Otologic and Neurotologic Emergencies

On this page
🚨 Emergency Triage Mastery: The Otologic Crisis Command Center
When a patient arrives with acute vertigo, facial paralysis, or sudden hearing loss, the next 90 seconds of your assessment may determine whether you're managing a benign condition or averting a life-threatening stroke, meningitis, or intracranial catastrophe. This lesson equips you with the triage frameworks, diagnostic patterns, and time-critical interventions that separate otologic urgencies from true emergencies. You'll master rapid recognition of dangerous presentations, build systematic differential diagnosis skills, and deploy evidence-based protocols that optimize outcomes when every minute counts.
📌 Remember: DANGER - Deafness sudden, Auricular hematoma, Neurologic signs, Gushing CSF, Ear foreign body, Red flag vertigo. Each component demands immediate specialist consultation within 2-4 hours.
The temporal bone houses the densest concentration of neural structures in the human body, with the facial nerve traveling through 4 distinct segments spanning just 3 centimeters. This anatomical complexity means that emergency presentations often involve multiple systems simultaneously.
-
Immediate Life-Threatening Conditions (<1 hour intervention window)
- Intracranial complications of otitis media: 15-20% mortality if delayed
- Malignant otitis externa: 50% mortality without aggressive treatment
- Temporal bone fractures with CSF leak: 25% meningitis risk
- Longitudinal fractures: 80% of temporal bone injuries
- Transverse fractures: 20% but 90% sensorineural hearing loss
- Mixed pattern fractures: 40% facial nerve injury rate
-
Urgent Conditions (2-6 hour intervention window)
- Sudden sensorineural hearing loss: 30-65% recovery if treated within 72 hours
- Facial nerve paralysis: 85% recovery if steroids started within 24 hours
- Auricular hematoma: 6-hour window to prevent permanent deformity
- Cartilage necrosis begins after 6-8 hours of compression
- Cauliflower ear develops in >90% of untreated cases
⭐ Clinical Pearl: The "Rule of 6s" in otologic emergencies - 6 hours for auricular hematoma drainage, 6 cranial nerves potentially affected by temporal bone trauma, 6 millimeters maximum safe foreign body removal depth without specialist consultation.
| Emergency Type | Time Window | Mortality Risk | Functional Loss Risk | Key Diagnostic Sign |
|---|---|---|---|---|
| Intracranial complications | <1 hour | 15-20% | 40-60% neurologic | Altered mental status |
| Malignant otitis externa | <2 hours | 10-50% | 70% facial nerve | Granulation tissue |
| Temporal bone fracture | <4 hours | 5-10% | 60-90% hearing | Battle's sign |
| SSNHL | <72 hours | 0% | 35-70% hearing | Weber lateralization |
| Facial nerve paralysis | <24 hours | 0% | 15-30% facial | House-Brackmann >3 |
The emergency department evaluation must rapidly stratify patients into immediate surgical candidates, urgent specialist referrals, and those suitable for medical management with close follow-up. Understanding this triage framework transforms chaotic emergency presentations into systematic clinical decision-making.
🚨 Emergency Triage Mastery: The Otologic Crisis Command Center
🎯 Rapid Assessment Arsenal: The 90-Second Diagnostic Framework
📌 Remember: FAST-EAR assessment - Facial nerve function, Auditory acuity, Spontaneous nystagmus, Tympanic membrane integrity, External canal examination, Auricular inspection, Red flag symptoms. Complete evaluation requires <90 seconds in experienced hands.
The systematic approach begins with "Look, Listen, Test" - visual inspection for obvious deformity or drainage, auditory assessment for hearing loss patterns, and targeted neurologic testing for cranial nerve involvement. This sequence prevents anchoring bias while ensuring comprehensive evaluation.
-
Visual Inspection Priorities (15-second scan)
- Battle's sign: 70% sensitivity for temporal bone fracture
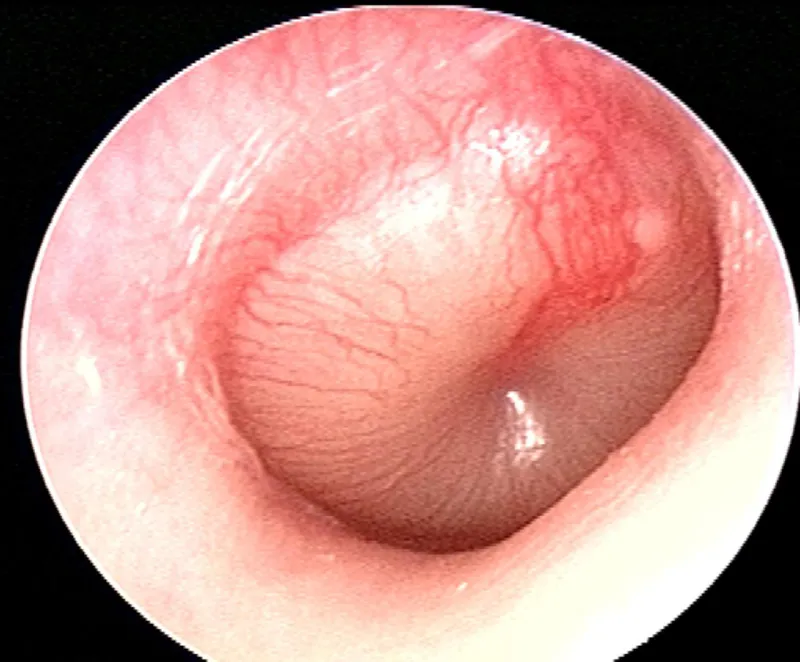
- Hemotympanum: 85% correlation with ossicular disruption
- CSF otorrhea: 25% of temporal bone fractures
- Clear fluid with glucose >30 mg/dL confirms CSF
- Beta-2 transferrin provides 99% specificity
- Halo sign on gauze suggests CSF contamination
-
Auditory Function Assessment (30-second evaluation)
- Weber test lateralization: >90% sensitivity for conductive loss
- Rinne test interpretation: 85% accuracy for ossicular pathology
- Whispered voice test: 80% correlation with >30 dB hearing loss
- Normal conversation: 60 dB sound level
- Whispered voice: 20 dB sound level
- Finger rub: 10 dB sound level
⭐ Clinical Pearl: The "Emergency Audiometry Triangle" - Weber lateralization to affected ear + negative Rinne + visible tympanic membrane abnormality = 95% probability of surgically correctable conductive hearing loss requiring urgent ENT consultation.
- Neurologic Red Flags (45-second screening)
- Facial nerve function: House-Brackmann grading in <30 seconds
- Spontaneous nystagmus: HINTS examination for central causes
- Cranial nerve V involvement: Gradenigo syndrome with CN VI palsy
- Complete facial paralysis: 90% chance of poor recovery without intervention
- Incomplete paralysis: 85% spontaneous recovery rate
- Associated hearing loss: 40% increased surgical indication
| Assessment Component | Normal Finding | Abnormal Threshold | Emergency Action |
|---|---|---|---|
| Facial nerve function | House-Brackmann I-II | Grade III or higher | Steroid protocol within 24h |
| Hearing assessment | <20 dB loss bilateral | >30 dB unilateral loss | Urgent audiometry |
| Tympanic membrane | Translucent, mobile | Perforation, hemotympanum | ENT consultation |
| Nystagmus pattern | None spontaneous | Vertical or rotatory | Neurology evaluation |
| CSF leak signs | No clear drainage | Glucose >30 mg/dL | Immediate imaging |
This rapid assessment framework provides the foundation for accurate triage decisions, preventing both over-treatment of benign conditions and under-recognition of surgical emergencies. Master this systematic approach to transform emergency otologic encounters from chaotic presentations into confident clinical decisions.
🎯 Rapid Assessment Arsenal: The 90-Second Diagnostic Framework
🔥 Life-Threatening Presentations: The Critical Recognition Matrix
📌 Remember: SKULL identifies intracranial complications - Seizures, Killed reflexes (altered mental status), Unsteady gait, Lethargic behavior, Leukocytosis with fever. Any component mandates immediate imaging and neurosurgical consultation.
Intracranial complications of otitis media represent the most feared otologic emergency, with mortality rates of 15-20% if treatment is delayed beyond 24 hours. These complications occur in 0.5-2% of acute otitis media cases but 10-15% of chronic otitis media with cholesteatoma.
- Intracranial Complication Patterns (<6 hour intervention window)
- Meningitis: 40% of intracranial complications
- Fever >38.5°C with neck stiffness: 85% sensitivity
- CSF pleocytosis >500 cells/μL: 90% diagnostic threshold
- Mortality rate: 10-15% with appropriate treatment
- Brain abscess: 25% of intracranial complications
- Ring-enhancing lesion on contrast CT: 95% diagnostic accuracy
- Temporal lobe location: 70% of otogenic abscesses
- Surgical drainage required if >2.5 cm diameter
- Lateral sinus thrombosis: 20% of intracranial complications
- Griesinger sign: mastoid tenderness with swelling
- Tobey-Ayer test: jugular compression increases headache
- Anticoagulation controversy: 60% of centers use heparin
- Meningitis: 40% of intracranial complications
⭐ Clinical Pearl: The "Otogenic Sepsis Triad" - chronic otitis media + altered mental status + fever >38.5°C = >90% probability of intracranial complication requiring immediate CT with contrast and neurosurgical consultation within 2 hours.
-
Malignant Otitis Externa Recognition (<4 hour intervention window)
- Demographics: >90% in diabetics or immunocompromised
- Pathognomonic sign: granulation tissue at bony-cartilaginous junction
- Pain severity: 10/10 pain disproportionate to findings
- Pseudomonas aeruginosa: 95% of causative organisms
- Skull base involvement: 60% develop cranial neuropathies
- Mortality rate: 10-50% depending on extent and comorbidities
-
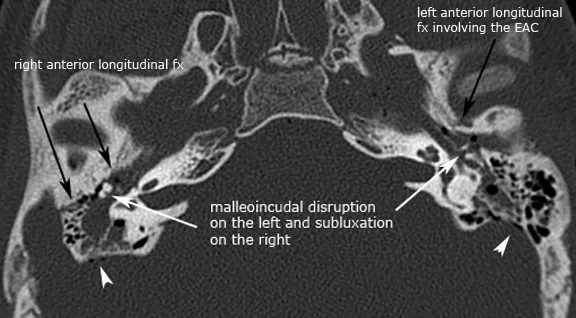
Temporal Bone Fracture Complications (<2 hour imaging window)
- CSF leak: 25% of temporal bone fractures
- Facial nerve injury: 20% immediate, 40% delayed onset
- Carotid injury: <5% but 80% mortality if missed
- Longitudinal fractures: 80% of cases, better prognosis
- Transverse fractures: 20% of cases, 90% hearing loss
- Otic capsule involvement: 100% permanent hearing loss
| Emergency Condition | Mortality Rate | Key Diagnostic Finding | Time to Intervention | Specialist Required |
|---|---|---|---|---|
| Otogenic meningitis | 10-15% | CSF pleocytosis >500 | <2 hours | Neurosurgery |
| Brain abscess | 5-10% | Ring enhancement CT | <6 hours | Neurosurgery |
| Lateral sinus thrombosis | 5-20% | MRV flow absence | <4 hours | Neurosurgery |
| Malignant otitis externa | 10-50% | Granulation tissue | <4 hours | ENT + ID |
| Carotid injury | 80% | CTA dissection | <1 hour | Vascular surgery |
Recognition of these critical patterns transforms potentially fatal presentations into manageable emergencies through prompt intervention. The key lies in maintaining high clinical suspicion and systematic evaluation protocols that prevent anchoring on benign diagnoses.
🔥 Life-Threatening Presentations: The Critical Recognition Matrix
⚡ Urgent Interventions: The Time-Critical Action Matrix
📌 Remember: URGENT time windows - Uricular hematoma (6 hours), Rapid SSNHL treatment (72 hours), Grade facial palsy steroids (24 hours), Ear foreign body removal (immediate if battery), Necrotizing otitis externa (4 hours), Temporal bone fracture evaluation (6 hours).
Sudden sensorineural hearing loss represents the most time-sensitive functional emergency, with recovery rates directly correlating to treatment initiation speed. Spontaneous recovery occurs in only 30-35% of untreated cases, while corticosteroid treatment within 72 hours improves recovery to 65-85%.
-
Sudden Sensorineural Hearing Loss Protocol (72-hour window)
- Diagnostic threshold: >30 dB hearing loss in 3 contiguous frequencies
- First-line treatment: Prednisone 1 mg/kg (max 80 mg) daily × 7 days
- Salvage therapy: Intratympanic steroids if no improvement at 2-4 weeks
- Weber test lateralizes to unaffected ear: >90% sensitivity
- MRI with gadolinium if bilateral or neurologic signs
- Hyperbaric oxygen within 3 months: 20-30% additional benefit
-
Facial Nerve Paralysis Management (24-hour steroid window)
- Complete paralysis: House-Brackmann Grade VI = <10% spontaneous recovery
- Incomplete paralysis: Grade II-V = 85% spontaneous recovery
- Steroid protocol: Prednisone 1 mg/kg daily × 10 days with taper
- Electroneuronography at 72 hours: >90% degeneration = surgery
- Bell's palsy: 70% of idiopathic cases
- Ramsay Hunt syndrome: 50% recovery rate, add acyclovir
⭐ Clinical Pearl: The "Steroid Golden Hour" principle - facial nerve paralysis and SSNHL both show exponential decline in recovery rates after 24 hours and 72 hours respectively. Early aggressive steroid therapy within these windows provides 2-3x better functional outcomes than delayed treatment.
-
Auricular Hematoma Drainage (6-hour window)
- Pathophysiology: Perichondrial separation → cartilage ischemia → necrosis
- Technique: 18-gauge needle aspiration + pressure dressing × 5-7 days
- Complications: >90% cauliflower ear if untreated beyond 6-8 hours
- Recurrence rate: 30-40% with aspiration alone
- Incision and drainage: preferred for >48 hours or recurrent
- Quilting sutures: prevent re-accumulation in >2 cm hematomas
-
Foreign Body Removal Protocols (Immediate if button battery)
- Button batteries: tissue necrosis begins within 15 minutes
- Safe removal depth: <6 mm from external auditory meatus
- Contraindications: vegetable matter (swells), sharp objects, deep location
- Irrigation contraindicated: if tympanic membrane perforation suspected
- General anesthesia: required for >50% of pediatric cases
- ENT consultation: mandatory if >2 failed attempts
| Urgent Condition | Time Window | Treatment Success Rate | Delayed Treatment Outcome | Key Intervention |
|---|---|---|---|---|
| SSNHL | 72 hours | 65-85% recovery | 30-35% recovery | Oral prednisone |
| Facial nerve paralysis | 24 hours | 85% recovery | 10-60% recovery | Steroid therapy |
| Auricular hematoma | 6 hours | 95% normal appearance | 90% cauliflower ear | Drainage + pressure |
| Button battery | 15 minutes | No tissue damage | Severe necrosis | Immediate removal |
| Perilymphatic fistula | 48 hours | 70% symptom resolution | 30% permanent vertigo | Bed rest + surgery |
Understanding these time-critical interventions enables emergency physicians to make appropriate triage decisions and initiate treatment protocols that preserve function and prevent permanent disability. The key lies in recognizing the narrow therapeutic windows and acting decisively within them.
⚡ Urgent Interventions: The Time-Critical Action Matrix
🧭 Differential Diagnosis Navigation: The Pattern Recognition Engine
📌 Remember: PATTERN recognition - Pain severity assessment, Age and risk factors, Timing and onset, Tympanic membrane appearance, External canal findings, Red flag symptoms, Neurologic involvement. This systematic approach prevents diagnostic anchoring.
The "Red Flag vs. Green Light" framework rapidly stratifies presentations into high-risk and low-risk categories. Red flag features mandate immediate specialist consultation, while green light findings allow emergency department management with appropriate follow-up.
-
Vertigo Differential Matrix (HINTS examination critical)
- Peripheral vertigo (vestibular neuritis): 85% of emergency presentations
- Horizontal nystagmus: beats away from affected side
- Head impulse test: positive (corrective saccade)
- Test of skew: negative (no vertical misalignment)
- Central vertigo (stroke): 15% but high mortality if missed
- Vertical or rotatory nystagmus: >90% central origin
- Negative head impulse: >95% central lesion
- Positive test of skew: >90% brainstem involvement
- Peripheral vertigo (vestibular neuritis): 85% of emergency presentations
-
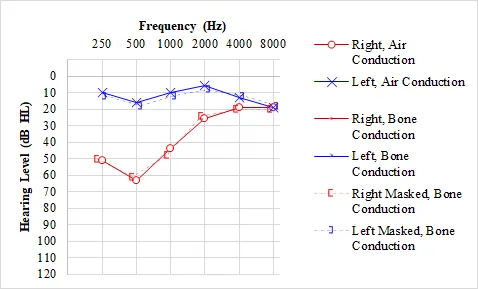
Hearing Loss Pattern Recognition (Weber and Rinne interpretation)
- Conductive loss: Weber lateralizes to affected ear, Rinne negative
- Cerumen impaction: 40% of emergency hearing complaints
- Ossicular disruption: Weber >20 dB lateralization
- Tympanic membrane perforation: visible on otoscopy
- Sensorineural loss: Weber lateralizes away, Rinne positive both ears
- Sudden onset: SSNHL until proven otherwise
- Gradual onset: presbycusis or noise-induced
- Bilateral: ototoxicity or autoimmune causes
- Conductive loss: Weber lateralizes to affected ear, Rinne negative
⭐ Clinical Pearl: The "Rule of Asymmetry" - any unilateral otologic symptom (hearing loss, tinnitus, vertigo, facial weakness) requires urgent evaluation to exclude retrocochlear pathology, especially acoustic neuroma or cerebellopontine angle tumors.
- Ear Pain Differential Hierarchy (severity and character guide diagnosis)
- Mild-moderate pain (1-6/10): typically infectious causes
- Otitis externa: swimming history, tragal tenderness
- Acute otitis media: bulging tympanic membrane, fever
- Referred pain: TMJ, dental, cervical sources
- Severe pain (7-10/10): consider serious pathology
- Malignant otitis externa: diabetic, granulation tissue
- Temporal arteritis: >50 years, ESR >50
- Trigeminal neuralgia: sharp, electric quality
- Mild-moderate pain (1-6/10): typically infectious causes
| Symptom Complex | Benign Cause | Serious Cause | Key Discriminator | Immediate Action |
|---|---|---|---|---|
| Acute vertigo | Vestibular neuritis | Posterior stroke | HINTS examination | Neurology if central |
| Unilateral hearing loss | Cerumen impaction | SSNHL | Weber lateralization | Steroids if SSNHL |
| Severe ear pain | Acute otitis media | Malignant OE | Granulation tissue | ENT if granulation |
| Facial weakness | Bell's palsy | Temporal bone tumor | Gradual vs sudden | MRI if gradual |
| Ear drainage | Otitis externa | CSF leak | Glucose testing | Neurosurgery if CSF |
This pattern recognition framework enables rapid, accurate diagnosis while preventing both over-investigation of benign conditions and under-recognition of serious pathology. The key lies in systematic application of discriminating features that reliably distinguish between similar presentations.
🧭 Differential Diagnosis Navigation: The Pattern Recognition Engine
🎯 Emergency Management Protocols: The Rapid Response Playbook
📌 Remember: TREAT protocol - Time-sensitive interventions first, Risk stratification, Evidence-based medications, Appropriate specialist consultation, Targeted follow-up planning. This sequence prevents missed interventions and ensures comprehensive care.
Corticosteroid protocols represent the cornerstone of emergency otologic management, with specific dosing regimens proven effective for sudden sensorineural hearing loss, facial nerve paralysis, and autoimmune inner ear disease. Timing is critical - delayed steroid administration significantly reduces efficacy.
-
Corticosteroid Management Protocols
- Sudden SSNHL: Prednisone 1 mg/kg (max 80 mg) daily × 7 days
- Alternative: Methylprednisolone 1.6 mg/kg daily if GI intolerance
- Contraindications: active infection, uncontrolled diabetes
- Monitoring: glucose levels in diabetics, blood pressure in hypertensives
- Facial nerve paralysis: Prednisone 1 mg/kg daily × 10 days with taper
- Taper schedule: full dose × 5 days, then decrease 10 mg daily
- Add acyclovir: 800 mg 5x daily if Ramsay Hunt syndrome
- Eye protection: artificial tears, taping if incomplete closure
- Sudden SSNHL: Prednisone 1 mg/kg (max 80 mg) daily × 7 days
-
Antibiotic Selection Matrix (pathogen-directed therapy)
- Acute otitis media: Amoxicillin 875 mg BID × 7-10 days
- Penicillin allergy: Azithromycin 500 mg daily × 3 days
- Treatment failure: Amoxicillin-clavulanate 875/125 mg BID
- Severe disease: Ceftriaxone 1-2 g daily × 3 days
- Otitis externa: Ciprofloxacin-dexamethasone drops 4 drops BID × 7 days
- Severe cellulitis: Ciprofloxacin 500 mg BID PO × 7-10 days
- Diabetic patients: consider malignant OE, urgent ENT consultation
- Acute otitis media: Amoxicillin 875 mg BID × 7-10 days
⭐ Clinical Pearl: The "Steroid-Antibiotic Rule" - never delay steroids for SSNHL or facial paralysis to obtain cultures or additional testing. Start treatment immediately based on clinical diagnosis, as every hour of delay reduces recovery probability by 1-2%.
-
Pain Management Protocols (multimodal approach)
- Mild-moderate pain (1-6/10): Ibuprofen 600 mg q6h + acetaminophen 1000 mg q6h
- Severe pain (7-10/10): Oxycodone 5-10 mg q4-6h + NSAIDs
- Topical anesthetics: Benzocaine drops for external canal pain
- Avoid topical anesthetics if tympanic membrane perforation
- Heat therapy: warm compress × 15-20 minutes q2-4h
- Positioning: affected ear up to promote drainage
-
Emergency Procedures (technique-specific protocols)
- Auricular hematoma drainage: 18-gauge needle, complete evacuation
- Pressure dressing: dental rolls + head wrap × 5-7 days
- Prophylactic antibiotics: Cephalexin 500 mg QID × 5 days
- Follow-up: 24-48 hours for re-accumulation check
- Foreign body removal: direct visualization, <2 attempts
- Contraindications: vegetable matter, button batteries >15 min
- Irrigation: only if intact tympanic membrane
- ENT consultation: immediate if unsuccessful removal
- Auricular hematoma drainage: 18-gauge needle, complete evacuation
| Clinical Scenario | First-Line Treatment | Dosing Regimen | Duration | Follow-up Timing |
|---|---|---|---|---|
| SSNHL | Prednisone | 1 mg/kg daily (max 80mg) | 7 days | 48-72 hours |
| Facial paralysis | Prednisone | 1 mg/kg daily × 10 days | Taper over 15 days | 72 hours |
| Acute otitis media | Amoxicillin | 875 mg BID | 7-10 days | 48-72 hours |
| Otitis externa | Cipro-dex drops | 4 drops BID | 7 days | 3-5 days |
| Auricular hematoma | Needle drainage | Complete evacuation | Single procedure | 24 hours |
These evidence-based protocols provide the framework for consistent, optimal emergency otologic care while ensuring appropriate specialist consultation and follow-up planning. Master these protocols to transform emergency otologic encounters into systematic, successful interventions.
🎯 Emergency Management Protocols: The Rapid Response Playbook
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app












