Ossicular Shake‑Up - Bone‑rattling Blows
Traumatic ossicular disruption: A break in the ossicular chain (📌 M-I-S: Malleus, Incus, Stapes) due to trauma, often resulting in conductive hearing loss.
- Mechanisms:
- Direct: Penetrating injury (e.g., Q-tip).
- Indirect: Head trauma, whiplash.
- Blast injuries: Explosions.
- Barotrauma: Sudden pressure changes.
- Frequent Causes:
- Temporal bone fractures (longitudinal > transverse for ossicular injury).
- Direct penetrating trauma to tympanic membrane.
- Iatrogenic (e.g., during mastoidectomy).

⭐ Temporal bone fractures, especially longitudinal types, are a leading cause of traumatic ossicular disruption.
Chain Reaction Chaos - Break‑Down Patterns
- Primary Mechanisms:
- Inertial/Indirect Force: Common in head trauma (e.g., RTA, falls); ossicles move differentially.
- Direct Force: Penetrating injuries (e.g., foreign body, q-tip), surgical trauma, or temporal bone fractures.
- Hierarchy of Vulnerability (Most to Least Common):
- Incudostapedial (I-S) Joint: Separation/subluxation is most frequent. (📌 "I"njury "S"eparates Incus & Stapes)
- Incudomalleolar (I-M) Joint: Disruption or dislocation.
- Stapes: Crural fracture, footplate fracture, or subluxation into vestibule.
- Malleus: Fracture (less common).
- Dislocation Patterns:
- Isolated: Single joint/ossicle affected.
- Multiple/Combined: Complex disruptions involving several ossicular components.
⭐ The incudostapedial joint is the most frequently disrupted articulation in ossicular trauma due to its delicate nature and tenuous blood supply.
Sounding the Alarm - Signs & Scans
- Symptoms: Conductive hearing loss (CHL), tinnitus, otalgia, vertigo, bleeding from ear.
- Signs: Hemotympanum, TM perforation; Rinne: bone > air (affected ear); Weber: lateralizes to affected ear. Visible ossicular displacement (rare).
- Diagnostic Tests:
- Otoscopy: Key initial assessment.
- Tuning Fork Tests: Confirm CHL.
- Pure Tone Audiometry (PTA): CHL, often 40-60 dB; air-bone gap > 30 dB.
- Imaging: High-Resolution CT (HRCT) of temporal bone (axial & coronal views) to visualize ossicles.
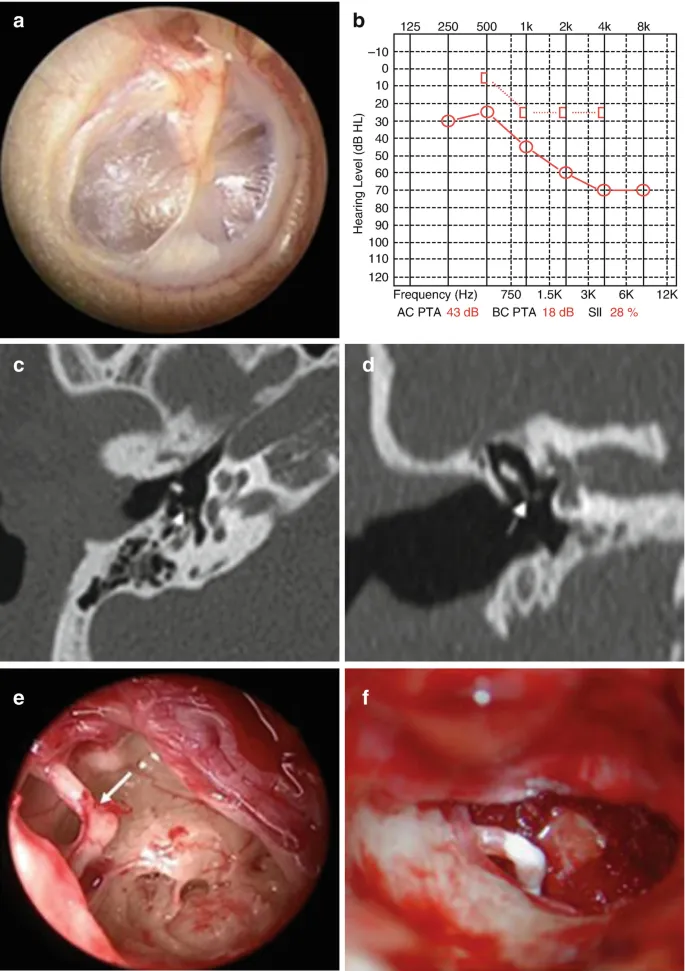
⭐ A conductive hearing loss with an air-bone gap exceeding 30 dB following head trauma is highly suggestive of ossicular disruption.
Fixing the Links - Repair & Restore
- Management Approach:
- Conservative: Observation if CHL is minor.
- Surgical: Indicated for significant CHL impacting quality of life, or patient preference.
- Timing: Delayed repair (3-6 months post-trauma) is preferred for TM healing and edema resolution.
- Surgical Options:
- Exploratory tympanotomy.
- Ossiculoplasty: Using PORP (Partial Ossicular Replacement Prosthesis) or TORP (Total Ossicular Replacement Prosthesis).
- Graft materials: Autograft (cartilage/ossicle), bone cement, synthetic prostheses.
⭐ Exploratory tympanotomy with ossiculoplasty is the definitive management for persistent, symptomatic conductive hearing loss due to traumatic ossicular disruption.
Aftershock Assessment - Risks & Recovery
- Injury Risks: Persistent CHL, SNHL, facial nerve injury (with fracture), CSF leak.
- Surgical Risks (Ossiculoplasty): Graft displacement/extrusion, recurrent CHL, infection, SNHL.
- Prognosis Hinges On:
- Disruption type
- Stapes integrity
- TM status
- Surgical technique & graft material
- Hearing Gain: Variable post-operatively.
⭐ The integrity of the stapes suprastructure is a critical prognostic factor for successful hearing restoration in ossiculoplasty.
High‑Yield Points - ⚡ Biggest Takeaways
- Head trauma, especially temporal bone fracture, is the leading cause.
- Incus is the most commonly dislocated/damaged ossicle, often at the incudostapedial joint.
- Stapes crural fracture is another common injury pattern.
- Key symptom: Maximal conductive hearing loss (CHL), around 50-60 dB.
- High-Resolution CT (HRCT) of temporal bone is diagnostic.
- Audiometry confirms CHL with an air-bone gap.
- Treatment is typically surgical repair (ossiculoplasty) for persistent CHL_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

