Facial Nerve Anatomy & Basics - Nerve Nuances
- Nuclei (Pons): Motor, Sup. Salivatory (parasymp), NTS (sensory).
- Functions: Motor (face), Glands (lacrimal, submandibular/lingual), Taste (ant. 2/3 tongue). 📌 FACE-L: Facial expression, Acoustic reflex, Chorda, Eye closure, Lacrimation.
- Course: CPA → IAM → Facial Canal (geniculate ganglion) → Stylomastoid foramen.
- Branches (in canal):
- Greater Petrosal (lacrimation)
- N. to Stapedius (stapedial reflex)
- Chorda Tympani (taste, salivation)
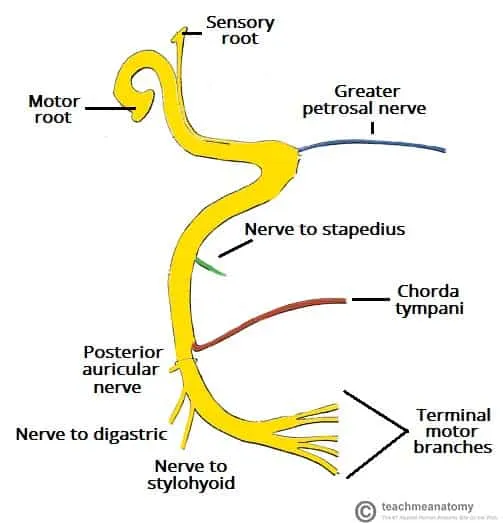
⭐ Labyrinthine segment: narrowest part of facial canal (~0.68mm), prone to compression in Bell's Palsy.
Causes & Localization of FNP - Culprit Countdown
-
Common Culprits (Causes):
- Idiopathic: Bell's Palsy (most frequent, >70%).
- Infections: Ramsay Hunt (VZV), Otitis Media, Lyme.
- Trauma: Temporal bone # (longitudinal/transverse).
- Neoplastic: Acoustic neuroma, parotid tumors.
-
Pinpointing the Lesion (LMN Topodiagnosis):
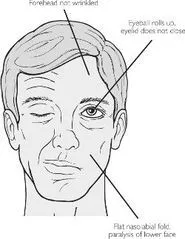
- UMN vs LMN: UMN spares forehead; LMN affects entire hemiface.
⭐ Bell's Palsy is a diagnosis of exclusion; always rule out sinister causes like tumors, especially in atypical/progressive FNP or recurrent FNP on the same side.
Clinical Evaluation & Grading - Face Facts
- History: Onset (sudden?), otalgia, vesicles (HZV), hearing loss, vertigo, trauma.
- Exam:
- Otoscopy: Check for vesicles, AOM.
- Differentiate UMN (forehead spared) vs LMN paralysis.
- Assess facial zones: Forehead, Eyes (Bell's phenomenon, closure), Mouth (smile, pucker).

- Grading: House-Brackmann (HB) Scale:
- I: Normal
- II: Mild
- III: Moderate
- IV: Mod-Severe
- V: Severe
- VI: Total
⭐ In LMN paralysis, Bell's phenomenon (upward outward rolling of eyeball on attempted eye closure) is present.
Key Syndromes & Management - Nerve Navigators
- Bell's Palsy: Most common, idiopathic LMN type.
- Sudden, unilateral.
- Rx:
- Corticosteroids (Prednisolone 1 mg/kg/day, max 60-80 mg, 7-10 days, taper). Start <72h.
- +/- Antivirals (Valacyclovir 1g TID / Acyclovir 400mg 5x/day, 7 days) if severe.
- Eye care (lubrication, patching).
- Ramsay Hunt Syndrome (Herpes Zoster Oticus): VZV origin.
- Facial palsy + otalgia + vesicles (ear/mouth). 📌 Pain, Palsy, Pox.
- Rx: Antivirals + Corticosteroids. Worse prognosis vs Bell's.
- Other Causes: Trauma (e.g., temporal bone #), Tumors, Infections (e.g., AOM, Lyme), Systemic (e.g., Sarcoidosis, GBS).
- General Rx:
- Grade severity (House-Brackmann).
- Corneal protection.
- Physiotherapy.
- Surgery (select cases: trauma, unresponsive Bell's).
⭐ For Bell's Palsy, corticosteroids initiated within 72 hours of onset yield maximal benefit.
Prognosis & Complications - Future Face
- Prognosis: Varies by cause, severity (House-Brackmann). Bell's: 85% recovery. ENoG >90% degeneration = poor.
- Complications:
- Corneal ulcers (exposure keratitis)
- Synkinesis (miswiring)
- Crocodile tears (gustatory lacrimation)
- Contractures
⭐ Synkinesis, due to aberrant nerve regeneration, is a common long-term complication.
High‑Yield Points - ⚡ Biggest Takeaways
- Bell's palsy: most common LMN facial paralysis, often idiopathic/viral (HSV-1).
- Ramsay Hunt syndrome (Herpes Zoster Oticus): facial palsy, ear pain, vesicles in auricle/EAC.
- House-Brackmann grading is standard for facial nerve function assessment.
- UMN lesions spare the forehead (bilateral innervation); LMN lesions affect the entire hemiface.
- Temporal bone fractures, especially transverse type, carry a high risk of facial nerve injury.
- Management: Corticosteroids (e.g., prednisolone) are mainstay for Bell's palsy; antivirals controversial. Eye care is crucial to prevent corneal complications.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

