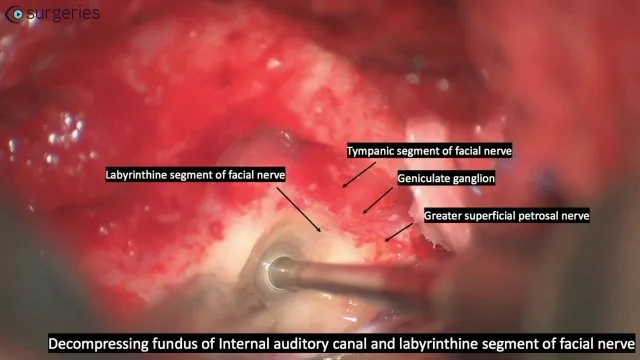
⭐ The labyrinthine segment is the most frequent site of compression in Bell's palsy and Ramsay Hunt syndrome due to its anatomically constricted bony canal, making it a key focus for surgical decompression when indicated.
Why Decompress? - Causes & Calls
- Causes:
- Bell's Palsy (Idiopathic)
- Trauma (e.g., temporal bone fracture)
- Infections (Ramsay Hunt Syndrome, AOM)
- Tumors (e.g., facial neuroma)
- Indications (Electrophysiologic Criteria):
- Bell's Palsy / Ramsay Hunt Syndrome:
- ENoG: >90-95% degeneration
- Timing: Within 14 days of onset
- EMG: No voluntary motor unit potentials (MUPs)
- Traumatic Facial Palsy:
- Immediate, complete paralysis with transection signs
- ENoG: >90% degeneration within 6 days post-injury
- Bell's Palsy / Ramsay Hunt Syndrome:
⭐ For Bell's Palsy, ENoG showing >90% degeneration (compared to normal side) within 14 days of onset strongly suggests considering decompression.
Surgical Strategies - Freeing the Nerve
- Goal: Relieve nerve pressure, promote recovery.
- Timing:
- Bell's: >90% ENoG degeneration (first 14 days), no EMG.
- Trauma: Immediate (transection); delayed (3-6 wks) if progressive/no improvement.
- Approaches:
- Transmastoid: Mastoid, tympanic segments.
- Middle Cranial Fossa (MCF): Labyrinthine segment, geniculate ganglion.
- Translabyrinthine: If no hearing.
- Extent: Guided by HRCT, ENoG/EMG. Decompress involved segments.
⭐ MCF approach is vital for labyrinthine segment/geniculate ganglion lesions, aiming to preserve hearing.
Outcomes & Pitfalls - The Recovery Road
- Recovery Influenced By:
- Pre-op nerve status (e.g., ENoG degeneration >90%).
- Etiology (Bell's palsy, iatrogenic/traumatic injury, tumor).
- Timing of decompression: Bell's <2-3 weeks; Trauma <72 hrs for acute, complete palsy.
- Assessment: House-Brackmann (HB I-VI) scale. Gradual improvement over 6-12 months.
- Common Pitfalls:
- Incomplete recovery (persistent weakness, HB ≥III).
- Synkinesis (aberrant reinnervation, e.g., eye closure with smiling).
- Sensorineural hearing loss (SNHL), vertigo.
- CSF leak, infection, altered taste/tear production.
⭐ Synkinesis is the most common long-term complication after severe facial nerve injury and subsequent regeneration, potentially managed with physiotherapy or botulinum toxin injections.
High‑Yield Points - ⚡ Biggest Takeaways
- Indications: Severe Bell's palsy (>90% ENoG degeneration within 14 days), traumatic facial palsy (immediate, >90% degeneration).
- Critical timing: Bell's palsy within 3 weeks (ideally 14 days); trauma ASAP.
- Surgical approaches: Transmastoid, Middle Cranial Fossa (MCF), Translabyrinthine.
- Most vulnerable segments: Labyrinthine segment, geniculate ganglion, tympanic segment.
- Goal: Relieve pressure on the nerve, improve blood supply, promote recovery.
- ENoG >90% degeneration is a key surgical indication.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

