Introduction & Etiology - Dizzying Blows
- Labyrinthine Concussion: Defined as a transient vestibulocochlear dysfunction (hearing and balance impairment) occurring after trauma.
- Etiology - The "Dizzying Blows":
- Head Injury: Most common; direct impact or indirect (acceleration-deceleration, whiplash).
- Barotrauma: Sudden pressure changes (e.g., blast exposure, diving accidents).
- Intense Noise Exposure: Acoustic trauma.
- Mechanism (Brief): Shearing forces damage the delicate membranous labyrinth. May involve micro-hemorrhages or transient endolymphatic hydrops.
⭐ Head trauma accounts for the majority of labyrinthine concussion cases.
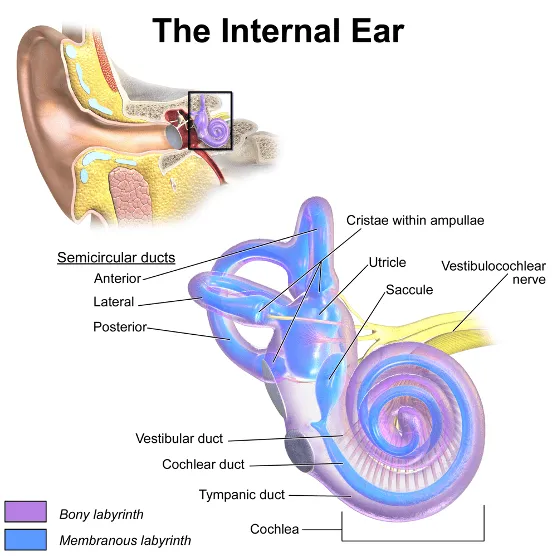
Pathophysiology & Clinical Features - Inner Ear Turmoil
- Pathophysiology:
- Traumatic injury damages delicate inner ear neuroepithelium: cochlear hair cells, utricular/saccular maculae, semicircular canal cristae.
- Possible otoconial (otolith) displacement from maculae, leading to BPPV-like positional vertigo.
- Clinical Triad (📌 VHT):
- Vertigo: Sudden, severe, often rotational; can be positional (provoked by head movements).
- Sensorineural Hearing Loss (SNHL): Typically high-frequency, usually transient but may persist.
- Tinnitus: Subjective ringing or buzzing sound.
- Other Symptoms: Nausea, vomiting, imbalance/ataxia, headache, aural fullness.
- Onset: Acute, developing within hours to a few days post-trauma.

⭐ Sudden, severe vertigo appearing post-head trauma, especially with transient SNHL, is highly indicative of labyrinthine concussion.
Diagnosis - Spotting the Spin
- History: Detailed trauma (mechanism, severity, timing of symptoms).
- Clinical Exam: Otoscopy (usually normal TM), Cranial nerve exam, Romberg, Fukuda stepping test.
- Tuning Fork Tests: Weber lateralizes away from affected ear (SNHL), Rinne AC > BC (positive).
- Provocative Maneuvers: Dix-Hallpike (for associated BPPV - look for torsional nystagmus).

- Audiometry: Pure Tone Audiometry (PTA) to confirm SNHL (often high-frequency dip), Speech audiometry.
⭐ High-frequency sensorineural hearing loss is a characteristic audiometric finding.
- Vestibular Function Tests (VFTs): Videonystagmography (VNG)/Electronystagmography (ENG) may show unilateral vestibular hypofunction. Head Impulse Test (HIT/vHIT).
- Imaging (to rule out other pathology): CT temporal bone (fractures), MRI brain (central causes, or if PLF suspected & symptoms severe/persistent).
Differential Diagnosis - Ruling Out Rivals
- BPPV: Positional vertigo; Dix-Hallpike positive.
⭐ BPPV can be a sequela of labyrinthine concussion.
- Perilymphatic Fistula (PLF): Vertigo with straining (Tullio phenomenon), fluctuant SNHL.
- Temporal Bone Fracture: Otorrhea, hemotympanum, Battle's sign.
- Meniere’s Disease: Episodic vertigo, tinnitus, SNHL; less clear trauma link.
- Vestibular Neuritis/Labyrinthitis: Post-viral; acute sustained vertigo; +/- SNHL.
- Central Causes (e.g., VBI, cerebellar stroke): Other neurological signs (diplopia, ataxia).
Management & Prognosis - Steadying the Course
- Acute Phase: Bed rest, reassurance.
- Symptomatic Relief (<3 days):
- Antiemetics (e.g., Prochlorperazine).
- Vestibular suppressants (e.g., Diazepam 2-5mg, Meclizine).
- Corticosteroids: Controversial; consider for severe SNHL (Prednisolone 1mg/kg/day tapered).
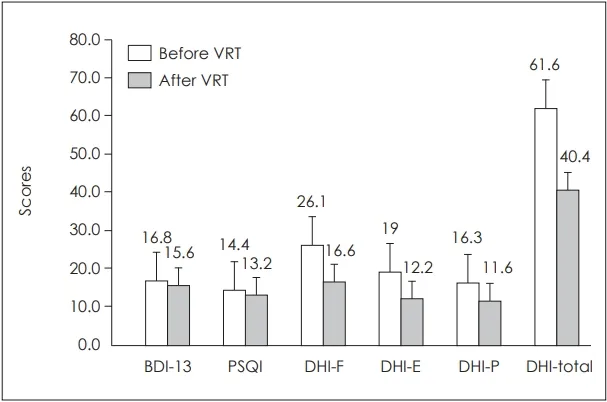
- Vestibular Rehabilitation Therapy (VRT): Crucial for persistent dizziness/imbalance (e.g., Cawthorne-Cooksey exercises).
- Associated BPPV: Manage with Epley maneuver if identified.
- Prognosis: Generally good; symptoms typically resolve in 4-6 weeks. Some may experience persistent issues.
⭐ Vestibular Rehabilitation Therapy (VRT) is the primary treatment for persistent disequilibrium following labyrinthine concussion.
High‑Yield Points - ⚡ Biggest Takeaways
- Caused by head trauma (even mild), leading to inner ear dysfunction without fracture.
- Key symptoms: sudden vertigo, nausea, vomiting, often with transient sensorineural hearing loss and tinnitus.
- Otoscopy and imaging (CT/MRI) are typically normal.
- Caloric testing may show canal paresis or vestibular hypofunction on the affected side.
- Management is primarily conservative and symptomatic: bed rest, antiemetics, and vestibular suppressants (e.g., dimenhydrinate).
- Prognosis is generally good, with symptoms usually resolving spontaneously within days to a few weeks.
- Must differentiate from BPPV, labyrinthine fistula, and temporal bone fractures which may have similar onset.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

