Otology

On this page
🎯 Otology Mastery: The Precision Medicine of Hearing
Otology demands more than memorizing ear anatomy-it requires you to think like a diagnostic architect who can trace a patient's hearing loss or vertigo back through intricate pathophysiologic mechanisms, distinguish between overlapping presentations with surgical precision, and deploy evidence-based interventions that restore function and prevent complications. You'll master the frameworks that transform isolated symptoms into coherent diagnoses, connect otologic disease to systemic conditions, and build the pattern recognition skills that separate competent clinicians from true experts at the bedside.
The Otologic Foundation: Architectural Precision
The ear's three-compartment design enables sound transformation from mechanical waves to neural signals through 4 distinct energy conversions:
-
Outer Ear Mechanics
- Auricle amplifies frequencies 2000-5000 Hz by 10-15 dB
- External auditory canal resonates at 2700 Hz (quarter-wave resonator)
- Cerumen production: 1-2 mg daily with pH 4.0-5.0
-
Middle Ear Transformer
- Tympanic membrane area: 55 mm² vs stapes footplate 3.2 mm²
- Mechanical advantage ratio: 17:1 pressure amplification
- Ossicular chain lever arm ratio: 1.3:1 additional gain
- Total middle ear gain: 22-25 dB at optimal frequencies
-
Inner Ear Transduction
- Cochlear length: 35 mm with 2.75 turns
- Hair cell population: 15,500 inner + 12,000 outer cells
- Frequency mapping: 20 kHz (base) to 20 Hz (apex)
- Endolymphatic potential: +80 mV driving force
📌 Remember: COAT for middle ear transformer - Concentration (area ratio), Ossicular leverage, Amplification (25 dB), Transmission efficiency (99.9% at 1000 Hz)
Clinical Correlation Matrix
| Structure | Normal Function | Pathology | Clinical Impact | Diagnostic Threshold |
|---|---|---|---|---|
| TM | Sound transmission | Perforation | 25-40 dB CHL | >2mm significant |
| Ossicles | Mechanical coupling | Disruption | 40-60 dB CHL | >30 dB gap |
| Stapes | Oval window motion | Otosclerosis | 50-70 dB CHL | Carhart notch 2kHz |
| Cochlea | Neural transduction | SNHL | Variable loss | >25 dB abnormal |
| Vestibule | Balance function | Vertigo | Spatial disorientation | >20° VOR gain |
💡 Master This: The 500 Hz bone conduction threshold predicts stapedectomy success-thresholds better than 30 dB achieve 95% closure rates, while worse than 45 dB show only 60% success.
Understanding this otologic foundation unlocks the diagnostic logic behind every hearing complaint, from simple cerumen impaction causing 30 dB conductive loss to complex retrocochlear pathology producing asymmetric sensorineural hearing loss with rollover phenomenon.
🎯 Otology Mastery: The Precision Medicine of Hearing
🔬 Pathophysiology Powerhouse: Disease Mechanisms Decoded
Inflammatory Cascade Architecture
Middle ear inflammation follows predictable molecular pathways that determine clinical presentation and treatment response:
-
Acute Phase Response (0-72 hours)
- Cytokine release: IL-1β, TNF-α peak at 6-12 hours
- Vascular permeability increases 300-500%
- Neutrophil infiltration: 10,000-50,000 cells/μL
- Middle ear pressure: -200 to -400 mmH₂O
-
Chronic Inflammatory Remodeling (>3 months)
- Mucin gene upregulation: MUC5AC increases 10-fold
- Bone resorption markers: RANKL/OPG ratio increases 5-8x
- Fibroblast proliferation with Type III collagen deposition
- Ossicular erosion risk: 15% incus, 8% stapes, 3% malleus
📌 Remember: STEAM for chronic otitis media complications - Sensorineural loss, Tympanosclerosis, Erosion (ossicular), Adhesions, Mastoiditis progression
Mechanical Disruption Patterns
Ossicular chain pathology creates characteristic audiometric signatures that enable precise diagnosis:
| Pathology Type | Primary Site | Frequency Pattern | Air-Bone Gap | Acoustic Reflex |
|---|---|---|---|---|
| Malleus fixation | Anterior process | Low frequency | 20-30 dB | Present |
| Incus erosion | Long process | Flat loss | 40-50 dB | Absent |
| Stapes fixation | Footplate | Carhart notch | 50-60 dB | Absent |
| Chain disruption | I-S joint | High frequency | 45-65 dB | Absent |
| TM perforation | Variable size | Low frequency | 15-45 dB | Variable |
- Histologic focus size: <1mm (clinical), >2mm (surgical)
- Bone turnover rate: 20x normal in active disease
- Fluoride uptake: 3-5x increased on bone scan
- Progression rate: 1-2 dB/year untreated
- Cholesteatoma Growth Dynamics
- Epithelial migration rate: 0.1-0.3 mm/day
- Keratin accumulation: exponential in closed spaces
- Bone erosion enzymes: collagenase, acid phosphatase
- Complication risk: 10% intracranial, 15% facial nerve
⭐ Clinical Pearl: Carhart notch at 2000 Hz with 15-20 dB bone conduction depression indicates stapes fixation with 95% specificity, even when air conduction appears normal at this frequency.
💡 Master This: Cholesteatoma's "silent destruction" pattern-normal hearing with retraction pockets progresses to 40+ dB conductive loss over 2-5 years, making annual otoscopy critical for early detection.
These pathophysiologic principles connect directly to pattern recognition frameworks that enable rapid diagnosis based on audiometric and otoscopic findings, transforming complex disease processes into actionable clinical insights.
🔬 Pathophysiology Powerhouse: Disease Mechanisms Decoded
🎨 Pattern Recognition Mastery: Diagnostic Frameworks Unleashed
Audiometric Pattern Recognition Matrix
Transform audiometric curves into instant diagnoses using these high-yield pattern correlations:
-
Conductive Loss Signatures
- Flat pattern + 40-50 dB gap = Ossicular disruption (85% incus erosion)
- Low-frequency loss + 25-35 dB gap = TM perforation (>5mm diameter)
- Carhart notch + 2kHz dip = Stapes fixation (95% otosclerosis)
- High-frequency tilt + 30-40 dB gap = Malleus fixation (70% congenital)
-
Sensorineural Loss Patterns
- High-frequency slope + >40 dB at 4kHz = Noise-induced (4kHz notch)
- Asymmetric loss + >15 dB difference = Retrocochlear (95% if >20 dB)
- Cookie-bite + mid-frequency dip = Genetic (DFNA mutations)
- Precipitous drop + >60 dB/octave = Sudden SNHL (viral/vascular)
📌 Remember: SHARP for retrocochlear indicators - Speech discrimination poor (<70%), High-frequency rollover, Asymmetric loss (>15 dB), Reflex decay positive, Poor ABR wave morphology
Otoscopic Decision Trees
Systematic otoscopic evaluation using the "CLEAR" approach:
-
Color Assessment Hierarchy
- Gray/translucent = Normal (95% healthy ears)
- Red/bulging = Acute otitis media (bacterial >80%)
- Yellow/amber = Serous otitis media (viral/allergic)
- White/opaque = Chronic changes (fibrosis/calcification)
- Blue/purple = Hemotympanum (trauma/barotrauma)
-
Landmark Visibility Scoring
- All landmarks clear = Normal middle ear (>95% specificity)
- Malleus obscured = Fluid/inflammation (80% sensitivity)
- Light reflex absent = TM abnormality (70% sensitivity)
- Pars flaccida retraction = Cholesteatoma risk (40% progression)
| Clinical Scenario | Key Pattern | Diagnostic Accuracy | Next Step |
|---|---|---|---|
| Unilateral CHL + normal TM | Ossicular fixation | 90% | CT temporal bones |
| Bilateral CHL + family history | Otosclerosis | 95% | Audiometry + tympanometry |
| Asymmetric SNHL + tinnitus | Retrocochlear | 85% | MRI with gadolinium |
| Fluctuating loss + vertigo | Meniere's disease | 80% | Electrocochleography |
| Sudden SNHL + viral prodrome | Viral labyrinthitis | 75% | Steroids within 72 hours |
💡 Master This: The "whispered voice test" at 2 feet detects hearing loss >30 dB with 90% sensitivity-patients who cannot repeat 3/6 whispered words need formal audiometry.
These pattern recognition tools enable rapid triage and diagnosis, connecting seamlessly to systematic comparison frameworks that differentiate similar presentations with quantitative precision.
🎨 Pattern Recognition Mastery: Diagnostic Frameworks Unleashed
⚖️ Differential Diagnosis Architecture: Systematic Discrimination Mastery
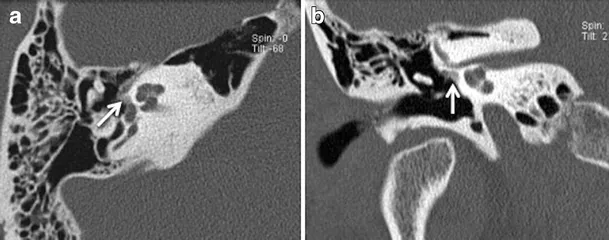
Conductive Hearing Loss Discrimination Matrix
Systematic differentiation of conductive pathology using quantitative clinical parameters:
| Parameter | Otosclerosis | Ossicular Disruption | Chronic Otitis Media | Congenital Atresia | TM Perforation |
|---|---|---|---|---|---|
| Age of Onset | 20-40 years | Post-trauma/infection | Childhood onset | Birth | Any age |
| Air-Bone Gap | 50-60 dB | 45-65 dB | 30-50 dB | 60+ dB | 15-45 dB |
| Bone Conduction | Carhart notch | Normal | Mixed loss | Variable | Normal |
| Tympanometry | Type A/As | Type Ad | Type B/C | Absent | Variable |
| Acoustic Reflexes | Absent | Absent | Absent | Absent | Present if small |
| Family History | 80% positive | Negative | Variable | 15% genetic | Negative |
| CT Findings | Lucent focus | Ossicular erosion | Soft tissue/erosion | Canal atresia | Normal bones |
- Clinical: Progressive CHL + normal TM + family history
- Audiometric: Carhart notch + bone conduction <30 dB at 500 Hz
- Surgical: Stapes fixation + pink promontory (Schwartze sign)
- Histologic: Otospongiotic foci with increased vascularity
- Ossicular Chain Disruption Patterns
- Incus erosion: Most common (60%), affects long process first
- Malleus fixation: Congenital (70%) vs acquired (30%)
- Stapes disruption: Trauma (80%) vs infection (20%)
- Complete discontinuity: Maximum CHL (60-65 dB)
📌 Remember: OTOSCLEROSIS mnemonic - Onset young adult, Tinnitus common, Otoscopy normal, Schwartze sign, Carhart notch, Low bone conduction, Exploratory surgery diagnostic, Recessive inheritance, Oval window focus, Stapedectomy curative, Improvement >90%, Sodium fluoride medical option
Sensorineural Hearing Loss Differentiation Framework
Vestibular Disorder Discrimination
| Condition | Episode Duration | Hearing Loss | Nystagmus Pattern | Triggers | Diagnostic Test |
|---|---|---|---|---|---|
| BPPV | <2 minutes | None | Rotatory/upbeat | Position change | Dix-Hallpike |
| Meniere's | 20min-12hrs | Fluctuating | Horizontal | Spontaneous | Electrocochleography |
| Vestibular Neuritis | Days-weeks | None | Horizontal | Viral prodrome | Head impulse test |
| Migraine | Minutes-hours | Variable | Variable | Triggers | Clinical criteria |
| Acoustic Neuroma | Progressive | Asymmetric | Minimal | None | MRI gadolinium |
- Definite: ≥2 episodes vertigo 20min-12hrs + SNHL + tinnitus/fullness + not better explained
- Probable: 1 episode vertigo + audiometric SNHL + tinnitus/fullness
- Possible: Episodic vertigo without documented hearing loss
- Retrocochlear Indicators (High Suspicion Criteria)
- Asymmetric SNHL >15 dB at ≥2 frequencies
- Speech discrimination <70% or >20% asymmetry
- ABR wave V latency >0.4ms interaural difference
- Acoustic reflex decay >50% at 10 seconds
⭐ Clinical Pearl: Sudden SNHL with >30 dB loss requires oral steroids within 72 hours for 65% recovery rate vs 35% spontaneous recovery-intratympanic steroids salvage 15-20% additional patients.
💡 Master This: Acoustic neuroma presents with asymmetric high-frequency SNHL in 95% of cases, but only 5% have classic triad of hearing loss, tinnitus, and vertigo-MRI sensitivity approaches 100% for tumors >2mm.
These systematic discrimination tools connect directly to evidence-based treatment algorithms that optimize outcomes through precise therapeutic targeting based on specific pathophysiologic mechanisms.
⚖️ Differential Diagnosis Architecture: Systematic Discrimination Mastery
🎯 Treatment Algorithm Mastery: Evidence-Based Intervention Strategies
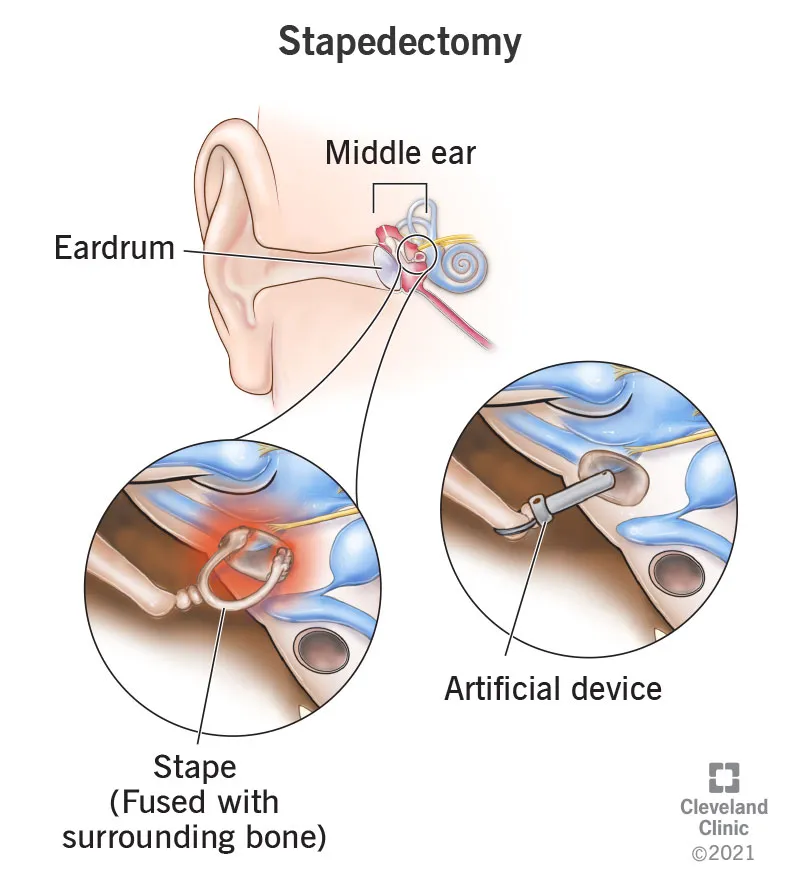
Surgical Decision Algorithm Framework
Stapedectomy Outcomes Matrix
Patient Selection Criteria with Success Predictors:
| Parameter | Excellent Outcome | Good Outcome | Poor Outcome | Success Rate |
|---|---|---|---|---|
| Bone Conduction | <25 dB | 25-35 dB | >35 dB | 95%/85%/60% |
| Age | 20-50 years | 50-65 years | >65 years | 95%/90%/85% |
| Otosclerosis Type | Fenestral | Retrofenestral | Cochlear | 95%/80%/50% |
| Preop Discrimination | >90% | 80-90% | <80% | 95%/85%/70% |
| Revision Surgery | Primary | First revision | Multiple | 95%/75%/45% |
- Air-bone gap closure <10 dB: 90% of patients
- Hearing improvement ≥15 dB: 95% of patients
- Sensorineural hearing loss: <1% risk (experienced surgeons)
- Facial nerve injury: <0.1% risk
- Vertigo (persistent): <2% incidence
- Prosthesis Selection Impact
- Piston diameter: 0.4mm vs 0.6mm (no difference in outcomes)
- Material: Titanium vs Teflon (equivalent results)
- Length: 4.5mm standard (±0.25mm adjustment)
📌 Remember: STAPEDECTOMY success factors - Stable footplate, Thin crura, Adequate bone conduction (<30 dB), Patient age (<60), Experienced surgeon, Discrimination good (>80%), Ear anatomy normal, Cochlear reserve, Technique standardized, Otosclerosis fenestral, Motivated patient, Young adult preferred
Tympanoplasty Success Optimization
Graft Selection Algorithm based on Evidence-Based Outcomes:
-
Temporalis Fascia (Gold Standard)
- Success rate: 85-95% for small-medium perforations
- Advantages: Autologous, excellent integration, low cost
- Optimal for: <50% TM perforation, dry ear >3 months
-
Cartilage-Perichondrium Composite
- Success rate: 90-98% for large/revision cases
- Advantages: Structural support, infection resistance
- Optimal for: >50% perforation, eustachian tube dysfunction
-
Synthetic Materials (AlloDerm/Biodesign)
- Success rate: 80-90% (slightly lower than autografts)
- Advantages: No donor site, consistent thickness
- Optimal for: Revision surgery, limited fascia
Cochlear Implant Candidacy Algorithm
Adult Candidacy Criteria (FDA Guidelines 2022):
| Parameter | Traditional Criteria | Expanded Criteria | Outcomes |
|---|---|---|---|
| Pure Tone Average | ≥70 dB | ≥60 dB | Equivalent benefit |
| Speech Recognition | ≤40% sentences | ≤50% sentences | Significant improvement |
| Duration of Deafness | <30 years optimal | <50 years acceptable | Plasticity dependent |
| Age | No upper limit | >65 years excellent | Motivation key |
| Medical Fitness | ASA 1-3 | Cardiac clearance | Low surgical risk |
- Open-set speech recognition: 80% achieve >50% sentences
- Telephone use: 65% successful within 12 months
- Music appreciation: 40% report satisfaction
- Quality of life: Significant improvement in >90%
⭐ Clinical Pearl: Cochlear implant outcomes correlate strongest with duration of auditory deprivation-patients implanted within 10 years of profound loss achieve 85% excellent outcomes vs 45% after >20 years deprivation.
💡 Master This: Tympanoplasty success depends on eustachian tube function-patients with normal tympanometry preoperatively achieve 95% graft take vs 70% with persistent dysfunction.
These evidence-based treatment algorithms connect seamlessly to multi-system integration concepts that optimize outcomes through comprehensive patient management and long-term follow-up strategies.
🎯 Treatment Algorithm Mastery: Evidence-Based Intervention Strategies
🌐 Multi-System Integration Hub: Advanced Otologic Connections
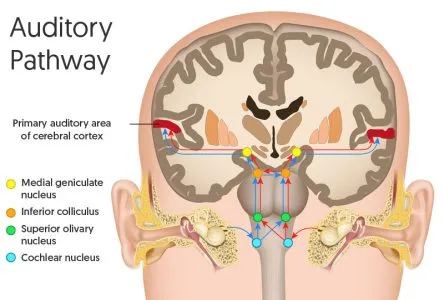
Neurocognitive-Auditory Integration Network
Hearing Loss Cognitive Impact (Longitudinal Studies 2020-2023):
-
Cognitive Load Theory in Hearing Loss
- Working memory demands increase 40-60% with moderate hearing loss
- Processing speed decreases 15-25% per 10 dB hearing loss
- Executive function decline accelerates 2-3x in untreated presbycusis
- Dementia risk increases 24% per 10 dB hearing loss after age 60
-
Central Auditory Processing Integration
- Brainstem plasticity: 6-12 months for cochlear implant adaptation
- Cortical reorganization: Cross-modal plasticity in superior temporal gyrus
- Attention networks: Effortful listening depletes cognitive reserves
- Memory consolidation: Auditory input critical for hippocampal function
📌 Remember: BRAIN-EAR connection - Brainstem processing, Recognition cortical, Attention networks, Inhibition reduced, Neuroplasticity critical, Effortful listening, Auditory deprivation, Reorganization maladaptive
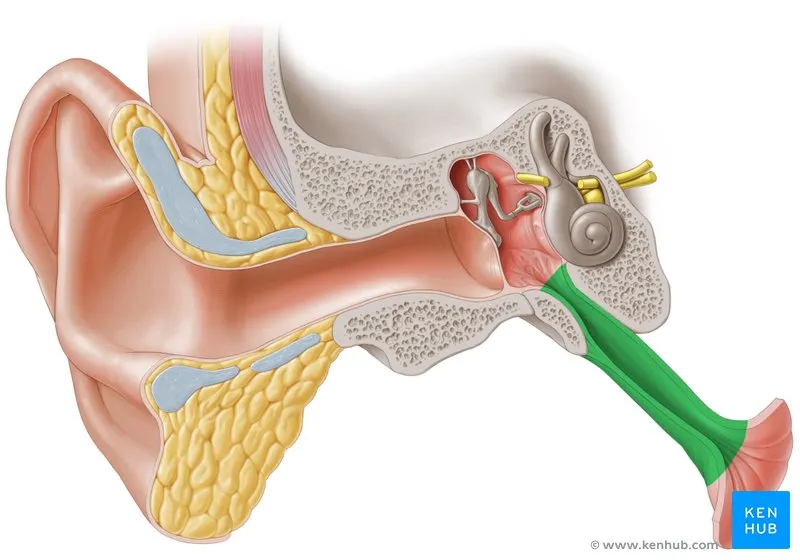
Respiratory-Otologic System Interface
Eustachian Tube Dysfunction creates cascading effects across multiple organ systems:
| System | Primary Effect | Secondary Impact | Clinical Manifestation | Quantitative Measure |
|---|---|---|---|---|
| Respiratory | Mucosal inflammation | Chronic sinusitis | Persistent congestion | >30% improvement with treatment |
| Immunologic | Biofilm formation | Recurrent infections | Antibiotic resistance | 3-5x higher infection rate |
| Vestibular | Pressure asymmetry | Balance dysfunction | Spatial disorientation | >20% VOR asymmetry |
| Neurologic | Referred pain | Headache patterns | Trigeminal sensitization | 40% migraine association |
| Sleep | OSA interaction | Pressure changes | Sleep fragmentation | 15-25% AHI increase |
- Shared inflammatory mediators: IL-4, IL-13, IgE elevation
- Eustachian tube edema: 50-70% reduction in diameter
- Treatment response: Intranasal steroids reduce OM episodes by 40%
- Seasonal patterns: Spring/fall peaks correlate 85% with pollen counts
Cardiovascular-Auditory Relationships
Emerging Research (2022-2024 Studies):
-
Microvascular Disease Correlation
- Diabetes: 2-3x higher SNHL risk, high-frequency predominance
- Hypertension: Cochlear blood flow reduction, 15% per 20mmHg increase
- Atherosclerosis: Vertebrobasilar insufficiency causes sudden SNHL
- Smoking: 70% increased hearing loss risk, dose-dependent
-
Sudden Sensorineural Hearing Loss Vascular Etiology
- Anterior inferior cerebellar artery (AICA) infarction: 5-10% of cases
- Vertebral artery dissection: Wallenberg syndrome with hearing loss
- Sickle cell disease: Vaso-occlusive episodes affect cochlear circulation
- Cogan's syndrome: Autoimmune vasculitis with audiovestibular symptoms
⭐ Clinical Pearl: Sudden SNHL in patients >50 years with cardiovascular risk factors requires MRI to exclude posterior circulation stroke-15% have vertebrobasilar pathology requiring anticoagulation.
💡 Master This: Hearing aid use in mild-moderate hearing loss reduces cognitive decline by 32% and dementia risk by 18%-early intervention provides neuroprotective benefits beyond auditory improvement.
These multi-system integration principles culminate in comprehensive mastery frameworks that synthesize complex otologic knowledge into practical clinical tools for immediate application.
🌐 Multi-System Integration Hub: Advanced Otologic Connections
🏆 Clinical Mastery Arsenal: Rapid Reference & Integration Tools
Essential Clinical Numbers Arsenal
Critical Thresholds for Immediate Decision-Making:
-
Hearing Loss Severity Classification
- Normal: ≤25 dB HL
- Mild: 26-40 dB HL (hearing aid consideration)
- Moderate: 41-55 dB HL (hearing aid recommended)
- Moderately Severe: 56-70 dB HL (power aids)
- Severe: 71-90 dB HL (cochlear implant evaluation)
- Profound: >90 dB HL (cochlear implant candidate)
-
Surgical Intervention Thresholds
- Air-bone gap >30 dB = Surgical consideration
- Bone conduction <30 dB = Excellent stapedectomy candidate
- Speech discrimination <70% = Retrocochlear workup
- Asymmetric loss >15 dB = MRI indicated
- Sudden SNHL >30 dB = Steroids within 72 hours
📌 Remember: OTOLOGIC EMERGENCY criteria - Onset sudden (<72 hrs), Tinnitus pulsatile, Otalgia severe, Loss asymmetric (>15 dB), Otorrhea purulent, Giddiness with nystagmus, Infection spreading, Cranial nerve palsy
Rapid Diagnostic Decision Matrix
| Clinical Presentation | Key Discriminator | Immediate Action | Success Rate |
|---|---|---|---|
| Sudden SNHL | <72 hours onset | Oral steroids 1mg/kg | 65% recovery |
| Asymmetric SNHL | >15 dB difference | MRI with gadolinium | 95% sensitivity |
| Conductive loss + normal TM | Carhart notch present | CT temporal bones | 90% diagnostic |
| Vertigo + hearing loss | Episodic pattern | Electrocochleography | 80% Meniere's |
| Otalgia + discharge | Granulation tissue | Culture + biopsy | 85% malignancy rule-out |
The Otologic Excellence Framework:
- "Every asymmetric SNHL >15 dB gets MRI" - Acoustic neuroma detection >95%
- "Sudden SNHL is steroid emergency <72 hours" - Recovery rate 65% vs 35%
- "Carhart notch = stapes fixation until proven otherwise" - 95% specificity
- "Pulsatile tinnitus demands vascular imaging" - Glomus tumor 15% incidence
- "Conductive loss + normal TM = ossicular pathology" - CT required
- "Cholesteatoma grows silently - annual otoscopy saves hearing" - Early detection critical
- "Cochlear implants work best within 10 years of deafness" - Plasticity window
⭐ Clinical Pearl: The "Rule of 15s" in otology - >15 dB asymmetry needs MRI, >15 years deafness reduces CI outcomes, <15 dB air-bone gap rarely needs surgery.
💡 Master This: Otologic triage follows the "HEAR" protocol - History focused (onset/asymmetry), Examination systematic (otoscopy/tuning forks), Audiometry when indicated (>25 dB loss), Referral for surgical candidates or sudden loss.
This clinical mastery arsenal transforms years of otologic training into immediately accessible tools that enable expert-level decision-making, optimal patient outcomes, and confident management of complex ear disorders across all clinical settings.
🏆 Clinical Mastery Arsenal: Rapid Reference & Integration Tools
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























