Perilymphatic Fistula - Leaky Labyrinth Intro
- Definition: An abnormal communication between the perilymph-filled space of the inner ear and the air-filled middle ear cavity or mastoid.
- "Leaky Labyrinth": Refers to the leakage of perilymph, typically through the oval or round windows.
- Common Sites of Leakage:
- Oval window (especially fissula ante fenestram).
- Round window membrane.
- Etiology:
- Traumatic: Head injury, barotrauma (e.g., diving, flying), iatrogenic (post-stapedectomy, cochlear implantation).
- Congenital: Inner ear malformations (e.g., Mondini dysplasia, enlarged vestibular aqueduct).
- Spontaneous: Often after sudden increases in intracranial or intralabyrinthine pressure (e.g., straining, coughing, sneezing, Valsalva maneuver).
- Erosive (rare): Cholesteatoma, tumors.
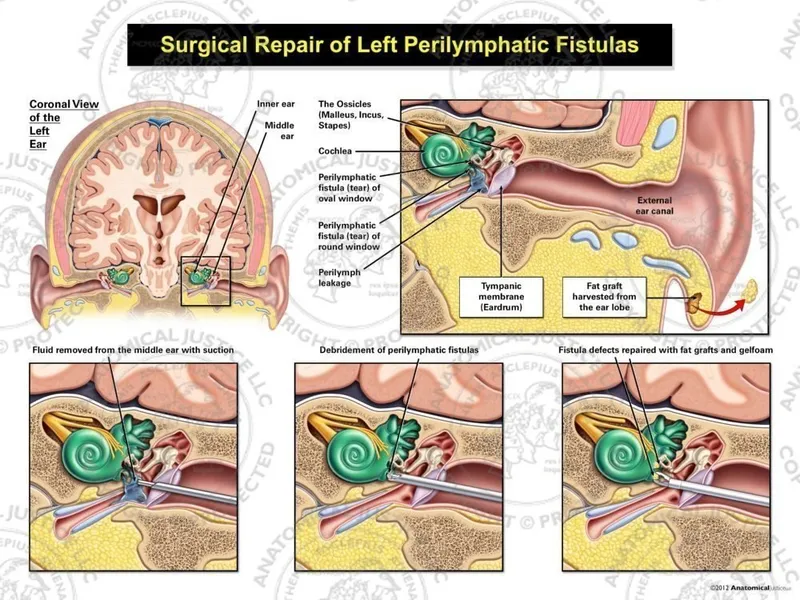
⭐ The oval window is the most common site for perilymphatic fistulas, particularly following trauma or stapes surgery.
Perilymphatic Fistula - Inner Ear Mayhem
- Abnormal communication between perilymph-filled inner ear & air-filled middle ear/mastoid.
- Etiology:
- Trauma: Head injury, barotrauma (diving, flying), iatrogenic (stapedectomy).
- Congenital: Inner ear malformations (e.g., Mondini dysplasia).
- Spontaneous: Often after straining, coughing, sneezing.
- Erosive: Cholesteatoma, tumors.
- Pathophysiology: Leakage of perilymph → pressure changes in cochlea & vestibule → auditory & vestibular symptoms.
- Clinical Features:
- Episodic vertigo, often triggered by Valsalva, loud noises (Tullio phenomenon), or pressure changes.
- Fluctuating sensorineural hearing loss (SNHL), often low-frequency initially.
- Tinnitus, aural fullness.
- Hennebert's sign: Nystagmus/vertigo on tragal pressure (positive fistula test).
- Tullio phenomenon: Sound-induced vertigo/nystagmus.
⭐ Fistula Test (Hennebert's Sign): Induction of nystagmus and vertigo by applying positive or negative pressure to the external auditory canal using a Politzer bag or pneumatic otoscope. A positive test strongly suggests PLF, but can also be seen in Meniere's disease (due to saccular fibrosis) or semicircular canal dehiscence.
- Diagnosis: Often clinical; CT temporal bone may show defect. Exploratory tympanotomy is gold standard for confirmation & repair.
- Management: Bed rest, head elevation, avoidance of straining. Surgical repair (grafting oval/round window) if conservative measures fail or symptoms are severe/persistent.
Perilymphatic Fistula - Spotting the Seep
- Objective: Confirm perilymph leakage from inner ear (oval/round window) to middle ear.
- Clinical Provocative Tests:
- Fistula Test (Hennebert's sign): Nystagmus/vertigo with pneumatic otoscopy/tragal pressure.
- Tullio Phenomenon: Loud sounds induce vertigo/nystagmus.
- Investigations:
- Audiometry: Sensorineural hearing loss (SNHL), often fluctuating/progressive.
- VEMP/ECoG: May be abnormal; non-specific.
- Imaging (HRCT/MRI): Rarely diagnostic for leak; may show fluid, helps rule out other issues.
- Gold Standard: Exploratory tympanotomy for direct visualization and repair.
⭐ Beta-2 transferrin assay of aspirated middle ear fluid is highly specific for perilymph/CSF, confirming leak.
Perilymphatic Fistula - Plugging the Problem
-
Conservative Management (Initial):
- Strict bed rest, head elevation.
- Avoidance of straining (stool softeners, cough suppressants).
- Observation for 1-2 weeks; spontaneous healing possible.
-
Surgical Management (If conservative fails or severe symptoms):
- Tympanotomy and exploration of oval and round windows.
- Grafting material: temporalis fascia, perichondrium, fat, fibrin glue.
- Aim: Seal the fistula.
-
Flowchart: Management Approach
-
Post-operative Care:
- Continued bed rest initially.
- Avoidance of pressure changes (flying, diving).
-
Prognosis & Complications:
- Variable; depends on duration and severity.
- Potential for persistent hearing loss or vestibular symptoms.
- Rare: meningitis.
⭐ High-Yield Fact: Surgical repair of a perilymphatic fistula primarily aims to stabilize or improve vestibular symptoms; hearing improvement is less predictable and often not the primary outcome achieved.
- 📌 Mnemonic: PLUG it - Positioning (bed rest), Limit straining, Undergo surgery (if needed), Grafting windows.
High‑Yield Points - ⚡ Biggest Takeaways
- Abnormal connection between perilymphatic space of inner ear and middle ear/mastoid.
- Often post-traumatic (e.g., head injury, barotrauma, stapes surgery) or congenital.
- Key symptoms: Episodic vertigo, fluctuating/progressive sensorineural hearing loss (SNHL).
- Tullio phenomenon (sound-induced vertigo) and Hennebert's sign (pressure-induced nystagmus/vertigo) are suggestive.
- Diagnosis is often clinical; exploratory tympanotomy is gold standard for confirmation & repair.
- Management: Initial conservative measures (bed rest, head elevation); surgical repair (grafting) if symptoms persist.
- Associated with sudden SNHL or vertigo after straining, coughing, or nose-blowing (Valsalva).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

