Intro & Causes - Dizzying Depths
- Acute Vestibulopathy (AV): Sudden onset of vertigo, nausea/vomiting, and nystagmus due to unilateral peripheral vestibular dysfunction. No auditory or neurological symptoms (typically).
- Key Entities:
- Vestibular Neuritis (VN):
- Inflammation of the vestibular nerve (CN VIII).
- Presumed viral (HSV-1 reactivation common) or post-viral.
- Sudden, severe vertigo, lasting days to weeks.
- Nystagmus: Unidirectional, horizontal, suppressed by visual fixation.
- Positive head impulse test.
- No hearing loss or tinnitus.
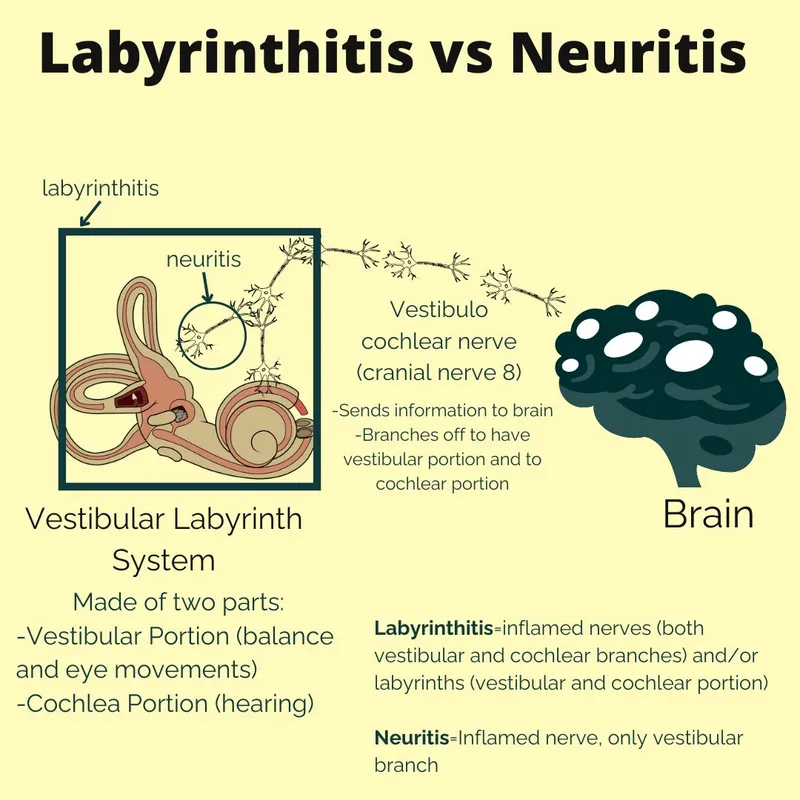
- Labyrinthitis:
- Inflammation of the labyrinth (vestibular & cochlear apparatus).
- Similar vestibular symptoms to VN.
- Key Differentiator: Associated auditory symptoms (hearing loss, tinnitus).
- Causes: Viral (mumps, measles), bacterial (otitis media extension), autoimmune.
- Vestibular Neuritis (VN):
- Other Causes (Less Common):
- Vascular (e.g., AICA stroke - but usually has other neurological signs).
- Trauma.
- Ototoxicity.
⭐ Vestibular neuritis is the second most common cause of peripheral vertigo after BPPV. It typically affects individuals aged 30-60 years.
📌 Mnemonic (VN vs. Labyrinthitis): Neuritis = No hearing loss; Labyrinthitis = Loss of hearing (and vestibular symptoms).
Clinical & HINTS - Spinning Signals
-
Acute Vestibulopathy (Peripheral):
- Sudden, severe vertigo (spinning).
- Nausea, vomiting, postural instability.
- Unidirectional, horizontal nystagmus (fast phase away from lesion), suppressed by fixation.
- Gait deviation to affected side.
- No other neurological deficits.
-
HINTS Exam (Differentiates Peripheral vs. Central AVS):
- Head Impulse Test (HIT):
- Peripheral: Abnormal (corrective saccade).
- Central: Normal.
- Nystagmus:
- Peripheral: Unidirectional, horizontal; ↑ with gaze to fast phase; fixation ↓.
- Central: Direction-changing, vertical, or pure torsional.
- Test of Skew:
- Peripheral: Absent.
- Central: Present.
- Head Impulse Test (HIT):
-
HINTS Interpretation:
- 📌 INFARCT (Central): Impulse Normal, Fast-phase Alternating, Refixation on Cover Test (Skew).
- One central sign = suspect stroke.
⭐ HINTS is more sensitive than early MRI (<48h) for posterior circulation stroke in Acute Vestibular Syndrome (AVS).

Diagnosis & Management - Steadying Steps
- Diagnostic Workup (Beyond HINTS if atypical/central concerns):
- MRI Brain: Essential to exclude stroke/central pathology.
- Audiogram: If hearing loss, differentiates neuritis from labyrinthitis.
- vHIT / Caloric testing (VNG): Confirms unilateral vestibular loss (UVL).
- Core Management Principles:
- Alleviate acute symptoms (vertigo, nausea).
- Promote vestibular compensation.
- Address underlying cause if identifiable (e.g., viral for neuritis).
- Pharmacological Management:
- Symptomatic Relief (short-term, max 72h):
- Antihistamines (e.g., Meclizine, Dimenhydrinate).
- Benzodiazepines (e.g., Diazepam, Lorazepam).
- Antiemetics (e.g., Ondansetron, Prochlorperazine).
- ⚠️ Prolonged use delays central compensation.
- Specific Treatment (Vestibular Neuritis):
- Corticosteroids: E.g., Prednisolone 1mg/kg/day (max 60mg), tapered over 10-14 days. Start within 72 hours of symptom onset.
- Symptomatic Relief (short-term, max 72h):
- Vestibular Rehabilitation Therapy (VRT):
- Cornerstone for long-term recovery; initiate ASAP.
- Aims: Enhance gaze stability, improve postural control, reduce sensitivity to head movements, promote central compensation.
- Includes: Cawthorne-Cooksey exercises, customized balance and gaze exercises.
⭐ Early and consistent Vestibular Rehabilitation Therapy (VRT) is the most critical factor for achieving complete recovery and preventing chronic symptoms in patients with acute peripheral vestibulopathy.
High‑Yield Points - ⚡ Biggest Takeaways
- Sudden onset of vertigo, nausea/vomiting, and gait instability.
- Often preceded by viral illness (e.g., vestibular neuritis).
- No auditory symptoms (like hearing loss or tinnitus) differentiates from labyrinthitis.
- Nystagmus is typically unidirectional, horizontal or horizontal-torsional, and suppressed by visual fixation.
- Head Impulse Test (HIT) is positive (corrective saccade when head turned towards affected side).
- Generally benign course with spontaneous recovery; vestibular rehabilitation aids faster improvement.
- Crucial to rule out stroke (posterior circulation) using HINTS exam (Head Impulse, Nystagmus, Test of Skew).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

