Inner Ear GPS - Anatomy's Grand Design
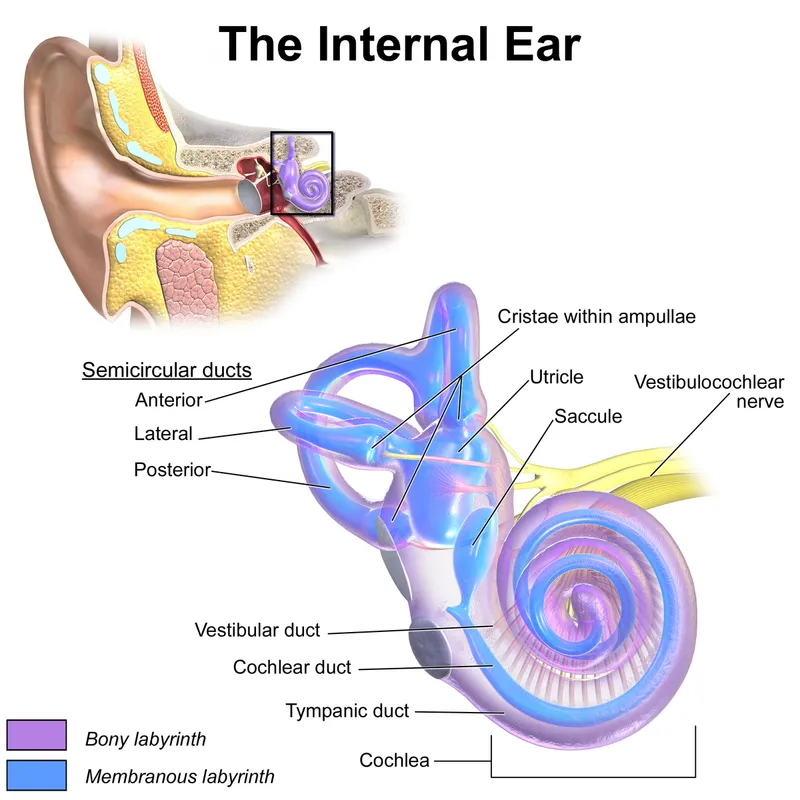
- Vestibular Labyrinth: Bony & Membranous parts within petrous temporal bone.
- Bony Labyrinth: Houses membranous labyrinth; contains perilymph.
- Vestibule: Central part; contains utricle & saccule.
- Semicircular Canals (SCCs): Superior (Anterior), Posterior, Lateral (Horizontal). Detect angular acceleration. Each has a dilated end (ampulla).
- Membranous Labyrinth: Suspended within bony labyrinth; contains endolymph.
- Utricle & Saccule (Otolith Organs): Located in vestibule. Detect linear acceleration & head position relative to gravity.
- Semicircular Ducts: Within SCCs; connect to utricle.
- Endolymphatic Duct & Sac: Projects from utricle/saccule; involved in endolymph homeostasis.
- Bony Labyrinth: Houses membranous labyrinth; contains perilymph.
- Sensory Receptors: Hair cells.
- Maculae: Sensory areas in utricle & saccule.
- Contain otoconia (calcium carbonate crystals) embedded in otolithic membrane overlying hair cells.
- Utricular macula: primarily horizontal plane.
- Saccular macula: primarily vertical (sagittal) plane.
- Cristae Ampullaris: Sensory areas in ampullae of SCCs.
- Gelatinous, dome-shaped cupula overlying hair cells; no otoconia.
- Detects endolymph movement during angular acceleration.
- Maculae: Sensory areas in utricle & saccule.
⭐ The lateral (horizontal) SCC is tilted approximately 30° superiorly from the horizontal plane when the head is in the anatomical position (Frankfurt plane).
Hair Cell Hype - Motion to Message
Vestibular hair cells, mechanoreceptors in the utricle, saccule, and semicircular canal ampullae, convert head motion into neural signals. Each cell has a polarized bundle of stereocilia and a single kinocilium.
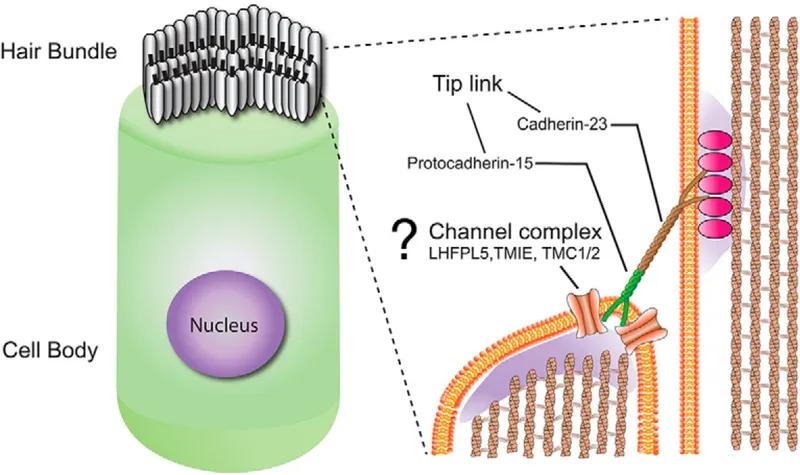
- Core Structure & Function:
- Stereocilia: ~50-100 actin-rich projections, graded in height, alongside a single, taller kinocilium.
- Tip Links: Connect stereocilia tips. Tension on tip links opens/closes MET (Mechano-Electrical Transduction) channels.
- MET Channels: Non-selective cation channels, primarily permeable to K⁺ from endolymph.
- Mechanoelectrical Transduction:
- Ionic Environment:
- Apical surface bathed in K⁺-rich endolymph (~150 mM K⁺, +80mV endocochlear potential).
- Basolateral surface in normal perilymph (low K⁺).
- 📌 King K⁺ drives depolarization (K⁺ influx) and repolarization (K⁺ outflux via basolateral channels).
⭐ Vestibular hair cells have a resting discharge. Deflection towards the kinocilium increases firing rate; deflection away decreases it. This bidirectional response allows precise encoding of head movement.
Brain's Balancing Crew - Reflexes & Relays
- Central Hub: Vestibular Nuclear Complex (VNC)
- Located in brainstem; comprises superior, medial, lateral (Deiters'), and inferior nuclei.
- Primary processing centers for inputs from SCCs & otoliths.
- Integrates vestibular, visual, & proprioceptive information for a cohesive sense of balance.
- Key Reflexes for Stability:
- Vestibulo-Ocular Reflex (VOR): Maintains stable vision during head movements, ensuring gaze remains fixed on a target.
- VOR gain (eye velocity / head velocity) ≈ 1.0.
- Classic three-neuron arc: Vestibular nerve → Vestibular nuclei → Oculomotor nuclei.
- Vestibulospinal Reflex (VSR): Adjusts body posture via lateral & medial vestibulospinal tracts, maintaining upright stance.
- Vestibulocollic Reflex (VCR): Acts on neck musculature to stabilize the head.
- Vestibulo-Ocular Reflex (VOR): Maintains stable vision during head movements, ensuring gaze remains fixed on a target.
- Crucial Pathways & Modulators:
- Medial Longitudinal Fasciculus (MLF): Major brainstem tract connecting VNC to oculomotor (III), trochlear (IV), & abducens (VI) nuclei; critical for coordinating conjugate eye movements in VOR.
- Cerebellum (esp. Flocculonodular Lobe & Vermis): Modulates VOR & VSR, crucial for calibration, motor learning, and adaptation of balance reflexes; fine-tunes movements.
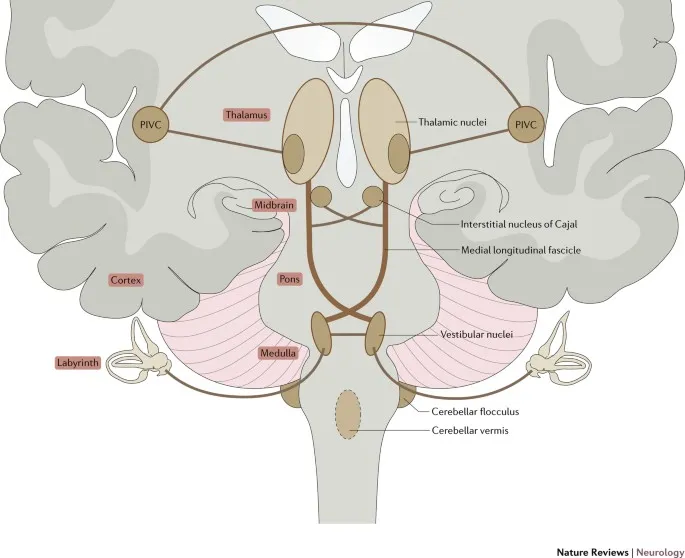
⭐ The VOR gain is normally close to 1.0. A gain significantly less than 1.0 results in retinal slip and oscillopsia (illusory movement of the visual world), a common complaint in bilateral vestibular loss.
High‑Yield Points - ⚡ Biggest Takeaways
- The vestibular system, comprising semicircular canals, utricle, and saccule, is crucial for maintaining balance.
- Semicircular canals detect angular acceleration (head rotation); otolith organs (utricle and saccule) detect linear acceleration and head tilt.
- Sensory receptors are cristae ampullaris in semicircular canals and maculae in utricle/saccule.
- Hair cell deflection: towards kinocilium causes excitation (depolarization); away causes inhibition.
- The Vestibulo-Ocular Reflex (VOR) stabilizes gaze during head movements, ensuring clear vision.
- Nystagmus, an involuntary rhythmic oscillation of the eyes, is a key sign of vestibular dysfunction.
- Caloric testing (COWS mnemonic: Cold Opposite, Warm Same) assesses peripheral vestibular function by inducing nystagmus.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

